Study Finds Sex Differences in Mental Illness Posted July 5th 2020
Men more likely to develop substance abuse, antisocial problems; women more likely to develop anxiety, depression
Related
WASHINGTON—When it comes to mental illness, the sexes are different: Women are more likely to be diagnosed with anxiety or depression, while men tend toward substance abuse or antisocial disorders, according to a new study published by the American Psychological Association.
Published online in APA’s Journal of Abnormal Psychology®, the study looked at the prevalence by gender of different types of common mental illnesses. The researchers also found that women with anxiety disorders are more likely to internalize emotions, which typically results in withdrawal, loneliness and depression. Men, on the other hand, are more likely to externalize emotions, which leads to aggressive, impulsive, coercive and noncompliant behavior, according to the study. The researchers demonstrated that it was differences in these liabilities to internalize and to externalize that accounted for gender differences in prevalence rates of many mental disorders.
Researchers analyzed data collected in 2001 and 2002 by a National Institutes of Health survey of 43,093 U.S. residents 18 and older who were civilians and not institutionalized. Of those, 57 percent were women and 56.9 percent were white; 19.3 percent were Hispanic or Latino; 19.1 percent were African-American; 3.1 percent Asian, native Hawaiian or Pacific Islander; and 1.6 percent were American Indian or native Alaskan. The data were representative of the age, race/ethnicity and gender distributions of the U.S. population in the 2000 Census. Participants answered interview questions. The analysis examined their lifetime mental health history as well as over the prior 12 months.
The authors cited previous research that found women suffer more than men from depression, because “women ruminate more frequently than men, focusing repetitively on their negative emotions and problems rather than engaging in more active problem solving.”
The findings support gender-focused prevention and treatment efforts, the study said. “In women, treatment might focus on coping and cognitive skills to help prevent rumination from developing into clinically significant depression or anxiety,” said lead author Nicholas R. Eaton, MA, of the University of Minnesota. “In men, treatment for impulsive behaviors might focus on rewarding planned actions and shaping aggressive tendencies into non-destructive behavior.”
Past research also indicated that women report more neuroticism and more frequent stressful life events than men do before the onset of a disorder, indicating that environmental stressors may also contribute to internalizing, the report said.
Article: “An Invariant Dimensional Liability Model of Gender Differences in Mental Disorder Prevalence: Evidence from a National Sample,” Nicholas R. Eaton, MA, and Robert. F. Krueger, PhD, University of Minnesota; Katherine M. Keyes, PhD, and Deborah S. Hasin, PhD, Columbia University; Steve Balsis, PhD, Texas A&M University; Andrew E. Skodol, MD, Columbia University and University of Arizona; Kristian E. Markon, PhD, University of Iowa; Bridget F. Grant, PhD, National Institute on Alcohol Abuse and Alcoholism; Journal of Abnormal Psychology, Vol. 121, No. 1.
Nicholas R. Eaton can be contacted by email or at (314) 954-1270
The American Psychological Association, in Washington, D.C., is the largest scientific and professional organization representing psychology in the United States and is the world’s largest association of psychologists. APA’s membership includes more than 154,000 researchers, educators, clinicians, consultants and students. Through its divisions in 54 subfields of psychology and affiliations with 60 state, territorial and Canadian provincial associations, APA works to advance psychology as a science, as a profession and as a means of promoting health, education and human welfare.
When Women Are More Likely to Lie
A new study reveals how gender and social pressure drive unethical decisions.
By Pamela Tom | October 24, 2016
Would you tell a lie to help someone else? A new study says women won’t lie on their own behalf, but they are willing to do so for someone else if they feel criticized or pressured by others.
In contrast, research by Professor Laura Kray of UC Berkeley and Assistant Professor Maryam Kouchaki of Northwestern University found that men are the opposite: They do not compromise their ethical standards under social pressure regardless of whether they’re advocating for themselves or anyone else.

“We found that when women act on their own behalf, they maintain higher ethical standards than men. However, women will act less ethically, such as telling a lie, when they fear being viewed as ineffective at representing another person’s interests,” says Kray. “When women negotiate on behalf of someone else, they are willing to make compromises in order to satisfy the needs of others.”
But at what cost?
Kray says there’s a tradeoff for women, who face a “Catch 22.” Men are typically less constrained by social expectations. But when women are asked to advocate for others, they face a conflict because they must either relinquish or reduce their usual moral standards, or open themselves up to possible social backlash.
The authors write, “They are damned if they lie because it goes against their communal mandate with respect to their negotiating counterpart, however they are damned if they do not lie because it goes against their communal mandate with respect to the party they are representing.”
The findings are a result of four studies, each involving from 160 to 235 participants.
In the first study, participants were assigned either self-advocacy or friend-advocacy roles and asked to consider the appropriateness of various negotiating tactics. As hypothesized, women who negotiated on behalf of someone else were less ethical than when advocating for themselves.
The second study was designed to better understand the psychological process behind unethical negotiating tactics. Participants advocating for others answered questions about how much they anticipated social backlash if they did not reduce their ethical standards to help others. For example, “How much would your friends like to socialize with you?” and “How likely would your colleagues be to go with you if you invited them out for drinks after work?” The findings were the same as in the first study. However, women were not found to completely disregard—only lower—their moral obligations regardless of whether they were advocating for themselves or others.
“This suggests that women did not see unethical tactics as more acceptable when helping others but instead, they lowered their ethical standards because they felt pressured to do so,” says Kray.
The third study focused on the anticipation of social backlash. Female participants were asked to read a description of a salary negotiation from a self-advocacy perspective; for example, as new recruits negotiating their own starting salary. They also read a description depicting an other-advocacy situation such as a friend negotiating salary on behalf of a new recruit whom she referred for the position. The ethical dilemma of each script is whether to tell the hiring manager that they (or the friend) had another job offer even though one didn’t really exist. The alternative option was to be honest with the hiring manager and tell him that they (or the friend) had no other job offers. Women were more inclined to lie when negotiating for the friend.
In the final study, the authors recruited participants to complete an actual negotiation and assigned them to be either a property seller or a buyer. In the scenario, the seller wants to sell to a buyer who would retain the property for residential use. However, buyers were instructed that their intent was to turn the property into a high-rise, commercial building against the wishes of the seller. Would those negotiating on behalf of the buyer be deceptive as a result of social pressure? Again, women who chose to be dishonest expected greater social backlash when negotiating for themselves than on behalf of others. And women who chose not to lie anticipated greater backlash when representing someone else’s interests.
Across all studies including men, the men’s ethics were not affected whether they represented themselves or another person. Also, their ethical standards were lower than women representing themselves.
The study’s results may appear disturbing to women who are trying to do the right thing, but Kray contends that when considering whether to compromise one’s usual ethics, consider the particular situation. Women may be unaware that they have this tendency to lower their moral standards when trying to help others.
“Ask yourself, ‘What are the constraints and social pressures? If I was doing this for myself or someone else, how would I act differently?” says Kray.
This article was originally published on Haas Now. Read the original article.
The hysteria accusation
Women’s pain is often medically overlooked and undertreated. But the answer is not as simple as ‘believing all women’ July 5th 2020
Pain is your body’s alarm system. It’s a sensation designed to tell you that something’s gone wrong. But being in pain, says Colin Klein, a philosopher at the Australian National University, is a bit like having your house guarded by a hyperactive terrier. Sometimes it barks at trespassers, but other times it gets upset at the postman. Sometimes it goes wild over nothing at all, and, on occasion, it would probably let in burglars if they brought snacks. Pain is correlated with tissue damage (the stuff you need protecting from), but the two don’t necessarily go together. If you’ve ever cut yourself and didn’t feel the slightest twinge until you saw blood, you’ve had tissue damage without pain. If you’ve ever felt a sting in anticipation of an injection or a dentist’s drill, you’ve had pain without tissue damage.
Part of what makes pain an effective protection mechanism also makes it inherently subjective. The International Association for the Study of Pain describes it as ‘an unpleasant sensory and emotional experience’. You wouldn’t jerk your hand back so quickly from a hot stove if pain was just a vaguely irritating tickle. Pain can protect us because we typically dislike it and find it emotionally distressing.
This affective dimension of pain – which we might also call its ‘interpretive’ or ‘psychological’ character – becomes especially complex when it intersects with gender. There’s good evidence that the modern Western medical system treats men and women’s pain quite differently. Women are more likely to have their pain dismissed or under-treated, often from a very young age. That’s especially true for women of colour, whose pain receives significantly less treatment than that of their white peers. Clinicians investigate women’s chest pain less frequently than men’s – even when women have all the classic symptoms of a heart attack, and even though heart disease is the leading cause of death in women. Women are also far more likely than men to have a physical illness misdiagnosed as a psychiatric condition, particularly depression.
One reason for these problems is that we don’t listen carefully when women talk about their lives and experiences. Women are often subject to what the philosopher Miranda Fricker at the City University of New York has called a credibility deficit: they’re treated as less reliable sources of information, precisely because stereotypes cast women as untrustworthy and irrational. As a result, society’s understanding of things such as workplace harassment, sexual violence and intimate partner violence is profoundly skewed, since we’re less likely to believe reports from the people most likely to be affected.
This credibility deficit makes women’s descriptions of their own lives a feminist issue. Feminists are more than justified in urging us to #BelieveWomen, as the Twitter hashtag puts it. Pain, though, is a particularly interesting case, because it reveals the limitations of this simple and compelling call. The demand that we recognise women’s pain is justified and necessary. But the way this demand plays out risks inadvertently reinforcing a deep-seated social bias about the hierarchy of psychological versus physical suffering – and doing so in a way that hurts women once again
There’s a Dark Side to Meditation That No One Talks About
Meditation can bring about a wide variety of thoughts and emotions—some are peaceful, others are not.
- Lila MacLellan

The calm before the panic attack.
We’ve all heard about the benefits of meditation ad nauseam. Those disciplined enough to practice regularly are rewarded with increased control over the brainwaves known as alpha rhythms, which leads to better focus and may help ease pain. In addition to calming the mind and body, meditation can also reduce the markers of stress in people with anxiety disorders. Rigorous studies have backed health claims such as these to convince therapists, physicians, and corporate gurus to embrace meditation’s potential.
What contemporary and ancient meditators have always known, however, is that while the hype may be warranted, the practice is not all peace, love, and blissful glimpses of unreality. Sitting zazen, gazing at their third eye, a person can encounter extremely unpleasant emotions and physical or mental disturbances.
Zen Buddhism has a word for the warped perceptions that can arise during meditation: makyo, which combines the Japanese words for “devil” and “objective world.” Philip Kapleau, the late American Zen master, once described confronting makyo as “a dredging and cleansing process that releases stressful experiences in deep layers of the mind.”
However, this demanding and sometimes intensely distressing side of meditation is rarely mentioned in scientific literature, says Jared Lindahl, a visiting professor of religious studies at Brown University, who has an interest in neuroscience and Buddhism. Along with Willoughby Britton, a psychologist and assistant professor of psychiatry at Brown, the two meditators have co-authored a study that documents and creates a taxonomy for the variant phenomenology of meditation. The paper, published in Plos One, is the beginning of an ongoing series of studies. “Just because something is positive and beneficial doesn’t mean we shouldn’t be aware of the broader range of possible effects it might have,” Lindahl says.
To conduct their research, the pair interviewed 60 Western Buddhist meditation practitioners who had all experienced challenging issues during their practice. They included both rookies and meditation teachers, many of whom had accumulated more than 10,000 hours of meditation experience in their lifetime. All belonged to either Theravāda, Zen, or Tibetan traditions.
The researchers identified 59 kinds of unexpected or unwanted experiences, which they classified into seven domains: cognitive, perceptual, affective (related to moods), somatic, conative (related to motivation), sense of self, and social. Among the experiences described to them were feelings of anxiety and fear, involuntary twitching, insomnia, a sense of complete detachment from one’s emotions, hypersensitivity to light or sound, distortion in time and space, nausea, hallucinations, irritability, and the re-experiencing of past traumas. The associated levels of distress and impairment ranged from “mild and transient to severe and lasting,” according to the study. Most would not imagine that these side-effects could be hiding behind the lotus-print curtains of your local meditation center.
However, the survey respondents didn’t necessarily perceive every non-euphoric event as negative. In fact, says Britton, she and Lindahl deliberately avoided the word “adverse” in their study for this reason. Instead, they chose “challenging,” which better captured the meditators’ varied interpretations of their experiences. For instance, a person who came away from a retreat feeling “very expanded and very unified with other people in the world” might have found their oneness with the universe distracting once they returned home. (That’s challenging, not tragic.)
The goal of the study was to look for patterns in the common accounts of unwanted reactions. Who runs into the unexpected hurdles? What are the unique set of factors involved? In which ways do teachers assist students who are struggling? (And do they blame inner demons for the upsets, or maybe something you ate at lunch?) The answers, which still require future research, may one day be relevant to the ways meditation is used as therapy.
More from Quartz
- Mindfulness fixes your brain while boosting your performance510 saves
- ‘Sleeping on it’ really is the smartest way to solve a problem94 saves
- The easiest way to lucid dream, according to science637 saves
Advertisement
The Psychology Behind Why Some People Wear Face Masks – And Others Don’t
Confusion, embarrassment, discomfort. Psychologists tell HuffPost UK what may stop people wearing a mask.By Natasha Hinde30/06/2020 12:12pm BST | Updated 3 hours ago
Face masks are quite divisive among Brits. When you look at photos of people hitting the beach, rushing to stores or taking buses in England where masks are mandatory, there’s a split of those who wear them – and those who don’t.
A YouGov poll from June suggests more people aren’t wearing them than are. It found under a quarter (21%) of Brits wear a mask or cover when out in public. We’re less likely to wear them than many other countries, too – only those in Scandinavia and Australia are less likely to wear masks than Brits, the poll found.
It’s a topic that needs exploring, perhaps, as research suggests a lockdown on its own won’t be enough to stop a second wave of coronavirus. Researchers believe the widespread use of face masks, in addition to lockdown and social distancing, is key to keeping the reproduction rate below 1.
So why are some people happy to wear face masks, but others aren’t? We asked psychologists.
Related…
We Tested 5 Ways To Wear Makeup That Won’t Gunk Up Your Face Mask

Physical (dis)comfort
Professor Tony Cassidy, an expert in child and family health psychology at Ulster University, believes comfort – or rather, discomfort – is a key factor. Some might have a mask that fits comfortably, but, he tells HuffPost UK, “masks can be too tight or loose and they can cause sweating or even difficulty breathing”.
This means anyone who is claustrophobic or maskaphobic will be unable to tolerate masks or face coverings. “Maskaphobia [a fear of masks] is surprisingly common among children,” he adds.
Feeling self-conscious
A YouGov survey in partnership with Imperial College London, conducted in May, looked at what was putting people off wearing masks. Of those who didn’t wear one, the vast majority (76%) said it was due to concerns about feeling uncomfortable – as Prof Cassidy mentioned above.
But many people also felt self conscious (52%), silly (52%) and embarrassed (47%) about wearing a mask.
Not being able to communicate
Masks, or face covers, can also be quite intrusive – “eating an ice cream or having a drink is impeded,” says Prof Cassidy.
When our faces are half-covered by masks, we lose key non-verbal information, Professor Kathleen Pike, an expert in psychology at Columbia University, explained in a blog post on mask-wearing. We also lose other information, like raised eyebrows, and shoulder shrugs become highly ambiguous without cues from the mouth.
“The effect leaves us feeling less able to communicate and less able to understand each other,” she wrote.

Confusion about whether they work
There’s been a lack of consistency in information about mask wearing and their benefits, and this has led to confusion, explains Prof Cassidy. The UK government didn’t recommend the use of face covers until almost two months into lockdown – and even then, it was a tentative recommendation.
Back in March, the deputy chief medical officer Jenny Harries said of masks: “For the average member of the public wandering down the street, it is really not a good idea.” Since then, the government has not only recommended their use in places where social distancing is difficult to manage, but has made wearing them mandatory on public transport and in hospitals in England.
The latest government line is that face coverings provide some “small additional protection” to others and prevent people spreading the virus if they’re asymptomatic.
A threat to freedom
Reluctance to wear a mask could be a replay of what happened in previous pandemics, suggests Professor Steven Taylor, a clinical psychologist at the University of British Columbia and author of The Psychology Of Pandemics.
“During the ‘Spanish flu’ pandemic in 1919 in San Francisco, for example, the Anti-Mask League was formed, in reaction to efforts by local government to make it mandatory to wear face masks,” he says.
The objections raised against wearing face masks were similar to those we see today, Prof Taylor says: 1) concern there isn’t strong evidence that masks are protective, and 2) that the mandatory wearing of them is perceived by some as a threat to their freedom. “In highly individualistic societies, attempts to compel people to do things can lead to pushback when people perceive their liberties to be threatened,” he explains.
This is known as psychological reactance. Some people have little reactance, while others have a lot. “The people strongly opposed to wearing face masks are also likely to oppose other threats to their freedom, such as enforced social distancing protocols,” says Prof Taylor.
Some “macho individuals” also worry about being perceived as weak if they wear masks, he adds, and believe it’s an admission of fear and vulnerability.
Related…
Can’t Wear A Face Mask For Health Reasons? Carry This Card Instead
Racism and racial profiling
Dr Mollie Ruben, a research assistant professor at Northeastern University who is researching the psychological effects of mask wearing in the US, says some people don’t feel safe wearing masks due to racial profiling.
In the US, an Oregon county made people of colour exempt from its mandatory mask policy – citing the potential for racial profiling. However, the exemption was removed after a backlash. “The very policy meant to protect them, is now making them a target for further discrimination and harassment,” leaders said.
Prof Taylor also says people with racist attitudes may be reluctant to wear masks “because mask-wearing is perceived as being an Asian cultural practice”.
Perceived risk
Prof Taylor believes some people – younger adults, he says – perceive the risk of Covid-19 as being “overblown”.
“If people see the risk as overblown, then they are unlikely to comply with wearing face masks,” he says. “Some people underestimate the seriousness of Covid-19 because this pandemic, unlike previous pandemics is largely hidden.”
Taylor believes if political leaders lead by example, there might be a shift in public perception of wearing masks in the UK. “The behaviour of our leaders has a powerful influence on the behaviour of the populace,” he says.
“If our community leaders want to increase the use of mask wearing in the UK, US, or elsewhere, they should label mask wearing as an act of community spirit, solidarity, and patriotism. That is, you’re serving your community and your country if you do your bit to reduce infection by wearing a mask.”
Abuse can lead to suicidal thoughts – Robert Cook June 30th 2020
Covid 19 and ludicrous lockdown has affected many of us, while helping the elite and police to make even more money – matters covered on other pages.
Because I , and my eldest son, have been on the receiving end of serious criminal abuse and misconduct by the British Police and NHS, I have spent the last three months seriously considering suicide. My ex wife’s physical and menatl abuse, along woith her abuse of my late mother and youngest son. led me to feelings of utter wothlessness in March 2007, when I nearly scceeded in hanging myself. The police refused to investigate my allegations from the outset 12 years ago, labelling me as mentally ill, then taking me to court four prosecutions and nearly 30 separate hearings, to get me jailed. Four of these hearings followed me swearing at an acting CID officer who took vital documents in a bogus and malicious 7 officer raid, keeping my property for over three months. He claimed to be distressed by my messages, left because he was always unavaible. That case, which involved allegations of me being involved as a gay prostitute working for my son in a brothel at my home. Adding insult to injury, I was accused of sending incriminating material, which turned out to be faked, to senior police officers and my ex inlaws. Polce still refuse to explain this.
My ex wife’s peculiar interest in my youngest son, washing and taking him to the toiler right up until she took hin from this house, had dreadful impact on me over several years. She told me she could do as she liked and that her brother would use his high police rank to deal with me.
Because my eldest son would not go with her and my youngest vulnearble son, my ex wife locked him out of his student home and put the house he had paid for in her name, effectively stealing his £20,000 depoist money and two years of mortgage payments. She also went on to band my eldest son from seeing his brother, telling the police that my eldest son was violent like me. Because she is a woman and sister of a high ranking police officer, she was beleived, my son and I being criminalised without investigation – as West Mercia have admitted in writing.
The fall out from this caused my mother’s death. There was also the issue of spreading lies about myself and eldest son. leading to acts of physical and verbal violence and social ostracism.
With three police forces backing my in laws lies, I have been plunged into a sense of utter hopelssness, made worse by the police inisting to the NHS that I am paranoid schoziphenic and deluded.
A situation like that is unbeleivable to specialists who are poorly trained and part of the system – so I know that messages like the official one below is pretty useless for people in my situation because mental health specialists never challenge the corrupt system of which they are a part. When officials lie about us, they define us to others, sometimes provoking their vctims toward insanity and suicide. Robert Cook
Are you thinking about suicide? How to stay safe and find treatment
Hopelessness may lead you to think about suicide. Learn how to stay safe, get through a crisis and find treatment.By Mayo Clinic Staff
When life doesn’t seem worth living anymore, it may seem that the only way to find relief is through suicide. When you’re feeling this way, it may be hard to believe, but you do have other options.
Take a step back and separate your emotions from your actions for the moment.
- Recognize that depression and hopelessness can distort your perceptions and reduce your ability to make good decisions.
- Realize that suicidal feelings are the result of treatable problems.
- Act as if there are other options instead of suicide, even if you may not see them right now.
It may not be easy, and you might not feel better overnight. Eventually, though, the sense of hopelessness — and thoughts of suicide — will lift.
Get immediate help
If you think you may hurt yourself or attempt suicide, get help right away by taking one of these actions:
- Call your mental health specialist.
- Call a suicide hotline number — in the United States, call the National Suicide Prevention Lifeline at 800-273-TALK (800-273-8255) to reach a trained counselor. Use that same number and press 1 to reach the Veterans Crisis Line.
- Call 911 or your local emergency number.
- Seek help from your doctor or other health care provider.
- Reach out to a close friend or loved one.
- Contact a minister, spiritual leader or someone else in your faith community.
Learn coping strategies
Don’t try to manage suicidal thoughts or behavior on your own. You need professional help and support to overcome the problems linked to suicidal thinking.
Your doctor or mental health provider can help you identify coping strategies tailored to your specific situation. Consider discussing these coping strategies with people who know you well, such as family members or trusted friends.
You may be advised to do things you don’t feel like doing, such as talking with friends when you’d rather stay in your bedroom all day. It will get easier to do such things as they become habits.
Make a plan for life
Create a written plan of action or a “safety plan” with your mental health provider that you can refer to when you’re considering suicide or in a crisis. Learn to spot your warning signs early, so you can put your plan into action.
Your plan is a checklist of activities and actions you promise to do, so you can stay safe when you have thoughts of suicide, such as:
- Contact your doctor, therapist or crisis center to help you cope with suicidal thoughts
- Call a supportive family member or friend who can help you cope with your suicidal thoughts
- Try specific healthy and enjoyable activities when negative thoughts start to intrude
- Review why your life is valuable and the reasons to live
Even if the immediate crisis passes with your self-care strategies, see a doctor or mental health provider. This will help you get appropriate treatment for suicidal thoughts and feelings so that you don’t have to continually operate in a crisis mode.
As a foundation for your plan, take these steps:
- Stick with your treatment plan. Commit to taking your medication as prescribed and attending all treatment sessions and appointments.
- Keep a list of contact names and numbers readily available. Include your doctors, therapists and crisis centers that can help you cope with suicidal thoughts. Include friends or loved ones who agree to be available as part of your safety plan.
- Remove potential means of killing yourself. This may include ridding your home of guns, razors or other objects you may consider using to hurt or kill yourself. If possible, give your medications to someone who can safeguard them for you and help you take them as prescribed.
- Schedule daily activities. Activities that brought you small pleasure in the past can make a difference — such as listening to music, watching a funny movie or visiting a museum. Or try something different. Because physical activity and exercise may reduce depression symptoms, consider walking, jogging, swimming, gardening or a new activity.
- Get together with others. Establish your support network by reaching out to friends, family and people who care about you and are there when you need them. Make an effort to be social, even if you don’t feel like it, to prevent isolation.
- Join a support group. Joining a support group can help you cope with suicidal thinking and recognize that there are many options in your life other than suicide.
- Avoid drug and alcohol use. Rather than numb painful feelings, alcohol and drugs can increase suicidal thoughts and the likelihood of harming yourself by making you more impulsive and more likely to act on your self-destructive feelings.
- Avoid risky websites on the Internet. Stay away from websites that may encourage suicide as a way to solve your problems.
- Write about your thoughts and feelings. Consider writing about the things in your life that you value and appreciate, no matter how small they may seem at the time.
Look beyond thoughts of suicide
The hopelessness you feel as you consider suicide may be the side effect of a difficult situation or an illness that can be treated. This emotion can be so overpowering that it clouds your judgment and leads you to believe that taking your own life is the best, or only, option.
- Recognize that these feelings are temporary and that with appropriate treatment you can learn how to help yourself feel better about life again. Asking others for support can help you see that you have other options and give you hope about the future.
- Create a list of the reasons you have to live. This list can include being alive for your pet, your children, a favorite niece, or something that you enjoy doing at work or at home. It doesn’t matter what the list includes, but finding a sense of purpose in your life can make a difference.
By getting proper treatment and using effective coping strategies, you can learn to manage or eliminate suicidal thoughts and develop a more satisfying life.
Jan. 31, 2018
What Causes Transsexualism? by Lynn Conway http://www.lynnconway.com/ Copyright @ 2000-2003, Lynn Conway. All Rights Reserved. [V-4-07-03] Many causes for transsexualism have been proposed over the years. As discussed earlier in Lynn’s TG/TS/IS information, it’s long been known from intersex data that the genes do not determine gender identity, and recent follow-ups on intersex infant surgeries show that consistency of “genitals and upbringing” does not determine gender identity. Instead, current scientific results strongly suggest neurobiological origins for transsexualism: Something appears to happen during the in-utero development of the transsexual child’s central nervous system (CNS) so that the child is left with innate, strongly perceived cross-gender body feelings and self-perceptions. We still don’t know for sure what causes this neurological development, and more research needs to be done. But the neurobiological direction for these explorations seem clear. However, even without any scientific evidence to back them up, many psychiatrists and psychologists over the past four decades have simply assumed that transsexualism is a “mental illness”. By DEFINING this socially unpopular condition to be a mental illness, these mental health professionals have shaped much of the medical establishment’s and society’s views of transsexuals as psychopathological “sexual deviants”. This page is an investigative report that describes and contrasts the older “mental illness” concept of transsexualism with more recently emerging scientific evidence of neurobiological bases for innate gender identity in humans.
| It is a capital mistake to theorize before one has data. Insensibly one begins to twist facts to suit theories, instead of theories to suit facts – – Sherlock Holmes |
[in Arthur Conan Doyle’s “A
Scandal in Bohemia” (1891)]
Traditional behaviorist psychological theories of transsexualism Behaviorist psychology was a dominent school of thought during the 1950’s-80’s, and has left a deep imprint on theories of gender and sexual behavior. Behaviorists “believe” that an infant’s mind is a blank slate upon which social factors and conditioning act to produce all aspects of personality, including gender. This belief takes the form of an axiom in their works – a basic assumption not based in evidence but upon which they derive results. Because of this belief in the infant’s “mind as a blank slate”, they have long had faith in John Money’s “genitalia and upbringing” theory of gender-identity formation. Readers should carefully study the section on Gender Basics in Lynn’s TG/TS/TS Information pages for background on John Money’s theory, and on the recent shattering of Money’s theory when it was discovered that he had fabricated many results and concealed any counterevidence. For many decades his theory was the basis for arbitrary surgical sex reassignments of intersex infants, mostly boys with tiny or missing penises who were turned into “girls”. Many of these kids reassigned as infants required later re-reassignments as boys when their innate gender identities became clear during childhood. In most cases, the boys lives were shattered by the surgeries that had been forced upon them as infants (they lost what genital tissues they had, as well as the ability to have orgasm). Money never reported any follow-ups of these infant surgeries that revealed the horrors that had been going on. As we’ll see, behaviorist theory has also had horrific impact on the lives of transsexual people, by classifying them as being “mentally ill”, instead of being open to the scientific possibility that they too have innate gender feelings. Denying the existance of any inborn gender identity, behaviorists (following Money’s ideas) see transsexualism as a failure of a person to properly socialize into their correct gender during childhood and adolescence, leading to “sexually deviant practices” in the adult which then brings on “mental illness” including the urge to “change sex”. From this viewpoint, transsexualism is viewed as psychopathological. It is even listed as a mental illness in the American Psychiatric Association’s Diagnostic and Statistical Manual of Mental Disorders, under the term “Gender Identity Disorder” (GID). This listing stigmatizes transsexualism as a mental illness, just as psychiatrists stigmatized “homosexuality” and “nymphomania” in the past (of course being gay is now seen as a natural variation in sexual-partner orientation, and being a sensual woman is now a sought-after-norm by many women). In the absence of definitive scientific explanations for transsexualism, which await a deeper understanding of developmental biology, certain dogmatic psychologists and pyschiatrists have seized the opportunity to spout and publish unscientific behaviorist “theories” without much challenge from the public, the medical establishment or the scientific establishment. They have long defended their theories in the same manner as John Money defended his: by maintaining dominant positions in their peer networks, attacking the “credentials” of any challengers, and attempting to suppress any counter-evidence put forward by others. Unfortunately, this sort of behavior can be effective in one’s advancement in niche fields such as sexology and gender studies, fields that attract few serious scientists and that are not subjected to close outside scrutiny by serious scholars. So powerful is the impact of a domineering “leader” like a John Money in a niche fields such as sexology that many wanna-be’s imitate his “dominance wins” style of behavior. When aggregated, such behaviors lead to the degeneration of such fields into non-scientific cliques of “experts” who rant about nonsense-theories not based in evidence, with each expert doing “whatever it takes” to get their pet theory accepted. Unfortunately, this “he who dominates wins” methodology is the only “scientific tradition” underlying many behaviorist psychiatrists’ theories in the realm of gender studies. Believing transsexualism to be a mental illness, behaviorist psychiatrists often try to treat transsexual people by “conditioning” and/or “aversion therapy”. Many transsexuals, especially young transsexuals taken to psychiatrists by their parents, have undergone years of costly psychiatric counseling to “cure their transsexualism”. There have no reports of permanent cures. After inevitably failing to cure a transsexual, and considering her to be “permanently mentally ill”, these psychiatrists may sometimes approve her for SRS. Of course the years of useless therapy cost thousands of dollars and waste valuable gender-corrected living-time that can never be recovered. The “two-type” behaviorist theory of transsexualism In the late 80’s, certain behaviorists proposed a very specific “two-type” theory of transsexualism that has since “caught on” in psychiatric circles as “explaining the cause of transsexual mental illness”. Two types of sexual urges were “intuited” and then described by behaviorists to explain MtF transsexualism: (i) extreme “effeminate homosexuality”, and, more recently, (ii) obsessive “autogynephilic autosexuality”. These so-called “deviant adult practices” are thought of as gradually “conditioning the transsexual” to want to “change into a woman”. The theorists proclaim that these are the only causes of transsexualism, and all MtF transsexual people are of either one type or the other. This theory was developed and elaborated BEFORE the collapse of John Money’s theory of gender was discredited, and it promotors are scrambling now to salvage it. The main promoters of this “two-type theory” are Ray Blanchard, Ph.D., a clinical sexologist at the notorious Gender Identity Clinic of Ontario’s Clarke Institute of Psychiatry who originated the idea, and his chief protege, J. Michael Bailey, Ph.D., a psychologist at Northwestern University. Only by reading Bailey in the original can you get some idea of how totally bogus and methodologically flawed this so-called “scientific work” is. For example, Bailey’s website contains a paper entitled “Women Who Were Once Boys” that simply asserts as fact, without any basis, that there are “two categories of transsexuals: homosexual and autogynephilic”, and he then uses various anecdotal evidence from “interviews” to show how TS people fit into this categorization. Bailey’s paper even goes on to include a simple twelve question “test” on how to tell the two types apart! However, it concludes with the warning: “Keep in mind that people don’t always tell the truth. This interview could be invalid if the transsexual is actually autogynephilic but is either (a) worried that you will think badly of her or deny her a sex change if you know the truth, or (b) obsessed with being a “real” woman.” Apparantly Bailey easily disregards any answers that don’t agree with his theory by simply characterizing the responder as a “lier”! For more insight into the shallow, speculative, pseudo-scientific theorizing of people like J. Michael Bailey, see the quote of Bailey attached below regarding “stereotypes of gay people that are real”. Unfortunately, the writings and lecturings of “sexologists” like Blanchard and Bailey are taken fairly seriously in psychiatric counseling circles, where few people have the courage or the wits to challenge the ideas of these aggressive theory-promoters who publish widely in obscure sexological journals. Let’s now consider each of these “two types” ideas in turn, and learn how the sexologists/psychologists/psychiatrists went wrong in their speculations. There have always been some gay males who are very effeminate. Some of these men will occasionally dress in drag. But such males do not want to become women – they love being men, and love other men – and they are simply signalling their homosexuality using methods that are traditional in the gay community. Such a gay male is never “conditioned by his sexual activity” to want to become a woman. The sexologists’ error is to not differentiate between the effeminate homosexual male and the young transsexual girl whose cross-gender feelings developed long before puberty. The sexologists thus mistakingly jump to the conclusion that effeminate homosexuality is equivalent to transsexualism, and, conversely, that addiction to “homosexual behavior” must have been what caused the transsexualism of those young TS girls who incorrectly appear to be effeminate homosexuals to the psychiatrists. In this theorizing, the sexologists and psychiatrists are victims of another of their errors, namely their notion that transsexualism is extremely rare. By assuming that transsexualism occurs in only 1:30,000 males, and then only looking for and sampling “transsexuals” in the gay male bar scene (where only a tiny fraction of TS girls hang out), they “confirm” their theory that most young TS girls come from among young “effeminate gay males” who have become addicted to receptive sex. After all, they find more than enough TS girls in that scene to cover the 1:30,000 prevalence number. What they do not perceive is that the young effeminate males and the young TS girls themselves know that they are two totally different kinds of people, even though they may hang out in some of the same bars. By overfocussing on the gay bar scene as a source for “transsexual research subjects”, the psychiatrists miss seeing the vastly larger number of TS girls who have no contact with that scene, who’ve had no “homosexual conditioning”, and who are strong counter-examples to their “theory”. By insisting on the validity of the theory that “young transsexuals cause their transsexualism by addiction to homosexual practices”, the sexologists and psychiatrists never seemed to notice the important group of “strong counter-examples” to this theory – namely that a moderate percentage (perhaps as much as 20% to 30%) of all young TS girls are actually “lesbian” in their female gendering and prefer other girls as love-partners. Worse yet, the psychiatrists years ago made the existance of these young girls “invisible” by never writing letters of support for SRS for any TS girl who was known to be “lesbian”! In other words, since these girls didn’t fit their theory of transsexualism, they were denied SRS because “they weren’t transsexual” according to the psychiatrists. As a result, even to this day, many young TS girls who are lesbian try to avoid their gender counselors about their sexual preference for girls, fearing that this preference will hurt their chances for approval for SRS. Therefore, we see that two errors in “theory”, namely (i) that transsexualism is extremely rare and (ii) that transsexualism is caused by conditioning to receptive homosexual sex, are compounded and mutually support each others’ apparant validity. This compound error is only recognized if one realizes that MtF transsexualism is about two orders of magnitude more common than previously recognized and that it mostly occurs in young boys who are not or were not immersed in the gay male bar scene. Then, in recent years, a new phenomenon has appeared that has also caught the psychiatrists’ attention: A number of intensely transvestic males have become aware, later in life, that the physical transformations made possible by transsexual medical and surgical technology might revitalize and enhance their solitary sexual pleasures. These are male-gendered persons who desire to live in, and enjoy sexually playing with themselves in, the body of a woman. These individuals may even seek SRS, even though they are male gendered and in many cases have no particular desire to socially transition. The appearance of this phenomenon is simply a byproduct of the availability of gender modification technology – an application of that technology for something different than it was originally designed for (correction of transsexualism). Such men are now called “autogynephiles”, although in public they usually call themselves “transsexuals” in order to present a more socially recognized and socially accepted explanation for their physical gender modifications. The recent tragic death of Ernest Hemingway’s son Gregory publicly revealed him to likely be an autogynephile, and revealed insights into the autogynephilic gender trajectory. Gregory had a long history of intense addiction to transvestism, and had apparently undergone SRS at sometime during his life. However, according to news reports Gregory only occasionally dressed as a woman in public, and he was referred to by the Hemingway family as Gregory (rather than Gloria or Vanessa, which were names Gregory sometimes used when dressed as a female). In such cases, the psychiatrists’ model of sexually conditioned behavior appears to offer an explanation for the behavior, because these people often self-describe their condition to counselors as being males who want to heighten their transvestic pleasures. However, such intensely transvestic autogynephilic males retain their male gender feelings even after being transformed physically into females. Therefore, they are on a completely different gender-identity trajectory from that of transsexuals. The psychiatrists’ mistake is to that they confuse autogynephilia with being equivalent to late-transitioning transsexualism. The existance of these two visible and identifiable groups of males (effeminate “homosexual” transsexuals and autogynephiles) who “appear to be transsexual”, and whose “transsexualism” appears to fit the behaviorist’s model that “sexual disorders are caused by conditioning”, has led many psychiatrists and psychologists to the generalization that ALL transsexualism is explained by just these TWO particular types of male sexual pleasure-seeking activity. Although there is no scientific basis for these behaviorist ideas, many male psychiatrists just can’t imagine anything except powerful male sexual urges gone awry that could cause an apparantly normal male to want to become a woman. Such psychiatrists thus try to stall-off transsexual surgeries as long as possible, even for decades in some cases, until it is obvious that a patient’s “homosexual urges” or “autogynephilic urges” cannot be further contained. Operating under an incorrect model of transsexualism they can do irrevocable harm by long-delaying the gender transitions of many actual transsexuals who come under their guidance. [By the way, these same male psychiatrists never question why an FtM transsexual would want to be a man, nor do they generate theories that FtM people want to be men because of “powerful female sexual urges gone awry”. To them it seems obvious that any woman might want to be a man, and thus it is only the MtF transsexual who is considered to be “mentally ill”. There is also present in their thinking a quaintly Victorian notion that only males have strong sexual drives, that only males masturbate and have orgasms, and that women are inherently passive sexually.] This situation has been worsened by additional over-promotion of the “theory of autogynephilia as the main cause of transsexualism” by an AG person who happens to run a very visible and oft-accessed TS women’s support site. This person, openly identifying as an autogynephile, projects their own experience and condition on most other transsexual women (except those who were very early transitioners and who admit having early “homosexual” activity). When doing this projection and when theorizing that most transsexual women are actually autogynephiles, this person mimics the well-known macho-dominant style of John Money – doing anything possible to promote their “theory” and to defame as “liers” those who “deny being autogynephiles”. Amazingly, the promoters of the autogynephilia theory of late-transitioners don’t seem to notice that many late transitioners do not just spend their lives alone engaging in solo-sex after transition as their theory would suggest. Instead, many late transitioners go on to form wonderful loving relationships – some with women and some with men – relationships in which they are fully sexual love-partners. Sadly, the widespread promotion of the non-scientific “autogynephilia theory” has caused a lot of angst among transsexual women who correctly perceive this as yet another trigger for public stigmatization and humiliation. Unfortunately, many decades of such speculative, non-evidence-based theorizing about the causes of transsexualism have greatly muddied the waters of thinking about this condition. To this day, the mental-illness model of the condition permeates the general medical profession and negatively impacts public stereotypes of transsexual people. All of this “theorizing” is without any scientific foundation whatsoever, being little more than the “intuitions” of the most dominant thought leaders among sexologists, starting with John Money. Maybe we should raise the question “what causes people to become sexologists”, apply the same “intuitive” methods to answer that question, and then see how sexologists react to our resulting theories! Applying some common sense to question these behaviorist “theories” Now let’s apply some common sense here. The deep sense of being incorrectly gendered begins in childhood for intense transsexuals, long before sexual feelings develop. After puberty, many young pre-op TS girls are attracted to boys just like any other girl would be. TS girls who are feminine and attractive may find boyfriends and make love with them while pre-op, just as any other girl would do. But these are not boy-to-boy homosexual relationships. These young transsexuals are thought of as girls by their boyfriends (just as Lynn was at ages 19-22), and their boyfriends are heterosexual, not homosexual. For psychiatrists to say that the “homosexual” sexual experiences of pre-op TS girls’ CAUSES their transsexualism is an incredible reversal of cause and effect. Instead it is their innate feelings of being female that cause them to seek the love of boys, and then in some cases to have sex with boys (always as “the girl”) in order to find affirmation of their femaleness. Also, many older MtF transsexuals if long untreated become obsessed with the idea of becoming women. Is that so surprising? Older pre-op transsexuals without partners may also be autosexual. But aren’t most humans without partners autosexual? Masturbation itself is not a solely a “male” activity nor is it a sign of “autogynephilia”, as these psychiatrists seem to suggest. Many women enjoy their bodies very much, and many women masturbate for sexual pleasure and orgasmic release. Autosexuality on the part of pre-op (and postop) transsexuals of any age is just a natural part of their human nature, whether male or female, instead of being a “male sexual fetish”. (It seems likely now that the old time male behaviorist psychologists didn’t even know that many women masturbate and can have orgasms!). To say that “thinking about being a woman while engaging in autosexual activity” CAUSES transsexualism is clearly another reversal of cause and effect. My goodness, do you think that a preop MtF transsexual would have masturbation fantasies in which she is a man? Common sense says she will have sexual fantasies in which she is a woman, because that is her inner identity. Therefore, to say that ALL late-transitioning transsexuals are autogynephilic is similarly a reversal of cause and effect. Unfortunately, most male psychiatrists and psychologists, never themselves having experienced the intense gender-identity-alienation, cannot get the idea out of their heads that “sexual urges must be the cause” (their own male sexual urges being the strongest urges they themselves have ever felt). In summary: Common sense tells us that the sexual practices of pre-op transsexuals, as they struggle during their difficult life trajectories to cope with bodies that are mis-gendered, can be far more easily explained and understood as being a natural BYPRODUCT of, rather than the CAUSE of, their transsexualism. Thus the old “mental illness” theories of transsexualism are based on a classic error in science: They have confused, reversed and conflated CAUSE and EFFECT. A lot of damage is done by the old mental illness theories. When psychiatric authority figures subtly brainwash a transsexual patient into believing that she is causing her own transsexualism by engaging in “homosexuality” or “autogynephilic masturbation”, and then attempt to delay her transition for years or decades, she can lose all chances of ever later assimilating into society as a woman. Even if she transitions, she may actually think of herself as a deviant male rather than as a woman, and may be stuck with that self-image forever. This is especially true in cases where her psychiatrists insist that she buy into and parrot their theories, forcing her to admit that she is a “mentally-ill man” as a condition for signing letters of consent for her SRS. When a counselor uses the terms homosexual transsexual and autogynephilic transsexual to classify their clients, it’s a sure tip-off they believe that ALL transsexuals are mentally ill sexual deviants who have caused their own transsexualism. Lynn advises transsexuals to avoid counselors who label transsexuals in these judgmental behaviorist categories. Transsexuals are also advised to avoid TG/TS support groups whose members identify primarily as autogynephilic, because they will not fit-in well and will not learn useful skills for assimilation as women in such groups. [On the other hand, older highly transvestic males who desire transsexual physical modifications should seek out such support groups; they should also seek counselors whose practice primarily involves autogynephiles, and who will refer such males for transsexual surgery, including SRS.] For further discussion regarding the psychological and psychiatric profession’s unscientific conception of transsexualism as a mental illness, see Gender as Illness: Issues of Psychiatric Classification by Katherine K. Wilson of the Gender Identity Clinic of Colorado (GIC). GIC has also developed a new webpage resource for the Reform of Gender Disorders in the DSM-IV-TR, located at http://gidreform.org/. Also consider recent research by psychiatrists in Norway that has found that TS patients selected for sex reassignment showed a relatively low level of psychopathology both before and after treatment. This new research also casts doubt on the old view that transsexualism is a “severe mental disorder”. For a further indictment of the professionalism, scientific credibility, factual accuracy and veracity of the APA and the DSM-IV regarding transsexualism, see Lynn’s discussion of the question “How frequently does transsexualism occur?“.
Recent neurological theories of transsexualism Except for the behaviorists (who unfortunately are still dominant among “sexologists” and “gender theorists”), most schools of psychological thought have ruled out causes related to upbringing, social interactions and sexual practices as leading to transsexualism. As in other fundamental areas of personality, most scientific researchers now believe that the formation of gender identity most likely occurs at an innate neurobiological level. Serious scientific research on the formation of gender identity is now focused on understanding the processes of CNS neurological integration of the fetus during pregnancy. Recent research indicates that MtF transsexualism may result from a female differentiation in a genetic male of the BSTc portion of the hypothalamus, during interactions between the developing brain and fetal sex hormones; this brain region is essential to sexual feelings and behavior. The first such research was reported in 1995: See NATURE, 378: 60-70, 1995 (this paper is also web accessible at http://www.symposion.com/ijt/ijtc0106.htm ). Significant extensions of this earlier work have just been reported, in May 2000 (see following abstract and link to the full paper) :
| The Journal of Clinical Endocrinology & Metabolism, May 2000, p. 2034-2041 Copyright 2000, The Endocrine Society Vol. 85, No. 5 Male-to-Female Transsexuals Have Female Neuron Numbers in a Limbic Nucleus Frank P. M. Kruijver, Jiang-Ning Zhou, Chris W. Pool, Michel A. Hofman, Louis J. G. Gooren, and Dick F. Swaab Graduate School Neurosciences Amsterdam (F.P.M.K., J.-N.Z., C.W.P., M.A.H., D.F.S.), Netherlands Institute for Brain Research, 1105 AZ Amsterdam ZO, The Netherlands; Department of Endocrinology (L.J.G.G.), Free University Hospital, 1007 MB Amsterdam, The Netherlands; and Anhui Geriatric Institute (J.-N.Z.), The First Affiliated Hospital of Anhui Medical University, Hefei, Anhui, 230032 China Address all correspondence and requests for reprints to: Frank P. M. Kruijver, M.D., or Prof. Dick F. Swaab, M.D., Ph.D., Graduate School Neurosciences Amsterdam, Netherlands Institute for Brain Research, Meibergdreef 33, 1105 AZ Amsterdam ZO, The Netherlands. E-mail: F.Kruijver@nih.knaw.nl. Abstract Transsexuals experience themselves as being of the opposite sex, despite having the biological characteristics of one sex. A crucial question resulting from a previous brain study in male-to-female transsexuals was whether the reported difference according to gender identity in the central part of the bed nucleus of the stria terminalis (BSTc) was based on a neuronal difference in the BSTc itself or just a reflection of a difference in vasoactive intestinal polypeptide innervation from the amygdala, which was used as a marker. Therefore, we determined in 42 subjects the number of somatostatin-expressing neurons in the BSTc in relation to sex, sexual orientation, gender identity, and past or present hormonal status. Regardless of sexual orientation, men had almost twice as many somatostatin neurons as women (P < 0.006). The number of neurons in the BSTc of male-to-female transsexuals was similar to that of the females (P =3D 0.83). In contrast, the neuron number of a female-to-male transsexual was found to be in the male range. Hormone treatment or sex hormone level variations in adulthood did not seem to have influenced BSTc neuron numbers. The present findings of somatostatin neuronal sex differences in the BSTc and its sex reversal in the transsexual brain clearly support the paradigm that in transsexuals sexual differentiation of the brain and genitals may go into opposite directions and point to a neurobiological basis of gender identity disorder. |
Support for this brain-differentiation and CNS imprinting theory of gender identity also comes from the recently reported research studies on intersex boys who had been surgically changed into girls and raised as girls, yet who grew up insisting on being boys (see the important earlier section on the intersexed). These follow-up studies demonstrate that having female genitals and being raised as girls did not make these brain-sexed boys into girls. They somehow deeply knew that they were boys, in spite of all the external evidence that they were girls – in other words, they presented just as if they were FtM transsexual boys. The we an see how the old behaviorist “genitals plus upbringing” psychological theory has caused tremendous pain and suffering, especially amongst (i) intersexed children who’ve undergone unwanted genital surgery and incorrect gender reassignment during their upbringing, and (ii) transsexual children who’ve undergone extended psychiatric “treatment” such as shock therapy, aversion therapy and behaviorist conditioning therapy in futile efforts to “reverse” their transsexualism, and who’ve been forced to grow up in the wrong gender in spite of their pleas and suffering. In the case of transsexual children there is also the added social stigmatization of being declared “mentally ill” by the psychiatric profession. Emerging scientific understanding of gender identity and the accumulating empirical evidence of successful gender transitions can help society and the medical community avoid such terrible treatments and misclassifications in the future, and better help these innocent children to find their best paths in life in each individual case. If anyone doubts that those who undergo gender transition can go on to lead full and happy lives, all they need do is study the empirical evidence at Lynn’s “TS Women’s Successes” and “Successful TransMen” pages. What if there is no cause? Could gender transition just be a “lifestyle choice”? Is gender transition a “choice” or “fate”? This question very often arises in conversations about transsexualism. The notion that transition is a lifestyle “choice” is rather prevalent in our society, and can be just as stigmatizing as the idea that it is due to a mental illness. But why do people jump to the conclusion that it is a choice? Perhaps it is because of the apparent suddenness of the onset of many transsexual transitions. Transsexual women often appear to be completely normal males before announcing they are going to “change sex”. The apparent suddenness of these transitions, and the rapid and dramatic physical changes that follow, fuels speculation among family, friends and co-workers that these “decisions” are very irrational ones. People often interpret unexpected transitions as “mental breakdowns”, or as sudden “choices” to do something totally weird and prurient and probably for “sexual reasons”. (These interpretations are furthered by the occasional cases of autogynephilic males who go through hormone therapy and SRS specifically for sexual reasons, and who remain rather visibly transgendered and do not “vibe” as women afterwards). What most people cannot comprehend is the extreme gender distress these transsexuals have endured during their entire lives. Forced by extreme family and societal pressures to keep their distress a secret from everyone else and never show any signs of cross-gender feelings, they simply suffer horrifically in silence, never revealing what is wrong inside. When the gender angst becomes totally overwhelming, and transsexual people seek counseling and discover options for gender-transition, the floodgates open in their minds: Transition then becomes an intensely sought-after goal, and to others may appear to have arisen out of the blue, as if it were a sudden “choice”. However, gender transition is NOT a choice. Instead it is destiny for those who are intensely transsexual. Why is there so much fixation on “causes” anyway?Do we really need to know the cause in order to treat the condition? Why is there so much fixation on “causes” anyway? The answer is simple: Transsexualism has been such a socially unpopular condition in the past that the issue of “what causes it” has always raised in discussions about what to do about it. In the past many behaviorist psychologists and psychiatrists have inherently blamed transsexuals for causing their own “sexually deviant mental illness”, giving those psychiatrists a claim to responsibility for “treatment and cure of transsexual people” and giving society a rationale for discrimination, marginalization and ghettoization of transsexual people. However, as we’ve seen, transsexualism is most likely a neurological condition of as yet unknown origin and not a “mental illness”. There are many other intense neurological conditions such a pain, depression and bipolar disorders for which we do not know the underlying causes but suspect biological causes. We know that these other conditions are real because we see people in distress, and we treat those people medically and with compassion to relieve their suffering. Why should it be any different with transsexualism? We now know how to relieve the suffering of transsexual people, having many options for practical counseling, social transition and hormonal/surgical gender reassignment. Why not accept those treatments as valid, since they truly relieve suffering and enhance the quality of life, even if we aren’t sure what causes the underlying condition. And why stigmatize people just because they have sought medical treatment for this condition. Fortunately there are a rapidly growing number of compassionate non-behaviorist gender counselors who provide practical help for transitioning transsexual people. These counselors follow a model of “informed consent” for their clients, presenting options for treatments and counseling clients on pragmatic, effective ways of resolving their gender issues. Most present-day, self-reliant transsexual people who are planning and managing their own transitions seek the advice and counsel of the modern-day pragmatic gender-counselors, and they avoid traditional psychiatrists like the plague. Modern medical treatments can resolve the transsexual condition, even in the absence of scientific understanding of the detailed biological mechanisms that determine one’s innate gender identity. Return to Lynn’s TG/TS/IS information page
Appendix: The following quote of J. Michael Bailey will help readers calibrate the incredibly naive and non-scientific level of thinking common among so-called “sexological researchers” when they speculate about and characterize their “research subjects”. Any intelligent reader will sense the arrogance, shallowness and lack of perceptiveness in Bailey’s thinking, his lack of sound evidence upon which to base conclusions, and his total conflation of causes and effects. Ask yourself if YOU’D like to be on the receiving end of “scientific thinking” like this? Need I say more?
| Source: http://after-words.org/grim/mtarchives/2002/08/index.shtml From an Interview on Stereotypes of Homosexuals. With J. Michael Bailey, Department of Psychology, Northwestern University Q: What stereotypes have turned out to have some truth to them? A: One big thing is occupational and recreational interests. In fact, hairdressers, professional dancers, actors and designers tend to be gay men, at least at much higher rates than their population rate, which is somewhere between 1 and 4 percent. And women who are in the armed services, or professional athletes (two of the three best all-time women’s tennis players are lesbian), are disproportionately lesbian. Children who are sex-atypical do tend to become homosexual. Especially males. Boys who want to be girls become men who want men. Most very masculine girls probably become heterosexual women, but their rate of homosexuality is probably still higher than would be expected given the population rate of female homosexuality, which is probably less than 1 percent. Recently, we have shown that on average, gay men and lesbians are very different on average from straight people in the way they walk and speak. There is such a thing, evidently, as a gay voice. And lesbians tend to look different than straight women — in particular, they have shorter hairstyles. On the other hand, some stereotypes about homosexual people are due to the fact that they are in certain other ways psychologically like straight people of their own sex. For example, gay men have lots of sex partners compared with straight men. This is because they have a male-typical level of interest in casual sex, but because they are seeking other men with the same interest, they can have as many partners as they want. Straight men are constrained by the desires of women. I think that there is nothing intrinsically “gay” about having hundreds of sex partners. Lots of straight guys would if they could. But they can’t, because they can’t find female partners who’ll have anonymous sex with them. |
Women have an at least equal propensity for evil and violence, they are also more vulnerable to mental illness. What they may lack in physical strength, they make up with weapons, deviousness and lies. May 22nd 2020




For Mental Health Awareness Week 2020, Stylist looks back on some of our most powerful essays on mental health, to offer support and solidarity during this week and beyond.
During the coronavirus pandemic, we’re talking about our mental health more and more.
Mental health charities have warned that anxiety and stress are on the rise in the UK, while psychiatrists have suggested there could be a “tsunami” of mental illness following lockdown.
And here’s a sobering statistic to consider: even before the coronavirus crisis, more than half (51%) of young women aged 18-30 in the UK said they were currently worried about their mental health. This figure was a sharp rise from 2016, when 38% of young women said they were worried about their mental health. The data, compiled by the Young Women’s Trust last year, shows a concerning trend for fears around issues such as anxiety, depression and OCD.

Stylist is proud to publish the following beautiful and moving essays from women detailing how they manage their mental health. While mental health is a big issue, estimated to affect one in four people in the UK every year, each person will have a unique experience with it – as these women’s words so eloquently prove.
Read on to find out how some of our most powerful writers faced challenges from dealing with anxiety and depression to battling insomnia and even their own genetics.
You may also like
Mental health diary: the life of a supermarket worker during the pandemic
“I’ve been having therapy over Zoom for a month and it’s completely changed my perspective”

Due to the UK lockdown, therapy sessions are now taking place across online platforms such as Zoom. Here, one writer describes what it’s like to tell a screen about her most intimate feelings.
“How running every day has made me happier – and why it can for you, too”

Following the breakdown of her marriage and a mental health crisis, Jog On author Bella Mackie turned to running – and she hasn’t looked back since. Here, Bella talks about the brilliant power of exercise for boosting our mental health, and shares her advice on getting started with your own running regime.
“My postpartum psychosis made me believe I was Cameron Diaz”

Postpartum psychosis is a rare mental health condition that can affect new mums. Here, one writer shares her own experiences of postpartum psychosis and postnatal depression following the birth of her son.
“How therapy helped me through my mum’s suicide”

Mary-Jane Wiltsher was 16 when her mum took her own life. After burying her grief throughout her twenties, she reconnected with her school therapist – a decision that changed her life.
The reality of body dysmorphia: “I don’t see myself the way others do”

Freelance journalist Millie Milliken talks about her experience with Body Dysmorphic Disorder for the first time, and offers an insight into life with the condition.
What it’s really like living with OCD: “I’m obsessed with the harm I could cause”

“The intrusive thoughts in my head range from starting fires, to causing car accidents, murder and other possibilities I find hard to write, even now,” says freelance journalist, Lucy Donoughue.
“The surprisingly simple way I learned to live with my anxiety”

“I can’t banish my anxiety, but I can control it. I can tame it,” writes journalist Kate Townshend.
“How it feels to inherit a mental illness”

From a young age, author Amy Molloy knew mental illness was rife in her family – especially among the women. Yet, by spending her life studying optimistic coping mechanisms, she believes she has finally broken the cycle. Here, she shares what she has learnt on her journey to happiness.
“How I use video games to curb my anxiety”

Videogames get a bad rap in the media, but countless studies have shown they’re actually really good for our mental health. Here, Stylist’s digital editor-at-large Kayleigh Dray explains how she uses videogames to regain a sense of control whenever she finds herself crippled by anxiety.
If you, or someone you know, is struggling with mental health issues, you can find support and resources on mental health charity Mind’s website or see the NHS’ list of mental health helplines here
This article was originally published in 18 May 2018 but has been updated throughout
Images: Getty, Maaike Nienhuis Jose Fontano, Min An, Holly Mandarich, Joshua Rawson Harris, Ev, MMPR, Pawel Kadysz
Topics
- Commissions
- Features
- Mental Health
- Mental Health Awareness Week
- Depression
- Anxiety
- Sleep
- Advice
- On Instagram
Share this article
Author

Sarah Biddlecombe
Sarah Biddlecombe is an award-winning journalist and Digital Commissioning Editor at Stylist. Follow her on Twitter
Recommended by Sarah Biddlecombe
How to deal with night-time stress and anxiety, according to a longtime sufferer
A new survey has revealed stress remains the number one barrier to a good night’s sleep around the world.Posted byKate Faithfull-WilliamsPublished2 months agoLong Reads
The Maytree: “What happened when I checked myself into the UK’s only suicide sanctuary”
The Maytree is a respite centre that offers help and support for those in suicidal crisis. One woman checks in for five days.Posted byRachel BarberPublished8 months agoLong Reads
“How running every day has made me happier – and why it can for you, too”
Bella Mackie turned to running after a marriage breakdown and a mental health crisis. She hasn’t looked back since.Posted byBella MackiePublished29 days ago
More about Commissions
A day in the life: a Marie Stopes nurse working through the pandemic
This Mental Health Awareness Week, Stylist is sharing mental health diaries from key workers.Posted byStylist TeamPublished6 hours agoLong Reads
Catching feelings? Here’s how to protect yourself from others’ negative emotions
You have every right to look after yourself during this worrying time.Posted byRuby DeevoyPublished20 hours agoLife
6 of the best eco-friendly sanitary brands you need to know about
27,938 used tampons and applicators were found on the world’s beaches in a single day. Let’s change that.Posted bySarah BiddlecombePublished21 hours agoLong Reads
7 easy ways to be a kinder person during lockdown
Now more than ever, we need kindness in the world.Posted bySusan DevaneyPublished1 day agoLife
“Why I tell my friends I’m taking antidepressants”
As new figures reveal that antidepressant usage has surged since lockdown, Stylist’s Lauren Geall explores why talking about medication is so important.Posted byLauren GeallPublished1 day agoLong Reads
A day in the life: a school teacher working from home during coronavirus
This Mental Health Awareness Week, Stylist is sharing mental health diaries from key workers on the frontline of the fight against coronavirus. Posted byStylist TeamPublished1 day agoLong Reads
Are you taking on too much emotional labour at work?
“Go easy on yourself and remember that this is a challenging situation.”Posted bySarah BiddlecombePublished1 day agoLong Reads
A day in the life: a therapist working through the pandemic
This Mental Health Awareness Week, Stylist is sharing mental health diaries from key workers on the frontline of the fight against coronavirus. Posted byStylist TeamPublished2 days ago
More from Sarah Biddlecombe
6 of the best eco-friendly sanitary brands you need to know about
27,938 used tampons and applicators were found on the world’s beaches in a single day. Let’s change that.Posted bySarah BiddlecombePublished21 hours agoLong Reads
Are you taking on too much emotional labour at work?
“Go easy on yourself and remember that this is a challenging situation.”Posted bySarah BiddlecombePublished1 day agoFood
How to bake the ultimate sourdough starter and loaf
Everything you need to know about baking your own sourdough.Posted bySarah BiddlecombePublished5 days agoLong Reads
“My housemate isn’t social distancing properly. How do I talk to them about it?”
What’s the best way to handle tension when you and housemates disagree on the social distancing rules?Posted bySarah BiddlecombePublished5 days agoLong Reads
All your post-lockdown rent and mortgage questions, answered
England’s housing market has reopened, but if you’re struggling to pay your rent or mortgage, there is help available.Posted bySarah BiddlecombePublished7 days agoLong Reads
What it’s really like to be an NHS nurse right now
“We’re almost risking our own lives to help other people.”Posted bySarah BiddlecombePublished9 days agoOpinion
Sex Change Hormonal Treatments Alter Brain Chemistry Posted March 6th 2020

Polly Sexual’s Image by Appledene Photographics.
Reports new study in Biological Psychiatry Share this:
Philadelphia, PA, October 8, 2015
Hormonal treatments administered as part of the procedures for sex reassignment have well-known and well-documented effects on the secondary sexual characteristics of the adult body, shifting a recipient’s physical appearance to that of the opposite sex.
New research published in the current issue of Biological Psychiatry indicates that these hormonal treatments also alter brain chemistry.
Researchers at the Medical University of Vienna, led by senior authors Dr. Siegfried Kasper and Dr. Rupert Lanzenberger, show that administration of the male hormone testosterone in female-to-male transsexuals raises brain levels of SERT, the protein that transports the chemical messenger serotonin into nerve cells.
In contrast, male-to-female transsexuals who received a testosterone blocker and the female hormone estrogen showed decreased levels of this protein in the brain.
SERT plays an important role in the treatment of mood and anxiety disorders, as many common antidepressants, such as Prozac, block its activity by inhibiting serotonin reuptake. In addition, some genetics studies have suggested that higher levels of serotonin transporter may increase resilience to stress and reduce risk for stress and mood disorders.
Because women are twice as likely to be diagnosed with depression as men, these changes in the levels of SERT are consistent with the increased risk for mood and anxiety disorders in females relative to males.
Lanzenberger added, “These results may explain why testosterone improves symptoms in some forms of depression. Our study also increases our knowledge on the role of sex hormones in sex differences of mood disorders.”
Overall, these findings suggest that when people switch from female to male, their biology changes in a way that is consistent with a reduced risk for mood and anxiety disorders, whereas the reverse happens when males switch to females.
“This study is the first to show changes in brain chemistry associated with the hormonal treatments administered in the sex change process,” said Dr. John Krystal, Editor of Biological Psychiatry. “It provides new insight into the ways that the hormonal differences between men and women influence mood and the risk for mood disorders.”
The article is “High-Dose Testosterone Treatment Increases Serotonin Transporter Binding in Transgender People” by Georg S. Kranz, Wolfgang Wadsak, Ulrike Kaufmann, Markus Savli, Pia Baldinger, Gregor Gryglewski, Daniela Haeusler, Marie Spies, Markus Mitterhauser, Siegfried Kasper, and Rupert Lanzenberger (doi: 10.1016/j.biopsych.2014.09.010). The article appears in Biological Psychiatry, Volume 78, Issue 8 (October 15, 2015), published by Elsevier.
—
Notes for editors
Full text of the article is available to credentialed journalists upon request; contact Rhiannon Bugno at +1 214 648 0880 or Biol.Psych@utsouthwestern.edu. Journalists wishing to interview the authors may contact Dr. Rupert Lanzenberger at +43 (1) 40400 35760 or rupert.lanzenberger@meduniwien.ac.at.
The authors’ affiliations, and disclosures of financial and conflicts of interests are available in the article.
John H. Krystal, M.D., is Chairman of the Department of Psychiatry at the Yale University School of Medicine, Chief of Psychiatry at Yale-New Haven Hospital, and a research psychiatrist at the VA Connecticut Healthcare System. His disclosures of financial and conflicts of interests are available here.
About Biological Psychiatry
Biological Psychiatry is the official journal of the Society of Biological Psychiatry, whose purpose is to promote excellence in scientific research and education in fields that investigate the nature, causes, mechanisms and treatments of disorders of thought, emotion, or behavior. In accord with this mission, this peer-reviewed, rapid-publication, international journal publishes both basic and clinical contributions from all disciplines and research areas relevant to the pathophysiology and treatment of major psychiatric disorders.
The journal publishes novel results of original research which represent an important new lead or significant impact on the field, particularly those addressing genetic and environmental risk factors, neural circuitry and neurochemistry, and important new therapeutic approaches. Reviews and commentaries that focus on topics of current research and interest are also encouraged.
Biological Psychiatry is one of the most selective and highly cited journals in the field of psychiatric neuroscience. It is ranked 6th out of 140 Psychiatry titles and 10th out of 252 Neurosciences titles in the Journal Citations Reports® published by Thomson Reuters. The 2014 Impact Factor score for Biological Psychiatry is 10.255.
About Elsevier
Elsevier is a global information analytics business that helps scientists and clinicians to find new answers, reshape human knowledge, and tackle the most urgent human crises. For 140 years, we have partnered with the research world to curate and verify scientific knowledge. Today, we’re committed to bringing that rigor to a new generation of platforms. Elsevier provides digital solutions and tools in the areas of strategic research management, R&D performance, clinical decision support, and professional education; including ScienceDirect, Scopus, SciVal, ClinicalKey and Sherpath. Elsevier publishes over 2,500 digitized journals, including The Lancet and Cell, 39,000 e-book titles and many iconic reference works, including Gray’s Anatomy. Elsevier is part of RELX, a global provider of information-based analytics and decision tools for professional and business customers. www.elsevier.com
Media Contact
Rhiannon Bugno, Editorial Office
+1 214 648 0880
Biol.Psych@utsouthwestern.edu
Can Women be as Violent as Men? Posted February 20th 2020
As a rule of thumb, men are responsible for over 90 percent of serious violent crimes, such as assaults, homicides, and violent robberies. Why is there such a large gender gap and is it likely to persist?
One might imagine that lower violent crime rates for women reflects a generally lower level of aggression. Yet, marriage researchers observe the opposite pattern. Women are more likely to pick fights with their husbands, they are quicker to escalate verbal aggression, and are as likely to use physical aggression as men (1).
Despite these counter-intuitive findings, men are much more likely to be convicted of domestic-violence-related charges. One obvious reason for this is that men are generally larger and stronger, and may have more experience with physical aggression, such as that commonly associated with contact sports.
Despite these counter-intuitive findings, men are much more likely to be convicted of domestic-violence-related charges. One obvious reason for this is that men are generally larger and stronger, and may have more experience with physical aggression, such as that commonly associated with contact sports.
Another intriguing difference between men and women in the context of domestic disputes is that men generally become more physiologically aroused in terms of increased blood pressure (2).
If the body is revved up for action, damaging aggression is more likely. Moreover, when it occurs, the aggression is more likely to be extreme, uncontrolled, or “disinhibited,” words that are sometimes used to describe the orgy of violence in unusually grisly crimes of violence.
In the vast majority of such crimes, the perpetrators are men.
Modern women are behaving much more like men when it comes to risk-taking and aggression. One sign of this phenomenon is greater participation in contact sports and dangerous competitions such as horse racing or car racing. According to Anthropologist Elizabeth Cashdan (5), in societies where women compete more amongst each other whether in occupations, or over spouses, their levels of stress hormones and testosterone increase.
In the modern world, there are far more women driving on the roads and they drive more aggressively and dangerously than ever before. As a result, their accident rates have risen from very low levels and young women are almost as dangerous on the roads as young men whose aggression and recklessness make driving much more dangerous for everyone else. Small wonder then that women are showing up in previously all-male crimes such as violent bank robbery.
As women have begun to take leadership positions in large corporations, they have also acted as leaders in criminal enterprises. One of the most successful Latin American drug kingpins was a Colombian woman, Griselda Bianco, known as La Madrina, who ran an extensive U.S. operation from Miami. She is not the only woman to rise to the top in organized crime.
That there are female equivalents of Pablo Escobar is intriguing from the perspective of gender differences in violence. Yet, there have always been female sociopaths, just fewer of them than males. Such figures certainly challenge gender stereotypes.
Yet, most evolutionary psychologists would predict that even amongst the restricted population of violent criminals, females will continue to be less extremely violent. The reason is that women remain generally less violent and more risk-averse than men. This risk aversion is tied to an evolutionary past in which women did most of the childcare and avoided violence as a way of staying alive to protect their children.
That theory has already failed in respect to vanishing gender differences in traffic accidents. We should not be too shocked if more women also take up bank robbery, and other violent crimes, as their “job.”
Notes
1. Arriaga, X. B., and Oskamp, S., Eds. (1999). Violence in intimate relationships. London: Sage.
2. Gottman, J. M., and Levenson, R. W. (1988). The social psychophysiology of marriage. In P. Moller and M. A. Fitzpatrick, Eds., Perspectives on marital interaction. Clevedon, England: Multilingual Matters.
3. Barber, N. (2002). The science of romance. Buffalo, NY: Prometheus.
4. Barber, N. (2009). Countries with fewer males have more violent crime: Marriage markets and mating aggression. Aggressive Behavior, 35, 49-56.
5. Cashdan, E. (2008). Waist-to-hip ratios across cultures: Trade-offs between androgen- and estrogen-dependent traits. Current Anthropology, 49, 1099-1107.
About the Author
Nigel Barber, Ph.D., is an evolutionary psychologist as well as the author of Why Parents Matter and The Science of Romance, among other books. In Print:The Myth of Culture: Why We Need a Genuine Natural Science of Societies
Can Two People Have the Same Dream?
If two people can share the same dream, then dreams transcend individual minds.
Posted Jun 19, 2016
Can two or more people share the same dream? As far as I know, there have been no scientific investigations of this question. But there are literally thousands of well-documented accounts.
The best-documented cases involve therapist-client shared dreams. In these, there is a professionally trained therapist who verifies the claim that the dream happened to both the therapist and the client around the same time. The next-best documented cases involve people in close relationships like parent/children, spouses, or lovers. Consistent with the effect of emotional closeness on shared dreams, we also have plenty of well-documented cases of twins sharing the same dream. The least well-documented cases involve complete strangers sharing the same dream. (We only have anecdotal reports of strangers experiencing the same dream because the strangers happened to run into one another and recognize each another from the dream!)
I have written about the shared dreams of twins in this blog and cited sources on twins in that post. For sources on shared dreams between therapists and clients, see Anthony Shafton’s 1995 book Dream Reader. For sources on complete strangers sharing dreams, see Frank Seafield’s Dream Curiosities. You can also find forums on shared dreams all over the web. We have to conclude that people everywhere do occasionally experience the same dream as another individual.
What are we to make of this fact? First, all we have are anecdotal reports. People believe they experienced the same dream, but we have to remain skeptical until controlled scientific investigations are conducted. In addition, the two people involved never agree about every detail about the shared dream. Nevertheless, I have learned to respect anecdotal reports in the world of dream research because these reports are usually reliable. There is no incentive for people to lie about the experience.
There are some commonalities among the reports that increase confidence in their reliability. For example, most often the two people involved know each other and are emotionally close. Obviously, you are more likely to hear about unusual experiences involving two people if they see each other on a regular basis. In addition, the way in which the two people typically discover that they shared a dream is that one person begins sharing the dream without knowing that the other person had the same one until the other person jumps in and finishes it.
People often report that nothing unusual happened before the shared dream. They report that they did not talk about dreams with the other person before the event, so there is no indication of biasing or priming effects. The fact that the two people involved often do not agree about every detail in the dream actually increases my confidence that the reports are honest accounts. It seems inevitable that individual differences, ranging from mood to IQ to memory differences, prevent people from recalling every detail of a dream—so reports of a shared dream should vary accordingly. The small amount of variance concerning details in reports of shared dreams therefore makes sense. Interestingly, the timing of the event can vary as well. Sometimes the shared dream occurs at the same time for both people. In other cases, it does not. What is remarkable is that so much of the shared dream, sometimes including small details, are recalled as strikingly similar or even identical by the two people involved, regardless of the timing of their experiences. article continues after advertisement
So let us provisionally accept the fact of shared dreams: Two persons can have the same dream. What does this imply for the science of dreams? If we assume that brains produce dreams, we have to assume that the two brains involved were in the appropriate brain states to produce identical content in two people. This may mean that the two people must have been in identical brain states, and that these identical states produced the same cognitive content.
Yet this option seems almost impossible to me given the huge plasticity and variability in brain physiologies across individuals. Even the brains of twins are vastly dissimilar. So attributing shared dreams to coincidentally identical brain states seems a stretch. But other alternative explanations are equally unappealing: For example, two people having the same dream seems to suggest that dreams are not mere products of the sleeping brain. Instead, they arise outside of us and then “happen” to us. They are in some sense independent of the minds that record and express them. Dreams are perhaps products of the interpersonal cultural world and float in the cultural morphospace waiting to alight on an individual consciousness.
But if that were the case, why is it that the cultural memes manifest as shared dreams and not some identical cognitive content in waking life? Perhaps shared dreams are like abstract Platonic forms that are bigger than individual brains, so they are able manifest in several brains attuned to the form.
None of these possibilities seem appealing or plausible to me.
In short, we have no good explanations for shared dreams. Perhaps that is why science has not yet investigated these events. Science has no place to put them within its current worldview—but this is all the more reason to investigate them. Paradigm-challenging phenomena are the most important data for science because they force revolutionary changes.
How Psychology Deals With The Concept Of “Toxic Masculinity” Posted January 15th 2020
There’s been a lot of discussion in the media over the last couple years about the topic of “toxic masculinity.” Some commentators seem to blame it for all the world’s problems, while others feel the term itself is an attack on all men, no matter what their backgrounds. It is difficult to find a measured view of what toxic masculinity is, detached from personal opinions and judgments. If you look at Twitter conversations on the subject, you will find anger and rhetoric, often along political lines.
But toxic masculinity is an important concept in the field of psychology. Understanding it in such a way that it is helpful rather than harmful, is necessary in order to address the actual problems.
What is “Toxic Masculinity”?
As soon as we use the term “toxic masculinity,” we hit a point of contention. Are we saying that masculinity is toxic, or are we saying that there is a kind of masculinity that is toxic? For the purposes of healing, it is crucial that we maintain the latter approach. In a psychological sense, a person or group of people are never the problem. Rather, it is a behavior or set of behaviors that is problematic.
Masculinity Definition
Masculinity itself is not easily defined. When we get down to the biological basics, men and women are not all that different. Aside from the obvious physical differences, our brains are almost exactly the same. Most of the differences we perceive between the genders stem from social and cultural constructs of how we expect men and women to behave.
So masculinity can be defined as a set of traits or even a culture we consider masculine. There is, of course, nothing wrong with being a man or associating with masculine traits, which is why it is so important to separate masculinity itself from the concept of toxicity.
Toxicity Definition
In the context of toxic masculinity, toxicity refers to behaviors, feelings, and thoughts which have a negative impact on the individual and those around them. Toxicity therefore refers to when traits considered masculine are exaggerated to a point at which they become harmful, as well as traits which if expressed at all will harm others.
For example, a man can be proud of his physical strength and even consider it an aspect of his masculinity. However, if he uses it to abuse, exert control over or denigrate others, it has become toxic. At their worst, toxic traits can lead to rape, murder, and other forms of violence. Similarly, if his self-worth is bound up in how physically strong he is, it has become toxic to himself.
When considering toxic masculinity, psychologists are therefore concerned about two separate but related themes: the harm it causes to woman and the harm it causes to men.
Many women speak to their therapists about the effect of toxic masculinity on their own lives. It comes through in their relationships with bosses, romantic partners, or family members. It comes through in their near-constant, realistic fear of rape. It also comes through in how they see themselves. Since the toxicity does not refer to masculinity itself, one does not need masculine traits in order to exhibit its effects. A lot of women have implicitly bought into toxic conceptions.
Its expression in men is markedly different. Many men speak to their therapists about how difficult it is to be vulnerable without feeling like they’re not real men. But most men don’t speak to therapists, or anyone, about this at all. The toxic idea that men should never show signs of weakness, should never cry, and should never ask for help, is literally killing men.

The statistics consistently show that more women are depressed than men. However, twice as many men commit suicide. The disparity between the numbers mostly comes down to the simple fact that men are far less likely to admit to themselves or others that they are struggling.
It is in this and other ways that toxic masculinity harms men to such a degree as to be fatal.
Not All Masculinity Is Toxic (Not Even Most)
It is therefore imperative to note that masculinity in and of itself is not toxic. Many experts emphasize that there are many masculinities. There are many traits and even cultures that men and women consider masculine which are not toxic. Most of these “masculinities” are healthy and are to the detriment of neither men nor women.
Toxic Culture vs Toxic Masculinity
There are those who would rather we didn’t refer to it as toxic masculinity at all. They point out that it is not masculinity, or even one of many masculinities, that is toxic. Rather, it is a toxic culture of masculinity. Author Mark Greene explains the difference as such:
“Culture is a construct, formed and shaped by all of us. It represents not us as individuals, but a collective agreement on how we should behave.”
Calling it a culture makes the clear distinction that this is not something inherent in men or masculinity itself.
Hegemonic Masculinity
In gender studies, there is a concept known as hegemonic masculinity. This refers to a culture that legitimizes men’s dominance in society and justifies the subordination of women. It is a significant part of what most people think of when they hear or say the term toxic masculinity. It can be an implicitly held viewpoint, or a philosophy to which an individual knowingly subscribes.
What Can We Do About It?
Toxic masculinity, or the toxic culture of masculinity, is deeply rooted in most societies across the world. It is perceptible in gender norms, career expectations, work environments, and even the way we educate children. With this perspective, the concept may seem too overwhelming to counter.
However, a culture exists among individuals, and by making the choice to change your own ideas and behaviors, you make an immediate difference, regardless of your sex or gender.
From a psychological standpoint, therapy is the perfect space to carve out your individual sense of self. Therapy can therefore help you challenge your own beliefs about masculinity, particularly in how they manifest in your life. Women can learn how to see themselves without the lens of the culture. Men can learn to let go of the expectations which are holding them back.
We need a nuanced understanding of toxic masculinity in order to deal with its effects on both men and women. You can begin by challenging the way you think of masculinity, as it relates to yourself and others. November 5, 2018 / 0 Comments / by Joshua MarcusAbout The Author Joshua Marcus
Joshua Marcus is a South African freelance writer in the mental health niche and founder of TheEmpathyHub.com. Having both studied psychology and battled his own depression, he is passionate about spreading awareness of mental illness and its treatment. He is currently traveling through South-East Asia with his husband, Kyle.←Previous post Next post→
Popular PostsAre You Dealing with a Sociopath? Here’s How To Tell… March 10, 2018 Rejection Sensitive Dysphoria: A Tell-All Guide April 15, 2018 Gaslighting: Signs You’re Suffering From This Secret Form of Emotional Abuse March 16, 2018
Recent PostsCBD Gummies for Anxiety and Depression June 22, 2019 Chronic Illness and Mental Health: The Connection May 20, 2019 Mental Health Awareness Month (MHAM): #4Mind4Body May 20, 2019

ThriveTalk is a secure, effective and easy-to-use online therapy platform that connects clients with highly trained therapists and supports and empowers therapists to build online private practices. Feel free to contact us with any questions about our work: ask@thrivetalk.com
More About ThriveTalk
Contact us anytime
- 207 Calle Del Parque
San Juan, Puerto Rico 00907
If you’re dealing with an acute mental illness or are experiencing a potentially life-threatening issue do not use this website.
Please use these resources. © 2018 Altva Holdings LLC Terms of Use | Privacy Policy
How to Tell If You’re Experiencing Seasonal Affective Disorder Posted December 18th 2019
So how can you know if you’re experiencing SAD? Even if you’re not in the 18 to 30 age group, have never been diagnosed with depression and don’t live in a northern part of the world, it could still be something you’re experiencing.
“Some common signs of SAD include a lack of motivation, decreased desire to participate in the activities you once enjoyed, increased irritability, trouble concentrating or sleeping,” says Benton.
“The symptoms of SAD are the same as depression,” Richardson agrees. “The only difference is that the symptoms present more during the fall and winter months. If you begin to feel down or depressed, not interested in things you normally like to do, or find that your energy is overall low, you may have SAD — and should speak with a healthcare professional.”
How to Combat Seasonal Affective Disorder
Does the above sound like your experience of the colder months of the year? If so, you should know that you don’t have to suffer like this every time the temperature drops and the days begin to shorten — there are ways to combat SAD.
“Try adjusting your daily schedule to optimise the amount of time you spend in the sun, whether it’s taking a walk during your lunch break or adjusting your exercise schedule to work out in the morning instead of the evening,” suggests Benton. When daylight savings time occurs, there’s a change to your circadian rhythm which can increase symptoms of SAD, she explains. “To counteract the change, it’s important to become strict with your sleep schedule and set specific times to go to bed and wake up every day.”
Another factor that contributes to SAD is a lack of activity, says Benton. “It can be extremely easy to fall into a sedentary lifestyle during the winter and the holidays, so try to avoid sitting for long periods of time and aim to do something active every day. Additionally, many people find the use of a light therapy lamp, a lamp that emulates natural sunlight, very helpful.”
Richardson agrees that light therapy is a big part of combating SAD symptoms.
“Light therapy, also called phototherapy, can be used to counteract the lack of sunlight during the winter months and give a boost to your circadian rhythm. Try phototherapy by going for a walk outside in the daylight for 30 minutes. If that is a little too cold for you, you can also try a light box that you can place on your desk and get some synthetic sunshine before the start of your day.”
He also suggests approaching SAD with the same seriousness you’d approach non-seasonal depression — by trying out counseling and/or speaking to a medical professional to discuss possible medication.
“If you find that your mood is taking a turn for the worse, try counseling. A therapist can help you identify the exacerbating factors worsening your mood and help guide you through the winter months,” Richardson says. However, he notes, the best way to treat SAD is to prevent it from happening. “Bupropion, also known as Wellbutrin, is a type of antidepressant that has been found to prevent SAD when started in the fall,” he says.
That doesn’t mean it’s too late for you if the snow has already begun falling, though.
“If you are in the midst of the winter and think you have developed a case of SAD, selective serotonin reuptake inhibitors (SSRIs), such as Prozac, Zoloft, or Lexapro, are your first-line treatment options to help get you back on your feet,” Richardson says. “These medications are fairly safe, but talk with your doctor to discuss if these medications are right for you.”
A State Serving Psychiatrists View from the U.S follows this article Posted December 14th 2019 “Bad mistakes made by some psychiatrists and registrars inthe NHS” https://www.careopinion.org.uk/15824
About: North East London NHS Foundation Trust
On more than one occasion, I have been unfortunate enough to go to a psychiatric hospital because of having to cope with too much stress. On more than one occasion, I was not listened to by the doctor, who unfortunately listened to my father who I hadn’t seen for about 2 years previously and tried to keep away from him as much as possible. Unfortunately again the doctors didn’t know that my father has been a violent and abusive alcoholic and rather than listen to me, they took the opinion of my father. I then received the wrong medical treatment, which was very painful for me. After getting a solicitor involved (luckily the hospital had an advocacy department) and after a lot of unnecessary trauma to myself, I finally got another doctor to listen to me, I was then, after about three weeks, put on the correct medicine.
This has happened before to me. The same thing happened about 10 years previously. Due to having a nervous breakdown, mainly because of having lived in fear for years with a violent and abusive alcoholic father, I ended up in a serious condition when I was thrown out of the home by the alcoholic father. I couldn’t cope with the whole trauma of not having any money and being homeless, I eventually ended up in a psychiatric hospital – once again the alcoholic father was doing all the talking to the doctors there and I was not given the right treatment. The doctors never listened to me, and if only they had known what kind of man my father was, I don’t believe I would have got such bad treatment. Unfortunately, once dosed up on the wrong type of medication, I could not communicate with any staff about what had happened to me. I was in a practically comatose state much of the time, and lost the ability to talk and think properly. This is did not help my health or mental health and has had detrimental effects on my life to this day.
Another time quite recently, I went to an out-patient meeting with my boyfriend, the consultant psychiatrist was not available so I had to see his house-officer. I must admit I was a bit depressed, but this has proved now to be an under-active thyroid problem which I didn’t know at that time, but anyway this registrar would not listen to me and kept asking my boyfriend questions about me, which my boyfriend couldn’t really answer. The registrar was asking him personal questions about me like ‘does she do this or does she do that’ as if I was invisible. The fact is, I had only known my boyfriend a few months and really he couldn’t answer these questions. It was totally disgusting that I was being ignored by this doctor, as if I was invisible. What right had this doctor to ask someone else about me, when I was sitting right opposite him and could answer the questions myself?
I did complain to the consultant about this registrars manner, but it probably won’t make any difference. In my experience, all doctors need to be trained in how to care for their patients properly and to listen to the patient with respect, and not listen to people in the family who have a personality problem themselves and are dysfunctional people anyway, that have brought about another relative to have a nervous breakdown because of their dysfunctional and aggressive behaviour. I tried to get an injunction against my father interfering in my life because of the way things always go wrong when he is around but I couldn’t get one, and consequently doctors would rather listen to parents or anyone in the family that doesn’t like another member of the family, than the patient themselves. Not all family’s are o.k., a lot are dysfunctional, and probably most of the people that end up in a psychiatric hospital got there because something went wrong within their family. Then the worst thing happens, because other family members get it all wrong and the person that has had the breakdown doesn’t get listened to. And once drugged up on the wrong drug (due to the wrong information being given to the doctors) the patient is unable to communicate with the staff to explain anything at all. I have written a book about the awful treatment I have had via the psychiatric services over the last two decades called ‘To Hell and Back’ published by Chipmunka Publishers, it is in paperback and an e-book on the World Wide Web, so that people everywhere can see how stupid certain doctors are and what a waste of time giving someone the wrong drug treatment is, by waste of time I mean a waste of many years of living the life someone was given, because doctors didn’t give the proper treatment in the first place to the patient.
I hope you can read a copy of my book, this might help mental health services help individual like me to have a voice. Thanks.





Psychiatry, Mental Illness, and the State Posted here December 14th 2019

By Donald Devine September 25, 2014
Finally, we have a definitive discussion of the discipline of psychiatry, from an insider committed to the profession but who does not shy away from its profound difficulties. In Our Necessary Shadow: The Nature and Meaning of Psychiatry, Dr. Tom Burns reveals all even while insisting that at bottom “psychiatry is a major force for good.” Psychiatry is inherently controversial since it claims to know the psyche; but this touches, as he puts it, what “is most human in us,” our being, our “soul” which we cannot be neutral about. Psychiatry is a “hybrid” of “guided empathy” and detached cure—and the profession has swung wildly between them for years.
There is no unifying theory—“no –ology in psychiatry,” Burns concedes—only approaches that work for individual patients who are encouraged to take responsibility for themselves. Psychiatry itself is a medical discipline, one of the mind. It can prescribe medicines in the form of brain-altering chemicals, and recommend and sometimes perform surgery. It even has legal authority to decide when compulsory treatment is required. Psychiatrists normally utilize psychoanalysis (and psychological therapy generally) but these are also practiced by non-medical psychologists. Both treat mental diseases, normally classified as psychoses or neuroses. The former—schizophrenia, manic depression (bipolar disorder), paranoia—are more severe and were once labeled madness—with patients demonstrating very disturbed behavior and loss of contact with reality. The term neuroses is now somewhat unfashionable due to its over-diagnoses of normal depression but is different from manic depression in that the patient acknowledges a problem.
Mental illness has been with us since ancient times, treated by shamans, witch doctors, priests, fakes, hypnotists, and con men, many with wild theories and exaggerated promises of a cure. Medieval society basically left matters to families and some religious groups. It was not until what Michel Foucault called the “great confinement,” under the rationalizing influence of the 16th century Divine Right monarchies, that officials sought to control madmen considered dangerous to society by incarcerating them in small units. The more enlightened thinking of the 19th century produced warehousing asylums, the physician-mesmerizer Franz Mesmer, and the first professor of psychiatry in 1864, but with little measurable improvement. Burns concedes that “multiple personality” was invented by psychotherapists through the power of suggestion, and “recovered memory” (brainwashing) was routinely induced by doctors and social workers.
He observes that the field has “lurched widely,” being broadly biological, then almost exclusively psychoanalytic, then back to unapologetically biological today. At the beginning, ineffective surgery, limited drug success and treatment abuses tainted psychiatry. Sigmund Freud brought some respectability to the discipline but through psychoanalysis rather than medical psychiatry. Very different approaches to psychoanalysis were undertaken, by Freud himself, over time, and then by the other pioneers such as Alfred Adler and C.G. Jung. All had their proponents and achieved great popularity especially among intellectuals. Yet, by the close of the 20th century, the fact that each began with different theories, utilized dissimilar treatments, and garnered equally poor results led to today’s emphasis on psychiatry and biology rather than psychoanalysis. Burns, while generally supportive of the new emphasis, insists psychotherapy is not an “add-on” but essential to the field since all mental illness ultimately is social rather than simply biological.
Medicated treatment—its four main types being antidepressants, antipsychotics, sedatives, and mood stabilizers—increasingly dominates the field. The first breakthrough was using malaria to cure late-stage syphilis in the late 1880s, then insulin for drug addicts during withdrawal and for schizophrenia, then treating psychosis with electric shock, and finally going beyond to brain surgery. Burns recognizes the abuses at each stage but even defends lobotomies and electrically induced epileptic fits by recounting the relief they give to very disturbed individuals, not to mention their families. He is fair to critics of the whole endeavor like Foucault, Erving Goffman, and the libertarian Thomas Szasz, but concludes they have no answers to the fact that mental illness is real and causes great harm.
Our author is a surgeon and argues for psychiatry’s firmer grounding in biology. He tries to distinguish between “illness” and “disorder,” psychoses and neuroses, biology and mind, psychiatry and psychoanalysis so as to devise some comprehensive orienting theme for his discipline. But he finally concludes that one can make legal but not medical distinctions, since medically each is useful in different circumstances. While questioning the concept of recovered memory, for example, he still finds some legitimacy in the idea of dissociation. There are psychological differences between psychosis and neurosis but he is reluctant to call the former scientific/medical and the latter merely requiring counseling. Chemical treatment and surgery may seem more scientific but after both are exhausted, social problems must be resolved for full recovery. So the lines sometimes blur, and in service of that point he notes that sympathetic counseling used by Quaker and religious nuns inspired early psychoanalysis. Also that treating folks patiently and decently is still the secret of success today.
Medicalizing all of life’s ordinary difficulties is our tendency today, and this concerns the author. Why not, he rhetorically asks, Prozac all the time for everyone? It would calm us all down; but at what cost to our humanity? Indeed he asks whether “psychiatry itself” isn’t “making us sicker?” He notes that in the United States, 10 percent of 10-year-old-boys are diagnosed with Attention Deficit Hyperactivity Disorder, which “surely cannot make sense,” and which in many cases is merely used to stop boys from being boys. He questions whether even alcoholism is a medical rather than a social disorder in most cases (although psychoanalysis can be helpful).
The fact that the psychiatric profession itself has expanded the number of mental illnesses from 106 in 1952 to 297 in 1994–an almost 300 percent increase—undermines its own claim to be a scientific discipline. “Of course,” he says “this does not mean that there are really hundreds more disorders” or that psychiatrists end up even using all of these categories.
Psychoanalysis is especially liable to abuse. Two-thirds of patients are women despite that mental illness, generally, seems roughly equal between the sexes. Even with increasing public criticism of over-diagnosis, demand for psychoanalysis remains high, especially if third parties or government bear the cost. People like a shoulder for comfort. Yet the “extreme dependency” of the patient in such settings and the profession’s skepticism of customary moral taboos makes such sessions open to abuse. A few therapists even justify close sexual relationships with patients. Beyond that, ill patients are often not able to make decisions and these must be turned over to families. Mothers tend to stick with the patient but many family members simply want the situation solved no matter the nature of the treatment or the risk to the patient.
Government is inevitably involved in such situations. “Compulsory community treatment” orders for a year or two are the current favorite but are expensive and have the obvious Catch 22, says Burns, that whether the patient improves or not, additional treatment is offered as the solution.
In the end, he writes, psychology is simply the “practical response to the reality of mental illness.” The fact of limited success is balanced against the real anguish of patients, parents, relatives, and friends. The mind is so complex there are no cut and dried solutions—but society still demands them. Psychological evaluations are required by legislators and judges to help them keep order and make distinctions between “mad and bad.” It is governmental officials and society more than psychiatrists who insist on medical support for compulsion. Even though Burns’ own study of compulsory treatment orders in Britain found “absolutely no effect” on recovery, he finds that compulsion is “inevitable” since few will accept Szasz’s solution of treating the mentally ill the same as ordinary criminals. Neuropsychology and gene research promise refinement of diagnosis in the future but Burns confesses to being “unaware of any philosophical breakthrough in understanding the mystery of consciousness and identity.”
Refinement certainly does not characterize how the totalitarians addressed this issue. Between 1939 and 1945, 200,000 people were diagnosed as incurably mentally ill and ordered medically euthanized by the Nazi Committee for the Scientific Treatment of Severe, Genetically Determined Illnesses. The Soviet Union routinely classified political dissidents as mentally ill, certified by the appropriate psychiatric physicians. Burns adds that it was not only the bad guys:
The systematic extermination of the mentally ill was a terrible consequence of more long-standing eugenic ideas which had been gaining strength in Europe, the UK and the USA for decades. “Social Darwinism,” and a moral panic that the unfit were “breeding” faster than the educated and able, had become a preoccupation at the turn of the 20th Century. It is never far from the surface, even now.
Forward-thinking Sweden sterilized over 60,000. The “enhanced interrogation” undertaken by the U.S. government after the attacks of September 11, 2001 was supervised by psychiatric physicians.
Reflecting on the Nazi abuses, Burns asks: “How could such a terrible thing happen and why was there no effective opposition from psychiatry? For there was none.” The only opposition was from some families and the church. After all, it was “scientific.” Even in the United States, the American poet Ezra Pound was confined to Saint Elizabeth’s Hospital in Washington, D.C. as “unbalanced” but mainly for being an open fascist sympathizer. Burns notes the “witch hunts” claiming child abuse from “recovered memory” children in the United States during the 1980s and 1990s. He is concerned about the “current dangers” of “commercial and social pressures.” Still, he expresses himself “relatively hopeful that psychiatry is unlikely to be such an obviously unwitting tool of state oppression again. We have learned our lesson and the profession is now more open and international.”
Two “errors” of early psychiatry highlighted by Burns suggest the difficulties that remain, and the profession’s enduring temptation to bend to public or elite opinion. Until 1973, homosexuality was listed by psychiatry as a mental illness. Today, it is considered normal and those who oppose it are labeled homophobic. Discrimination against homosexuals today is often punished by legal authorities and homophobia has even been recognized by professionals as a contributing factor to mental illness. Some states forbid psychiatric treatment to “reverse” homosexuality. It took the profession 40 years to turn homosexuality from a serious disorder to now requiring government to protect it.
Burns is also disturbed by early psychiatry’s treating women as mentally different from men, somewhat as inferior beings. But while noting many more women demand psychotherapy, he is careful not to blame either them or therapists. “Who is influencing whom can be debated,” he writes. He is ambivalent as to whether there actually is a mental difference between the sexes. One suspects that there would be no more opposition to the currently “correct” decision from the American Psychiatric Association today than there was back in the early 20th century.
The author’s warning that eugenics and Social Darwinism are “never far from the surface, even now” cannot be ignored. He makes very clear that psychiatry has no single view of human nature. There is no theory. It is empirical, relative to a given situation. So what is to keep it within limits? Ewen Cameron earned the presidency of the American and the international psychiatric associations claiming that the brain was simply a computer. He worked for the CIA and the Canadian government in the 1950s to change usually unwilling patients’ minds by applying electroshock twice a day (versus the norm of three times a week) to break all “incorrect” brain pathways and create “correct” patterns. The project was carried on by Canada’s McGill University into the 1960s, with no opposition from government, the academy, or the profession.
The fundamental problem is that Burns’ more traditional view that mind and brain are not the same is a minority opinion in government, in the academy, and in psychiatry. For Darwin there was no “mind,” only the evolved animal brain. Burns has done a great service in highlighting the dilemma that it is not really easier now to cure mental illness, to distinguish “mad” from “bad,” or to limit compulsion. Compulsion and not-fully-informed patients are inherent in the discipline—indeed have produced its most important advances. While he is right to defend psychiatry’s positive achievements, it is questionable whether a field of endeavor that has no theory to guide it has learned or ever can learn its lesson.
Donald Devine is senior scholar at the Fund for American Studies, the author of America’s Way Back: Reconciling Freedom, Tradition and Constitution, and was Ronald Reagan’s director of the U.S. Office of Personnel Management during his first term. This article originally appeared at The Liberty Law Forum. Photo Shutterstock Alfred AdlerC.G. JungDr. Tom BurnsMichel FoucaultNazisProzacSigmund FreudThomas Szasz
Copyright © 2019 The Federalist, a wholly independent division of FDRLST Media, All Rights Reserved.14 Comments


Copyright © 2019 The Federalist, a wholly independent division of FDRLST Media, All Rights Reserved.
One Flew Over the Cuckoo’s Nest by Ken Keasey- a summary posted December 11th 2019
Chief Bromden, the half-Indian narrator of One Flew Over the Cuckoo’s Nest, has been a patient in an Oregon psychiatric hospital for ten years. His paranoia is evident from the first lines of the book, and he suffers from hallucinations and delusions. Bromden’s worldview is dominated by his fear of what he calls the Combine, a huge conglomeration that controls society and forces people into conformity. Bromden pretends to be deaf and dumb and tries to go unnoticed, even though he is six feet seven inches tall.
The mental patients, all male, are divided into Acutes, who can be cured, and Chronics, who cannot be cured. They are ruled by Nurse Ratched, a former army nurse who runs the ward with harsh, mechanical precision. During daily Group Meetings, she encourages the Acutes to attack each other in their most vulnerable places, shaming them into submission. If a patient rebels, he is sent to receive electroshock treatments and sometimes a lobotomy, even though both practices have fallen out of favor with the medical community.
When Randle McMurphy arrives as a transfer from the Pendleton Work Farm, Bromden senses that something is different about him. McMurphy swaggers into the ward and introduces himself as a gambling man with a zest for women and cards. After McMurphy experiences his first Group Meeting, he tells the patients that Nurse Ratched is a ball-cutter. The other patients tell him that there is no defying her, because in their eyes she is an all-powerful force. McMurphy makes a bet that he can make Ratched lose her temper within a week.
At first, the confrontations between Ratched and McMurphy provide entertainment for the other patients. McMurphy’s insubordination, however, soon stimulates the rest of them into rebellion. The success of his bet hinges on a failed vote to change the television schedule to show the World Series, which is on during the time allotted for cleaning chores. McMurphy stages a protest by sitting in front of the blank television instead of doing his work, and one by one the other patients join him. Nurse Ratched loses control and screams at them. Bromden observes that an outsider would think all of them were crazy, including the nurse.
In Part II, McMurphy, flush with victory, taunts Nurse Ratched and the staff with abandon. Everyone expects him to get sent to the Disturbed ward, but Nurse Ratched keeps him in the regular ward, thinking the patients will soon see that he is just as cowardly as everyone else. McMurphy eventually learns that involuntarily committed patients are stuck in the hospital until the staff decides they are cured. When McMurphy realizes that he is at Nurse Ratched’s mercy, he begins to submit to her authority. By this time, however, he has unintentionally become the leader for the other patients, and they are confused when he stops standing up for them. Cheswick, dismayed when McMurphy fails to join him in a stand against Nurse Ratched, drowns in the pool in a possible suicide.
Cheswick’s death signals to McMurphy that he has unwittingly taken on the responsibility of rehabilitating the other patients. He also witnesses the harsh reality of electroshock therapy and becomes genuinely frightened by the power wielded by the staff. The weight of his obligation to the other patients and his fear for his own life begins to wear down his strength and his sanity. Nevertheless, in Part III, McMurphy arranges a fishing trip for himself and ten other patients. He shows them how to defuse the hostility of the outside world and enables them to feel powerful and masculine as they catch large fish without his help. He also arranges for Billy Bibbit to lose his virginity later in the novel, by making a date between Billy and Candy Starr, a prostitute from Portland.
Back on the ward in Part IV, McMurphy reignites the rebellion by getting into a fistfight with the aides to defend George Sorenson. Bromden joins in, and they are both sent to the Disturbed ward for electroshock therapy. McMurphy acts as if the shock treatments do not affect him, and his heroic reputation grows. Nurse Ratched brings him back to the ward so the other patients can see his weakened state. The patients urge McMurphy to escape, but he has arranged Billy’s date for that night, and he refuses to let Billy down. McMurphy bribes Mr. Turkle, the night aide, to sneak Candy into the hospital, and they have a party on the ward. Billy has sex with Candy while McMurphy and the other patients smoke marijuana and drink. Harding tries to get McMurphy to escape with Candy and Sandy to Mexico, but McMurphy is too wasted and falls asleep.
The aides discover the mess the next morning, setting off a series of violent events. When Nurse Ratched finds Billy with Candy, she threatens to tell Billy’s mother. Billy becomes hysterical and commits suicide by cutting his throat. McMurphy attacks Ratched, ripping open the front of her dress and attempting to strangle her. In retaliation, she has him lobotomized, and he returns to the ward as a vegetable. However, Ratched has lost her tyrannical power over the ward. The patients transfer to other wards or check themselves out of the hospital. Bromden suffocates McMurphy in his bed, enabling him to die with some dignity rather than live as a symbol of Ratched’s power. Bromden, having recovered the immense strength that he had believed lost during his time in the mental ward, escapes from the hospital by breaking through a window.
Sourece www.sparknotes.com
Editorial Comment No one in their right mind should evert talk to a psychologist or psychiatrist. they will always declare you as suffering from some sort of mental illness/syndrome. Robert Cook
June 27, 2016
10 Things That Could Get You Sent To An Insane Asylum Posted December 11th 2019


50 Comments
Insane asylums were big business back in the early 1900s, and nearly anyone could be declared “insane” and sent to an asylum. In a newspaper report from 1903, an asylum physician admits:
A person to be tried in Kentucky for lunacy is often hauled before a jury of as ignorant, illiterate, indiscriminating men as you could find in a month’s journey. The officers go out and just pick up anybody. Who would want his sanity passed on by the rakings and scrapings of creation?
Brutal words but apparently truthful. Getting placed in an asylum 100 years ago was as easy as dressing in the “wrong” clothes or speeding in your car.
10 Speeding

Are you nuts for speeding? Back in 1922, you might have had your head checked if caught speeding in Detroit, although some judges would have just thrown you in jail. A headline in one newspaper read: “Sanity Test for Detroit Auto Speeders.”
If any speeder failed the examination given by the court psychiatrist, he or she would be sent to an asylum for “treatment.” Just what exactly that treatment was is left to the imagination. These same speeders would also lose their driver’s license and would not be allowed to apply for a new one.
One judge stated:
I believe this new method will stop thousands of accidents each year. [The] Police Commissioner . . . has told me that under my plan of sending speeders to jail, and notwithstanding the fact that there are many thousands more automobiles on the streets this year than last year, there were 3,301 less accidents and that reckless driving has been cut down to 50 percent from 80 percent. If this is the result under my jail sentence plan, what will it be under the mental test plan?
9 Too Much Studying

Can you study your way into an insane asylum? While you might have felt like you were going nuts when studying for final exams, I bet you never knew that some minds can break under the strain. This was especially true of female minds back in 1915.
The Day Book, a newspaper out of Chicago, reported that two sisters had been sent to an asylum under orders from a county judge. Apparently, the poor dears were hard at work studying the doctrines of Christian Science and their “minds broke down.”
Christian Science was founded in 1879. It was started by Mary Baker Eddy when she and 15 followers founded the Church of Christ. It is a religion that is still practiced today and is widely known for its controversial faith healing. Christian Scientists favor prayer and homeopathy over modern medicine and are often the subject of news reports when a child is being denied necessary medical care.
8 Reading In The Morning

Come on, ladies. Not only should you avoid studying because it will drive you insane but getting caught reading a book is also proof that there is something wrong with you.
The following snippet sounds like something from out of a dictatorship where everyone’s moves must be controlled. Sadly, this report came out of Chicago in 1915: “Alice Ostwald . . . found on corner at 5:00 AM reading novel. Sent to insane asylum.”
This could have easily been any avid book reader. When a book is just that good, there will be no sleeping until the last page is read. Why was she at a street corner, though? Probably for the light. Street lamps were probably the only light some people had at night, especially if they were poor.
It could have been that she was catching up on some reading before going to work in one of the many factories in Chicago during those times. Regardless of the reason, it seems rather extreme to send someone away simply for reading a book in the morning.
7 Having A Drunken Father

In 1913, The Day Book published an unsettling report titled: “Shall We Build More Asylums Or Stop Breeding Epileptic, Idiotic, And Insane Children?” In the article, the reporter investigated the root cause of the increase of “insane” children and the need to build more institutions.
He found that poverty and a drunken father was the cause of “idiotic” children. He presented the common case of a poor wife and mother who is brought into the juvenile court with her six children. She has no money for food or rent, and her husband is a drunk. She wants to leave her husband but can’t because she needs the few dollars he sometimes provides his family each month.
The judge is then faced with a tough decision. According to the article:
Two roads lie open before the judge, who hates to take either of them. He can order the mother to kiss her children goodbye forever and put them into an asylum. Or he can reprimand the drunken father, order him to support his family, and send the wife and mother back to live with him.
In other words, while there was no actual proof that any of these children were “insane,” they could still be sent to an asylum for circumstances beyond their control.
6 Being Poor

Old newspapers are filled with accounts of poor people being sent to insane asylums. This often happened to women who had to rely on a husband’s income if they wanted to survive.
In 1913, there was an account of a woman who had worked as a stenographer. At 45 years old, she came to a “critical period in her life, she was unable to work.” She took the time off that she needed but eventually ran out of money.
She turned to a group called United Charities for help, and they immediately had her judged insane and sent to an asylum. She was held there as a prisoner for five years. At age 50, she was released and went on to sue the “county for false imprisonment.”
In another tragic story from 1921, an African-American woman was found wandering the streets in her bare feet, carrying her five-month-old baby in her arms. Both the mother and the infant were placed in an insane asylum simply because the woman’s sister had also been placed in one before this incident.
One can only assume that the woman was without funds or the help she needed to raise a small child. Instead of getting her real help, she was sent away, out of sight and mind.
5 Dressing Like A Man

Photo credit: Underwood & Underwood
Right now, people have their panties in a bunch over transgendered people using the “wrong” bathrooms. Back in the early 1900s, however, transgendered people would have been placed in insane asylums.
Proof of this exists in the little tidbit news lines found in newspapers 100 years ago. One morsel found in a 1916 paper read, “Mrs. Emma Miller . . . sent to insane asylum. Put on pants and worked as man.”
While there is no proof that she was transgendered, it is interesting that people at the time were offended by a woman who would dare dress like a man, let alone work like one. Sadly enough, in those times, women could not earn enough money to survive on their own as women. They had to marry to survive.
The woman in the above snippet was obviously married, but she may have been widowed or may have simply needed to contribute more income to the family to survive. None of these details were given in the article. All the people cared about was that she dressed and worked like a man. How crazy is that?
4 Epilepsy

Photo credit: Wellcome Images
Epilepsy used to be (and sometimes still is) blamed on demonic possession. But over 100 years ago, people who exhibited signs of epilepsy were often sent away to the insane asylum if a family member didn’t feel like taking the person into their full-time care.
In 1895, Mrs. Mary Brown was judged as having an unsound mind and was sent to an asylum. The reason given was that “she is subject to epilepsy and was seriously burned last spring by falling in the fire during an attack.”
Assuming that she was not a widow, one has to wonder if it was the husband who pushed for the insanity judgment so that he wouldn’t have to take care of his wife, which often happened in those times. Since epilepsy cannot be cured, many victims of the disease were probably left in asylums and forgotten over time.
3 Having Sex With A Jerk

Photo credit: Dante Gabriel Rossetti
In 1896, a report came out about a young woman who had a thing for old men. She had apparently gotten in trouble for her desire for older men in the past, but that didn’t stop her. She eventually met a “well-known old man” and claimed that they had sex. She wanted him to make the situation right and marry her.
The man refused and “charged her with insanity.” The young woman was examined, and “the commissioners concluded that she was crazy and ordered her sent to the asylum.” Some time later, it was discovered that she was pregnant.
The asylum could no longer keep the young woman because the asylum was not a safe place for a pregnant woman, not to mention that “someone” obviously had had sex with her as she had claimed. The young woman was returned to the county, and no further details were given about what happened to her.
2 Not Being Able To Work Long Hours

Photo via Wikimedia
In 1915, workers were trying to get the eight-hour workday passed so that they weren’t forced to work 10 or more hours a day, six days a week. Employers were against the eight-hour day because it would mean that they would have to hire more people to work around the clock. This would translate into less money in the owners’ pockets.
One lawyer for the Associated Employer’s Association felt that “workers who could not work the number of hours required by the employers should be examined by a physician and, if not able to do the work, should be sent to the state asylum to be taken care of.”
With people being sent to insane asylums for the lamest reasons, this threat to check people’s mental states was probably enough to scare quite a few workers into silence.
1 Annoying The Wrong Person

In the early 1900s, you had to be careful whom you annoyed. Take, for instance, Mrs. Helen Pike. She was sent to an insane asylum for annoying a streetcar magnate in 1917. No reason was given as to why she was annoying the man or how he found her annoying. She was simply taken before the courts and sent to an asylum.
Of course, that is not as bad as annoying the president of the United States. In 1916, Richard Cullen was sent to an asylum, possibly for life, because the youth “made persistent efforts yesterday to reach President Wilson while [the] chief executive was on [an] automobile tour of [the] city.”
The young man was declared insane and became an “inmate of [the] Marshalsea, Allegheny County institution for [the] insane.” Nowhere did the article state that he was somehow threatening the president. He was simply trying to get his attention.
Elizabeth spends most of her time surrounded by dusty, smelly, old books in a room she refers to as her personal nirvana. She’s been writing about strange “stuff” since 1997 and enjoys traveling to historical sights. Source Listverse
‘Under-reported’ use of anti-psychotic drugs
17 October 2012
The scale of the challenge to reduce the use of anti-psychotic drugs by people with dementia may be under-estimated, according to researchers from Aston University and the University of East Anglia, working with NHS Kent and Medway.
There is a key public health challenge to reduce the prescribing of anti-psychotic drugs to people with dementia as they are thought to be associated with up to 1,800 deaths a year.
Ian Maidment, corresponding author and a Senior Lecturer in Clinical Pharmacy from Aston University has worked in medication management in dementia for 20 years states: ‘The true scale of anti-psychotic usage in dementia may be under-estimated. Usage may be up to 46% greater than official figures suggest.’
The researchers compared the results of the government’s National Dementia and Anti-Psychotic Prescribing Audit with research, led by Anne Child, an experienced senior clinical pharmacist for NHS Kent and Medway cluster of primary care trusts (PCTs). They found that 15.3% of people with dementia received an anti-psychotic, compared to the national audit, which found 10.5%. However, only 48.9 per cent of GP practices across the country participated in the national audit compared with 98.3 per cent of practices in Medway which took part in the detailed local study.
The Medway project, carried out from January to December 2011, and analysed by researchers from Aston University and the University of East Anglia, identified that
·People with dementia living in care homes were nearly 3.5 times more likely to receive a low-dose anti-psychotic than people living at home (25.5 per cent compared to 7.3 per cent)
· It was possible to reduce or withdraw low-dose anti-psychotics for more than 60 per cent of patients with dementia (43 out of 70) whose medication was initiated by their GP.
· Clinical trials need to be commissioned as a matter of urgency to confirm the effectiveness of pharmacist medication reviews.
The paper, which appears in the BioMed Central’s open access journal BMC Psychiatry, also sets out the detailed process undertaken before and during withdrawal of anti-psychotics from patients.
Anne Child, primary author, who is now Head of Pharmaceutical Care at Avante Care and Support said: ‘We have demonstrated that a multi-disciplinary approach to dementia care, involving a pharmacy-led medication review, GPs, and care homes, can produce a positive outcome for patients, in one region of the country. More work is now needed.’
Dr Chris Fox, co-author, from UEA’s Norwich Medical School said: ‘Another issue with the national audit is it fails to report the usage of the drug lorazepam, which is sometimes used instead of anti-psychotics. It is potentially equally dangerous. Until we capture the true level of usage of all these drugs we cannot truly understand the issue.’
Ian Maidment added: ‘Whilst the national audit is an important first step, it presents a partial picture. If we rely on it, exclusively we are doing a disservice to people with dementia, their carers and their families.’
-ends
For further media information contact Alex Earnshaw Aston University Communications on 0121 204 4549
For further details or to interview Doctor Chris Fox please contact Lisa Horton UEA Press Office on 0160 359 2764
Article available on http://www.biomedcentral.com/content/pdf/1471-244X-12-155.pdf
Psychiatry & Psychotherapy Podcast
The History and Use of Antipsychotics
psychiatry podcast, psychotherapy podcast
sign up for an annual subscription to receive CME credit for this activity and more! Learn more Here.
Link to show on: iTunes, Google Play, Stitcher, Overcast, PlayerFM, PodBean, TuneIn, Podtail, Blubrry, Podfanatic
In my last post, Dr. Cummings and I talked about what psychopharmacology is, how medicine works in our body, and what factors affect medicine absorption rates.
In the latest podcast, Dr. Cummings and I talked about antipsychotics, the particular branch of psychopharmacology that deals with medicines that treat psychotic experiences and other mental disorders, such as:
- Schizophrenia
- Severe depression
- Severe anxiety
- Bipolar disorder
- Psychosis exhibiting hallucinations and delusions
The history of first generation antipsychotics
The use of antipsychotics as medication began in 1933 in France. The research around developing antihistamines evolved into the introduction of promethazine. This drug produced sedative side effects, so doctors started prescribing it before surgeries as a calming agent.
Eventually, a doctor studied the derivatives of promethazine, altered it, and developed chlorpromazine. It was mostly used as a pre-surgery anti-anxiety pill, until psychiatrists took note of the calming effect of the drug and began prescribing it to their patients.
Prior to chlorpromazine, the options for treating psychotic patients were electroconvulsive therapy, hydrotherapy, and putting patients in an insulin coma. None of those are antipsychotic in nature.
When two psychiatrists, Dr. Delay and Dr. Deniker, gave 38 psychotic patients a test round of chlorpromazine, they noticed the patients were calmer, and also less psychotic—they had less delusional thinking, fewer hallucinations, and fewer psychomotor-agitation symptoms. Deniker and Delay began giving talks on the benefits of the drug, and in 1955, chlorpromazine became available in the United States. Chlorpromazine is still used today as a treatment for different mental illnesses and mood disorders.
Once the government saw the positive effects of chlorpromazine, it began to shut down mental health facilities. There was no longer as large of a need to house psychotic patients, and they saw an opportunity to cut costs. However, they did not create adequate sources in the community for ongoing care. California alone is estimated to have 40-60% of homeless people that have a mental disorder.
Once chlorpromazine became a success, pharmaceutical companies rushed to create their own version of an antipsychotic drug. Because chlorpromazine was the grandfather of the first generation of antipsychotic drugs, the rest of that generation can be categorized by their ability to merely block dopamine D2 receptors in the brain.
In repeated studies, dopamine antagonism is responsible for 92% of their effectiveness. It also led to the thought that people were psychotic because they had too much dopamine. Since then we have found that their are much more complex psychopharmacological dynamics going on in psychosis.
Second generation antipsychotics
The next set of antipsychotics that came on the market were clozapine, olanzapine, risperidone, and other related drugs. Those medications had less effects on motor movement than the first generation drugs.
Clozapine is a poor antagonist of dopamine- blocking 30-40% of dopamine receptors but also promotes the activation of glutamate through activation of NMDA receptor, which increases activity in the frontal lobe (which helps with schizophrenia’s negative symptoms).
Clozapine had more system-wide changes than just dopamine suppression, and it had more positive response from patients. It was more effective—40-60% of people who won’t respond to a first generation antipsychotic, do respond to clozapine.
However, in Finland in 1975, 6 people taking clozapine died due to agranulocytosis (lowered white blood cell count, leading to a severe lack of immunity). A lowered neutrophil count (called agranulocytosis) can show potential problems with fighting off normal bacteria we live with all the time. When patients are on clozapine, initially they need weekly blood checks for this reason.
Despite the risks, clozapine can be an incredible drug—I have one patient who was schizophrenic and homeless, and she is now back in school and recently graduated with a perfect GPA! People who had been dysfunctional for decades, who are given clozapine, can become extremely high functioning. Key to success here was her willingness to work with me, despite having to try different things before something worked.
A trial run on a antipsychotic should be done at a minimum of 6 weeks, and blood tests must be conducted to make sure that the concentration of the medicine is at good therapeutic-dose levels. Dosage alone is sometimes not enough because we all metabolise drugs so differently. I have uploaded recommended levels in my resource page.
Third generation antipsychotics
What is deemed the third generation of antipsychotics, aripiprazole and brexpiprazole are partial dopamine receptor agonists. They keep dopamine at a max of 25% in the brain which due to the high affinity to the receptor it does not vary much based on dose.
The good thing about this generation of drugs is that they don’t lower blood pressure, cause insulin resistance, and are not sedating in nature.
It works for some people, it doesn’t for others. But when it does work, it works really well.
Side effects of psychiatric medicines
Akathisia is the inability to stay still, characterized by a feeling of inner busyness. It is a miserable side effect, exhausting to the patient.
If someone is experiencing this, they should immediately call their psychiatrist or go to an emergency room.
One of Dr. Cumming’s patients described it as “ants running up and down the bones of his legs.” It usually involves an anxious feeling, and a desire to move the lower extremities of the legs. Akathisia can be caused by any drug that lowers dopamine (including SSRIs).
This syndrome is so complex because it involves several compounds, including dopamine, norepinephrine, acetylcholine, and serotonin inputs. Options for treatment include: choosing a lower dosage, picking another dopamine antagonist that is less strong (quetiapine or clozaril), or prescribing a drug like amantadine, propranolol, mirtazapine or clonazepam (more nuance in the podcast on this).
It is a harmful disorder, and one to watch out for in patients. If a patient is sent home from the hospital experiencing these symptoms, but is not properly vetted for akathisia, a doctor could be subject to serious legal repercussions.
The questions to test a patient for akathisia are:
- Is the person moving? Can they not sit still?
- What is their internal sense of restlessness and anxiety?
- How much are they distressed by these feelings?
Acute dystonia involves muscle spasms and it affects movement, causing the posture to twist abnormally. It can be painful for patients to experience. This occurs because of too little dopamine in the basal ganglia part of the brain.
Parkinsonism involves muscle stiffness and slower movements. It’s usually uncomfortable, but not a miserable side effect. This also occurs because of too little dopamine in the basal ganglia part of the brain.
The future of antipsychotics
With each generation of new medicines, we’ve gotten closer to being able to help people stabilize their psychosis. We haven’t been able to achieve complete wellness.
Dr. Cummings says he has hope that with further advances in the medical field, we will be able to identify who is at risk. There is hopeful data that we may be able to one day prevent the development of schizophrenia.
History of Antipsychotics (notes by Arvy Tj Wuysang).
- 1933, France
- Initiative to develop antihistamine as treatment began
- 1947
- Promethazine
- Produced sedation and calmness in animal models
- Not highly effective in humans, but found to provide calmness in preoperative settings
- Promethazine
- 1950
- Discovery of Promethazine Derivatives, especially Chlorpromazine
- Initially tried in a surgical military hospital in France by Dr. Henri Laborit (1914-1995)
- Successful in making people calm and indifferent to impending surgery
- The medication was tried it in a volunteer
- The individual reported favorable effects, until he stood up and promptly fainted
- Determined as not safe in pre-operative setting because it was too effective as alpha-adrenergic antagonist in lowering blood pressure
- Discovery of Promethazine Derivatives, especially Chlorpromazine
- 1952
- Dr. Pierre Deniker (1917-1998), psychiatrist, with Dr. Jean Delay (1907-1987), his superintendent in Sainte-Anne’s Hospital in Paris, led the Chlorpromazine introduction as a psychopharmacologic agent
- They were interested in the calming effect of the drug
- Tried the drug in psychotic agitated patients
- Treatment options in those days were limited to:
- Electroconvulsive Therapy
- Hydrotherapy
- Insulin coma
- None of which were antipsychotic in nature
- Treatment options in those days were limited to:
- Tried it in 38 patients, made patients calmer, and less psychotic!
- Especially effective for positive psychotic symptoms like hallucinations, delusional thinking, psychomotor agitation
- Findings were impressive enough that Deniker began giving talks about the drug, including a conference in Montreal, that led to its introduction in North America
- Dr. Pierre Deniker (1917-1998), psychiatrist, with Dr. Jean Delay (1907-1987), his superintendent in Sainte-Anne’s Hospital in Paris, led the Chlorpromazine introduction as a psychopharmacologic agent
- 1955
- Chlorpromazine was approved for usage as antipsychotic in the US
- Subsequently used worldwide
- Led to the deinstitutionalization of a lot of psychotic patients
- Created a problem of lack of follow up of psychotic patients
- I.e. California has around 357,000 homeless individuals, estimated 40-60% suffer from mental disorder with schizophrenia spectrum highly represented in that percentage
- State spends about $200,000 per year per person to care for people committed to state hospitals. Funds committed to patients that are discharged from state hospitals are very minimal.
- Created a problem of lack of follow up of psychotic patients
- Led to development of a whole host of antipsychotic agents
- 1960s
- There was an explosion in the invention of antipsychotic drugs
- US FDA took a stance, did not allow approval of antipsychotic drugs that are not clearly better than chlorpromazine or haloperidol
- 1st generation antipsychotics all work by blocking Dopamine D2 receptors in the brain, counts for 92-23% of variance in mechanism
- Led to the simplistic dopamine hypothesis of psychosis
- 1958
- 2nd generation antipsychotic discovered by Eichenberger and Schmutz from the Swiss pharmaceutical company Wander AG, Clozapine
- Created because 2 other -antadine antipsychotics have been successful, Loxitane (Loxapine) and Perlapine
- Clozapine was initially thought of as a failure because it did not produce dystonia in white lab mice, as expected in 1st generation antipsychotics where it blocks dopamine effects in the brain
- Clozapine found to be a poor antagonist to dopamine, only blocks 30-40% of dopamine receptors. Although, it promotes release of glutamate, by binding to an allosteric site for glycine in the NMDA receptor, which in turn increases activity in the frontal lobe and suppresses dopamine release in the mesolimbic system.
- A number of small studies in the 1960s found that patients that don’t respond to 1st generation antipsychotics responded well to Clozapine treatment by showing better response of both positive and negative symptoms of schizophrenia.
- 1970s
- 1972, Clozapine usage was introduced in Austria
- 1974, Clozapine usage was introduced in Germany
- 40-60% of people that did not respond well to 1st generation antipsychotics, responded well to Clozapine
- 1975, 5 people in Finland died after Clozapine treatment due to agranulocytosis
- Clozapine found to trigger formation of antibodies targeting bone marrow cells that make neutrophils and essentially shut down a person’s immune system
- Must monitor Absolute Neutrophil Count closely when prescribing Clozapine
- Monitor weekly for 6 months, then every 2 weeks for another 6 months, and monthly for another year (in the USA)
- Risk for agranulocytosis decreases with time: peaks at 4 months of exposure at about 1.3%, .38% after 1 year of exposure, .06% after 2 years of exposure
- Clozapine usage in the US today
- Siskind, D., McCartney, L., Goldschlager, R., & Kisely, S. (2016). Clozapine v. first-and second-generation antipsychotics in treatment-refractory schizophrenia: systematic review and meta-analysis. The British Journal of Psychiatry, 209(5), 385-392.
- 15-20% of patients in California State Hospitals are on Clozapine, 53% in New York State
- Response rates to drugs other than Clozapine is pretty miserable in State Hospitals
- Olanzapine response rate even at high plasma concentrations is only 9%, compared to 40-60% for Clozapine. Every other antipsychotics’ response rate is between 0-5% for the severely psychotic, mentally ill patients.
- If patients meet Kane criteria (after John M. Kane)—treatment failure after two clearly adequate trials of antipsychotic treatment with minimum of 6 weeks duration with therapeutic plasma concentration—odds that they will respond to anything other than Clozapine is fairly low.
- Common mistake that clinicians make is to go by dosage as a measure of whether a person is receiving adequate medication
- Dosages only weakly correlates with plasma concentration since the metabolism of antipsychotic drugs is so variable
- Measuring plasma concentration to reach therapeutic levels is crucial in antipsychotic drugs administration, especially in patients who are seemingly refractory to treatment, to ensure adequate treatment
- Akathisia as side effect of antipsychotics
- Very rarely happens with Clozapine use
- Akathisia is a very miserable side effect of antipsychotics, described as “ants crawling up and down the bone of your legs” by a particular patient
- Characterized both by internal sense of anxiety and a near irresistible urge to move
- Barnes Akathisia Rating Scale, most commonly used to measure akathisia symptoms. Based on three main factors:
- Objective movement
- Internal sense of restlessness and anxiety
- How much are they distressed by these feelings
- Akathisia is a concerning and common reason for malpractice
- Underlying pathophysiology of akathisia is distinct compared to other extrapyramidal symptoms, involves not only dopamine and acetylcholine. It also involves norepinephrine and serotonin inputs to basal ganglia, makes it a difficult syndrome to treat successfully.
- Treatment options for akathisia:
- Use a less robust dopamine antagonist, such as Quetiapine or Clozapine
- Use lower dose of the antipsychotic
- Use Amantadine, increases dopamine release in the basal ganglia
- Was originally devised to treat influenza A
- Discovered to be effective in treating extrapyramidal symptoms, also effective for tardive dyskinesias (15% respond to amantadine)
- However, it is not as effective as B-blockers or Mirtazapine
- Amantadine is not anticholinergic (no memory problems, no GI side effects, no blurred vision, no urinary retention)
- Head-to-head trial between Propranolol versus Mirtazapine versus placebo, shows mirtazapine as more effective in treating akathisia
- Poyurovsky, M., Pashinian, A., Weizman, R., Fuchs, C., & Weizman, A. (2006). Low-dose mirtazapine: a new option in the treatment of antipsychotic-induced akathisia. A randomized, double-blind, placebo-and propranolol-controlled trial. Biological psychiatry, 59(11), 1071-1077.
- Mirtazapine at 15 mg at bedtime was effective in 43% of patients
- Placebo was effective in 7% of patients
- Akathisia may present as side effect in SSRIs and antiemetics (compazine)
- Expected or Therapeutic plasma concentration ranges for antipsychotics and mood stabilizers
- DSH Psychotropic Medication Policy (see resource page)
- Aripiprazole (Abilify)
- 3rd generation antipsychotics, partial dopamine agonist
- Has high affinity for dopamine receptors, higher than 1st and 2nd generation antipsychotics. If Aripiprazole is present at therapeutic concentrations, 1st and 2nd generation will have very little interaction with dopamine receptors.
- Keeps dopamine signaling at about 25% of dopamine’s maximum signal transduction, tends to produce all or nothing response in terms of treating psychotics. Not much ability to vary where dopamine is blocked because of it’s high affinity.
- Side effect profile is very favorable. Largely metabolically neutral, tend not to cause weight gain, glucose intolerance, and lipid abnormalities. Low affinity for alpha receptors or histamine receptors, is not very sedating and does not lower blood pressure.
- Use outside of schizophrenia
- I.e. risperidone and olanzapine also exhibit utility as mood stabilizer and antidepressant.
- 3rd generation antipsychotics also tend to improve mood, driven by quality of the molecules and in part by the desire of pharmaceutical companies to broaden their market
- Use in dissociative state, such as Borderline Personality Disorder
- Antipsychotics can help bring patients out of dissociative state in short period of time
- Borderline patients was found to have a significant limbic dysfunction, hence antipsychotics may be helpful
- Future of Schizophrenia Spectrum Treatment
- There is great need to identify individuals at risk for the disease and treat them with lower dose of antipsychotics. Hopeful data is currently present in support of this approach to lower the incidence and prevalence of schizophrenia.
Tagged: antipsychotics, psychopharmacology, history, schizophrenia, podcasts, podcast, psychiatry podcast for medical students, psychiatry podcast for residents, schizophrenia podcast, trauma podcast
Comments (0)
Newest First Subscribe via e-mail Preview Post Comment… Newer PostHow to Fix Emotional Detachment Older PostHow Psychiatric Medications Work with Dr. Cummings
Powered by Squarespace
‘Suicide is Painless it brings on many changes.’ Posted November 12th 2019

Back in my student days at the University of East Anglia, I had to deliver a seminar paper on Emile Durkheim’s study of ‘Suicide’ and to what extent had he followed his own ‘Rules of Sociological Method’ to deliver it.. Off the top of my head the French sociologist concluded, from his studies, that people committed suicide for reasons that could be cateogorised.
For example, altruistic suicide was committed for the benefit of the group. Captain Oates walking out into the Antarctic night, suffering from serious frostbite, saying he ‘might be some time’ was intended to unburden Scott’s struggling team of ill fated explorers. In our ‘grab what you can’ society that sort of suicide seems increasingly unlikely.
More commonly he concluded that a large number of people committed suicide because they were not integrated into any social group. Transexuals are a high suicide risk because they originate mainly from lower social class groups. Those groups tend to have rigid deferential moral systems and are likely to ostracise those who breach them.
Religion is another profound source of what many use for a moral code. In the Judaic/Christian/Islamic world suicide is a sin leading to eternal damnation. Up until the 1960s in Britain it was a police matter if the person failed in their efforts to die.
Even now the system avoids the truth by labelling suicides as linked to mental health problems, so if the person survives they will end up inside a mental hospital drugged up until such times as they are fit for ‘care in the community’ which is code for life on the street.
There is no room for a Durkheim in modern sociology. This would be science of society is now a mouthpiece for feminism and fake liberalism. It is not interested in struggling to expose key social dynamics. I was involved lecturing and examining sociology students work in the 1980s. I saw the subject hi jacked by the politically correct.
Durkeheim’s most interesting concept, for me, was anomie. For Durkhein, a functionalist sociologist from the nineteenth century, norms held societies together. Norms was short for social normals. A society needed to achieve normative integration to survive. Individuals who did not fit in with the norms was described as anomic. Durkheim concluded that anomie could lead to anomic suicide.
Modern sociology is based on fake Marxism, with women of the world portrayed as the underclass- lumpenproletariat. Women are told what they can be which is ‘anything they want to be. Men are told what they are. This bigotry infests politics and corrupts justice. It also distracts people from the truth or any effort to find it. It is based on the divide and rule tactics that built the British Empire – an ideology that grew to rule the world.
The problem is that, to borrow a phrase from Marx’s Communist Manifesto. ‘the workers of the world’ regardless of gender feel the strain, struggle to survive and fear for their children’s futures. They are not supposed to understand the patronising mumbo jumbo of politicans, psychiatrists and all the rest of the patronising global elite.
So the brainwashing has a flaw. Many people riot, others go mad while more and more commit suicide. Globalisation was only ever meant to help a global elite exploit a global labour force so that they get ever richer. Global media is meant to make money, not show poor people what is going on, the confusion is enough to frighten them.
Mass migration has the tendency to cause anomie as more and more people live like battery hens or on the street. For many intelligent people suicide is the best way to peace. Still the system cannot admit how it is actually indirecly killing these people. Meally mouthed politicians, religious bigotry and hypocrisy will not stem this tide.The film Mad Max was ahead of its time. Robert Cook
Postscript
Britain has one of the lowest numbers of hospital beds in Europe for young people struggling with serious mental health problems, EU-funded research has found.
It is lagging far behind the level of provision in many much poorer countries in eastern Europe, such as Latvia, Estonia and Slovakia, according to a study of care for troubled under-18s across the EU.
Britain has 9.4 specialist inpatient beds per 100,000 young people for those who are suffering from conditions such as anxiety, depression, psychosis, self-harm and suicidal thoughts. That places it 18th in a league table of the 28 EU countries, researchers say.
Germany has the most, at 64 beds per 100,000 young people, and Sweden has the least, at just 1.2 beds. Latvia, Lithuania and Estonia have 39.5, 31.5 and 21 beds per 100,000 under-18s.
Editorial Comment The real questions are 1) Why do so many young people have mental health problems- honestly? 2) Why does anyone think more hospital beds are the answer? 3) Why are so many people of all ages prescribed anti psychotic drugs and how does this help the probelms which the syetm seems reluctant to research and define without prejudice? Denial is a favourite concept and label used by psychiatrits and psychologists who are lackeys to the system.
That system is very corrupt and seriously into denial. That system is sick and might consider the aphorism ‘healer, heal thyself.’ That is putting it politlely I think it more apposite to quote from rebel psychiatrist and discile of R D Laing, psychiatrists and psychologists are whores offering their state sponsor and client anything they want, all things etc.
Robert Cook
The rate of suicides in the United States is growing – what can we do? Posted November 12th 2019

15 May 2019
- Christine Moutier Chief medical officer, American Foundation for Suicide Prevention
- Patrick J. Kennedy Founder, The Kennedy Forum
Predictions for 2030: What if we get things right? Read the series Most Popular Watch this 3D printer make a boat in world record speed, at record size Kristin Houser · Futurism 06 Nov 2019Alibaba hits $23 billion sales in 9 hours for Singles’ Day shoppingJosh Horwitz · Reuters 11 Nov 2019How millennials’ relationship with their phones is changing the economyCarola Jain · Quartz 11 Nov 2019 More on the agenda Forum in focus Toilet transformation: Changing waste management across India Read more about this project Explore context
Mental Health Explore the latest strategic trends, research and analysis
We are living in a time of urgency: suicide is a global, leading cause of death with a staggering loss of 800,000 lives each year.
Suicide cuts across high- and low-income countries, with lower and middle-income countries bearing the largest burden (80% of all suicides) but with it continuing to be a serious problem in high-income countries as well.
In recent years, the World Health Organization (WHO) and the United Nations have adopted actions plans focused on mental health and suicide prevention, and have set goals to reduce the rate of suicide by varying degrees: 10% by 2020 in the case of WHO, and 33% by 2030 in the case of the UN Sustainable Development Goals. Presently, 40 countries have enacted national strategies to prevent suicide, several of which are proving effective, with reductions in suicide rates in many countries such as China, Denmark, England, Switzerland, the Philippines and South Korea. Though the absolute number of suicides globally continues to increase, a recent study accounting for population growth, found the global rate of suicide has dropped by 32.7% over the past 27 years.
In the US, even as attitudes evolve regarding mental health and suicide prevention, the national rate of suicide has risen 33% over the past two decades with a societal price tag of $70 billion annually. Overall mortality, particularly in the middle years, is increasing as a result of the so-called “deaths of despair” due to suicide, alcohol, opioids, and liver disease. Although 94% of American adults believe mental health is equally as important as physical health, most do not know how to identify changes in mental health that signal serious risk, nor what to do in response.

Suicide was declared a public-health crisis in the US as long ago as 1999 by the Surgeon General. Many factors are involved, including human experiences of isolation, struggle, loss and unmet expectations; low mental-health literacy; and a separate and unequal system of care with limited treatment access for those with mental health and substance use disorders.
Although the suicide prevention field is still fairly young, a growing body of suicide prevention research indicates there is reason for hope – and that suicide can indeed be prevented on a general population basis. But to stem the rising tide of what is currently the 10th leading cause of death in the US, the science behind suicide prevention must grow in order to translate into effective solutions we can put into practice and bring to scale in communities throughout the country.
Fighting suicide at local and national level
Firstly, it is critical that we invest in suicide prevention science at a level commensurate with its mortality toll (see figure below).
Suicide is complex, but like most health-related leading causes of death, it has multiple risk factors we know converge to increase mortality. These include: genetic loading, neurophysiological functions in the brain, environmental factors both distant and current, social determinants, biological variants of the stress response on cognition, issues like impulsivity and aggression, and access to lethal means. Fortunately, just as the field of oncology has and continues to answer key questions related to cancer – its causes, prevention and treatment – suicide prevention scientists have reached consensus on scientifically based, population-level solutions in response to these risk factors.
These solutions have been replicated and are quite clear. They include public education on mental health and suicide, community approaches such as addressing access to lethal means during periods of risk, and clinical interventions that effectively target suicide risk.
Implementation of these strategies through local community-based initiatives are at a nascent stage, and a focused national effort through health systems, educational and workplace settings has yet to launch. We must therefore educate policymakers on the specific, effective strategies we know have demonstrated reductions in mortality and increased access to care. On a fundamental level, the Mental Health Parity and Addiction Equity Act of 2008 (Federal Parity Law), which requires insurers to cover treatment for mental health and substance use disorders no more restrictively than treatment for illnesses of the body, such as diabetes and cancer, must be fully enforced to make sure people can get the help they need.

This and other efforts will light a path forward for federal and state policy solutions, in accordance with the growing public demand related to mental health and suicide prevention.
Greater understanding and awareness of mental health and suicide prevention throughout communities are proven to reduce the rates of suicide in those communities. Imagine a society in which a common, basic understanding of neuroplasticity and epigenetics are fact not fiction, and serve to inform a more compassionate, trauma-informed approach to K-12 education and workplace wellness. Prevention for psychiatric illness can start early, suicide prevention can be built into every school and pediatric clinic, and children and adults can be taught strategies that protect and enhance cortical brain development.
Similarly, envision a society in which:
• Front-line citizens (e.g., first responders, teachers, health professionals, legal/financial advisors, probation/corrections officers, addiction counselors) are trained in basic mental health first aid and suicide prevention
• We move beyond the shame sometimes associated with psychological distress, suicide attempts and suicide loss
• Medication-assisted treatment (MAT) is embraced as the gold standard of care for Opioid Use Disorder and is readily available in states across the nation
• Biomarkers for suicide and predictive analytics are further refined and scaled to a national level, giving every patient in primary care the benefit of mental health screening and suicide preventive interventions, as they do for other leading causes of death (cardiovascular, cancer, infectious)
• Health systems have become suicide-safer systems of care
There is reason for hope. New recommended care standards were recently released for better detection and clinical care that reduces suicide risk. At the American Foundation for Suicide Prevention, research funding, community education and support for those who have attempted and/or lost loved ones to suicide serve as catalysts for cultural transformation. In addition, suicide rate reduction is being demonstrated through initiatives like AFSP’s Project 2025, which has the bold goal of reducing the annual rate of suicide in the US by 20% by the year 2025, using a dynamic systems-model approach to determine evidence-informed actions to take to achieve that goal.
The seeds of change are glimmering around the globe, and a hopeful foundation is being built upon an expanding awareness of this public health issue. New resources like WHO’s toolkit for engaging communities in suicide prevention are being launched. Stigma-reducing education like Mental Health First Aid is being taught around the world, from India to Ireland. In the US, the nation’s readiness for effective pro-mental health and suicide prevention strategies is growing like never before, and the scientific field of suicide has matured enough to provide answers on what we as a nation, and in communities throughout the country, can do to lower the rate of suicide throughout the country. We don’t have time to waste. We must all work together with partners of many types across sectors – health systems, business, labor, agriculture, law enforcement, media, education and policy – to mount an effective suicide prevention plan that is necessary to stem this rising tide.
Suicide prevention is a complex challenge, but we remain resolute. Let’s speed the scale-up of effective solutions and work together to reduce the suicide rate across nations, and further spread the sense of hope necessary to save lives.
5 ways communities can prevent suicides
• Host educational trainings such as Mental Health First Aid and Talk Saves Lives™ for frontline citizens and healthcare professionals.
• Invite local AFSP chapter to provide suicide prevention education and education on lethal means, especially among communities with higher gun ownership.
• Provide local media with guidance on safe reporting strategies, and hold them accountable for promoting messages of hope, help-seeking and resilience.
• Integrate mental health care and suicide prevention practices into primary care, and bring Safety Planning and SafeSide Primary Care Training to local health systems.
• Spread awareness of local mental health providers that specialize in treatment modalities that reduce suicide risk (especially in high risk individuals): cognitive behavioral therapy for suicidal people (CBT-SP), dialectical behavior therapy (DBT) for adults and adolescents with elevated suicide risk, attachment-based family therapy (ABFT), and collaborative assessment and management of suicidality (CAMS).
Why are so many men losing their sex drive? Men are now more likely to refuse sex than women – and doctors blame everything from the recession to toxins Posted November 7th 2019
By Clare Goldwin for the Daily Mail
Published: 23:43, 3 April 2013 | Updated: 23:43, 3 April 2013
Throughout their married life, Paul and Susan Bearley had always enjoyed a fulfilling physical relationship.
Even after 35 years and three children together, they were still making love several times a week. So when Paul, a PE teacher, suddenly lost interest in having sex, Susan feared he was having an affair.
‘If I made an advance, Paul would say things like “I’m not in the mood”,’ says Susan, now 57, from Sutton Coldfield in the West Midlands. ‘I’d think: “Is there something wrong with me? Is he going off with somebody else?”
‘We’d always said if we met someone else we’d be upfront. I was preparing myself for him telling me he’d met another woman.’
It was only when Susan, a site manager for a school, found Paul, now 59, in their bedroom in floods of tears that she realised something altogether different was going on.

Throughout their married life, Paul and Susan Bearley had always enjoyed a fulfilling physical relationship
‘By this point, the symptoms had been going on for a few months,’ she says. ‘He said he couldn’t understand what was wrong with him. Not only had he lost his sex drive, but he was exhausted all the time, had put on a lot of weight and was suffering from extreme mood swings.’
Susan forced her husband to see his GP, who ordered a blood test to check Paul’s testosterone levels.
Paul says: ‘My testosterone levels were almost non-existent, which the doctors think was a result of a bad bout of flu I’d had that had knocked out my ability to produce it.
He was prescribed three-monthly testosterone injections, which he now has to have for life.
It was after the second jab that Paul noticed his sex drive returning and his other symptoms disappearing. ‘It was an amazing feeling when my libido came back,’ he says.
Now, four years after his problems began, Susan says she and Paul make love up to five times a week.

‘It’s definitely difficult for a man to admit he is having problems in the bedroom’
She adds: ‘For months it felt like I’d lost my husband, but six months after starting the injections he was a new man. It was like having the Paul I first met back again.’
Paul adds: ‘It’s definitely difficult for a man to admit he is having problems in the bedroom. I’m so glad it could be sorted – those months were the worst period of our marriage.’
Paul might have felt alone, but he’s certainly not. There’s evidence that more and more men are suffering from a low libido.
The common perception is that men constantly think about sex and are always ready to make love. But a recent survey for online pharmacy ukmedix.com found 62 per cent of men turn down sex more frequently than their female partner, with a third admitting they had lost their sex drive.
Another poll revealed one in four men is no longer having sexual intercourse at all – and the figure rises to 42 per cent for men over 55 – while a quarter said they had been affected by erectile dysfunction at some point in their lives. Dr David Edwards, a GP specialising in sexual issues, says the impact of low libido on a man and his relationship can be devastating.
He says: ‘Sexual problems are the most common cause of men crying in my surgery. I saw a man recently and his low libido had destroyed his previous relationship. He’d suffered with it for 12 years, and only came to me because his current partner said she would leave unless he sought help.’
Lucy Bowden and Stuart Brown certainly know how a low libido can push a couple to the edge.
After seven months living together, they’d begun having blazing rows about trivial things such as who’d failed to buy teabags.
Both knew the real problem was much more sensitive – Stuart had virtually stopped wanting to make love. They got to the point where Lucy was reluctant even to give Stuart a cuddle in case she faced yet another rejection.
Not tonight
A sexless marriage is defined as one where a couple have sex fewer than ten times per year
‘When we first got together, our sex drives were fairly equal,’ says Lucy, a 36-year-old corporate fundraiser who has been with Stuart, 40, for two years.
‘Then, suddenly, everything changed. We went from having sex several times a week to once every two or three weeks, then less.
‘As much as you try not to, you can’t help thinking “he’s fallen out of love with me”. When sex did happen, I felt under pressure to make it brilliant. If it wasn’t happening, I’d feel even worse. It became stressful, instead of a pleasure.’
Like most men, Stuart found it acutely embarrassing to admit that his sex drive was waning.
He says: ‘Lucy would try to initiate love-making and I’d make an excuse and say I didn’t feel like it, or that I was too tired. I’m an engineer in the building trade, and there are lots of guys who boast about what they’ve done and how often. I didn’t even feel like having sex, and that made me feel low, that it was me being “weird”.
‘But after a few months it got to the point where I had to tell Lucy that it wasn’t a problem with her but with me, and thankfully she was very supportive.’

‘When we first got together, our sex drives were fairly equal,’ says Lucy, who has been with Stuart for 2 years
low libido can have psychological or physical causes, and sometimes a combination of the two.
Illnesses such as diabetes (50 per cent of men with Type 2 diabetes are testosterone deficient), a pituitary tumour called an adenoma, Klinefelter’s (a genetic syndrome affecting one in 500 men) and chronic conditions such as renal problems and cystic fibrosis can all affect testosterone levels.
Some medications also dampen libido, such as anti-depressants and beta blockers, which are used to treat anxiety and high blood pressure. As Paul discovered, it can also be a result of illnesses such as flu or glandular fever.
But the way we now live is also playing a part. Rising obesity levels are pushing up the number of men affected by low libido.
Dr Edwards explains: ‘If you have a big fat belly the testosterone gets bound to the fat, and that will lower levels of it.’ Testosterone levels also decline naturally over the years – sometimes called the andropause or ‘manopause’. Some doctors feel this is happening at an earlier age.
Dr Malcolm Carruthers, founder of the Centre for Men’s Health, has been treating men with libido problems for 25 years.

‘After a few months it got to the point where I had to tell Lucy that it wasn’t a problem with her but with me’
He says: ‘I do believe testosterone deficiency is becoming more common and happening younger.
‘It used to be mostly men in their 50s, but it’s now men in their 40s, or even 30s. Large studies done in America show that every decade there’s a decrease in testosterone levels by as much as ten per cent. I believe the same is happening in this country.’
He adds that rising oestrogen levels in the environment – caused by hormones from the contraceptive pill finding their way into the water supply and food chain – may have a counter-effect to testosterone.
Research has also shown a link between exposure in the womb to gender bending chemicals such as bisphenol A and phthalates, (found in some food packaging and other plastics), and lowered testosterone levels. Dr Carruthers also believes the pressures of the dire economic climate are having a detrimental effect on men’s libidos.
‘Stress can cause a decrease in testosterone production, and an increase in stress hormones such as cortisol and adrenalin, which causes resistance to testosterone.’
A quarter of people surveyed for Good Housekeeping magazine last year said they were making love less often than they were 12 months earlier, with men blaming their lack of libido on money worries.
Financial stress and lowered libido are things Neil Shah, 38, from West London, knows all about. Ten years ago he was the MD of a failing recruitment company employing 30 people. ‘For about a year I was struggling to keep the company going and I was under immense stress,’ he explains.
‘I wasn’t sleeping or eating, and I completely lost my libido. I’d recently got married, and though my wife and I had always had a good physical relationship, that side of things just disappeared.
‘My lack of libido contributed to us splitting up, and though we did get back together again, we eventually divorced.’
After Neil, now single, was forced to put his company into liquidation, he went travelling to try to recover from his broken marriage and failed business.
The break helped him realise the impact that stress had had on him, and inspired him to set up the Stress Management Society, a not-for-profit organisation offering support for those affected.
He says he’s noticed increasing numbers of men complaining that impaired libido is one of the problems they are facing in these tough economic times.

Financial stress and lowered libido are things Neil Shah, 38, from West London, knows all about
He says: ‘There’s a clear link between stress and low libido. When a person is under severe stress they go into survival mode. Oxygen is diverted to the heart and lungs, and away from the sexual organs. Reproduction is the last thing the body wants to engage in.’
He adds that lack of sleep also contributes to libido problems – a fact confirmed by a University of Chicago study which revealed that men who sleep for fewer than five hours a night for periods of more than a week have the testosterone levels of someone 15 years older.
So what can be done about a low libido?
Dr Edwards says wives and partners are vital in turning the situation around because without their support, men are unlikely to seek professional help.
‘Only a third of men with erectile problems come forward for help. To admit that your sex drive is waning isn’t a macho thing to do, so women have a vital role in getting their partners to seek help.’
Dr Edwards adds that low libido should always be investigated, and testosterone levels checked, to rule out any underlying medical condition. However, because some men have a higher natural resistance to testosterone than others, diagnosis can be more complex than a simple blood test, and consequently many men go undiagnosed, he says.
‘I believe only one per cent of men who could benefit from testosterone treatment are getting it at the moment. The way to diagnose it is by listening to the patient, their history and symptoms. If symptoms disappear when you give a course of testosterone treatment, that’s the answer as far as I’m concerned.’
While men such as Paul need testosterone replacement treatment (whether it’s quarterly injections or a gel rubbed into the skin), others, like Neil, resolve their problems by making lifestyle changes.
Stuart turned to a herbal remedy to help him. When he and Lucy, who live in Brighton, talked the issue over, he realised his waning desire was probably down to recurring bouts of depression triggered by the death of his father 11 years ago.
His GP recommended antidepressants but, knowing they can impair sex drive, he decided five months ago to try KarmaMood, a supplement based on St John’s Wort, a herbal extract believed to lift mood. ‘St John’s Wort has helped with both the depression and my libido,’ he says.
It seems low libido is a problem affecting an increasing number of couples for myriad reasons, but one thing is clear; if a couple can talk about it together, there is hope that it’s a problem they can solve. Why have sex with women like this.
‘Because I’m not wallowing in my own self-pity, I’m more upbeat and more up for sex. We’re having more of it, and I initiate it more often.’
Lucy says: ‘If you want a relationship to work, you have to work at it together and support your partner. I’m so glad I did.’
Edirorial Comment: It is of course worth noting that any issue within a heterosexual relationship is automatically the fault of the male partner. Why admit to needing anything when many women will refuse to offer any meaningful form of psychological support or help to their male partner?
Being a good partner should not require the male to perform sexually whenever the woman demands it. Sex is something that in times of stress or illness will often become a low priority rather than an immediate one. The rising need for viagra for men says it all. Why would chemical aids be so necessary if the feminist narrative of never ending harassment was true?
An unhappy male – whatever the reasons – will be treated with drugs to increase his waning libido to satisfy his female partner’s demands for physical intimacy. However were the two positions to be reversed that type of constant pressure on a woman to perform sexually would be classified as male controlling and abusive behaviour. It would not be treated as a medical condition but rather a crime requiring urgent police intervention.
There remains the popular social myth that ‘men’ will have sex with any women that cross their path. Not every man has an enormous sex drive or is so fragile mentally that they require constant sex to validate their egos.
Why tell the truth when it may well lead to ridicule and separation anyway? I suspect that many less than happy modern men are afraid to tell the truth about their declining libido to their female partners because relationships are now far from being equal in the new age of women – a clear matriarchy.
Charles Close
8 Reasons Why Men Lose Interest That Have Nothing To Do With You Posted November 7th 2019
By Taylor DuVall, August 19th 2016
A quick Google search about why men lose interest comes up with one common answer: it’s your fault, ladies. Some articles blame women for gaining weight, talking too much, or caring too deeply about women’s equality (How dare women eat, talk, and want to be treated like human beings! The horror of it all!)
Reality check: most of the time when guys lose interest in you – most of the time it has nothing to do with what you did right or wrong. You actually don’t have, and arguably shouldn’t have, the power to manipulate somebody else’s interest in you.
Sure, it’s always important to do a self-check and see if you were bringing any real issues to the table. Things like: codependency, a lack of honesty, still being in love with an ex, or too many expectations. But these are reasons for more serious relationship problems, not simply his lack of interest.
The reason why men lose interest often has way more to do with him and his own life than it has to do with how loudly you talked, how early you had sex, or how many times you called.
Here are 8 common reasons why men lose interest. (And none of them, ladies, have anything to do with you.)
1. He is dealing with his own demons.
Society still projects men as these tough superman characters who can’t be bothered with emotional problems. That is a load of crap. All people have demons, hang-ups, and painful experiences from their past that will still affect them in the present.
Though he may not feel comfortable telling you this is what he is doing, men may lose interest in having a relationship when they realize they have a whole bunch of baggage to deal with first.
I know, ladies, many of us think: “but I could help him!” Not every inner-battle can be helped. If you are in a long-term committed relationship or a marriage, he may be grateful working through it all with you. But often, these things cannot and should not be untangled with someone else around– and that’s definitely not your fault.
2. Something in his life has changed.
When a man loses interest in you, something has often changed. But that probably doesn’t mean you did. Think about how many times in your own life a new opportunity, plan, or idea has come forward all of a sudden. This can happen to your guy too.
Maybe he’s decided he wants to travel for a while. Maybe he has a new job opportunity that will either take him away or take up too much time. These life events happen and they don’t always work with someone else in tow.
This will have nothing to do with you. We are all on our own life paths and sometimes our paths join together beautifully, and sometimes there’s a fork in the road. You cannot predict these life changes each time you meet someone new. He probably didn’t either.
3. He has changed his mind.
Sometimes something in his life changes, but sometimes he is the one who changes. It is possible to want one thing and then realize it’s not all you hoped for. All the things he wanted when he met you could be different now. He simply changed his mind.
He could have thought marriage and family life would be ideal. But as he gets closer to tying the knot, he realizes that’s not the actually case. He could have thought he wanted a relationship to look a certain way, but it turns out he actually prefers something else entirely.
You will have to get out from the trap of thinking if you behaved differently, he wouldn’t have changed his mind. Remember, we are not in charge of other people’s thoughts and actions. We are really only witnesses to them.
4. He is not ready to commit to a relationship.
So many women feel it is their seductive powers that cause men to full under a spell of lifelong commitment. Then it means if he doesn’t commit, women take it personally, “What did I do wrong? It must be me.”
If a guy isn’t ready to commit, he’s not going to commit to anyone. Commitment is a personal choice that we cannot (and should not) force or make for another person. If he isn’t committing to you, that’s his 100% choice. And it’s not always for selfish reasons. He may simply be aware of the goals and experiences he wants to gain first– or he knows deep down that you want different things.
Maybe he thought he was ready, but actually wasn’t. Maybe he was stringing you along. Maybe he was honest about not wanting commitment, but you thought you could change him (you can’t, by the way). In fact, you are not the problem. Most of the time, he isn’t even the problem. He is just not ready.
5. He likes the chase more than the woman.
It is true that some men are bigger fans of the chase than any woman they are chasing after. If the act of pursuit is what turns him on, there is nothing you can do (or nothing you shouldn’t be doing) that can change that.
When a man loses interest because he has “won the prize” of having you, you cannot convince yourself that you did something wrong like having sex too quickly or introducing him to your family before the right time.
He wanted a chase. He wanted to win. He didn’t necessarily want a particular woman. In a sad way, you are interchangeable to a guy like this. That stings, but it should assure you that you had nothing to do with is lack of interest. Find a man who is more interested in you and the relationship itself.
6. He is in love with somebody else.
When a man falls in love with another woman, what do we often say? “His wife must not be having enough sex. His girlfriend must be too demanding. She’s so clingy, no wonder he strayed.” We blame the cheated woman.
If he is in love with another woman, that does not mean you are inadequate, ugly, uncaring, or unsexy. It means he fell in love with another person. He did. It’s his responsibility. Whether you’ve been dating a few months or married for decades, your man falling in love with someone else is not a reflection of your flaws. It is a sign of something going on within his own heart and mind.
He could also have lost interest because he is still in love with someone from his past. You are not responsible for using your magic powers to break that bond of love. That is something he will have to deal with on his own.
7. He is an asshole.
“Asshole” is definitely an option. This is the guy who isn’t interested the second you gain two pounds, the guy who can never be found when you need something. He’s the guy who only wants to be served, or the guy who simply was never interested to begin with.
These are assholes and they lose interest for all sorts of shallow, sexist, and lame reasons all the time. They are the ones who will blame everything on you and have a whole string of women who they “lost interest in.”
Assholes will probably tell you it is your entire fault, but that couldn’t be further from the truth. There is no pleasing an asshole. So let your bruises heal up and find a man who cares about more than himself.
8. He may have no reason at all.
Sometimes something just does not feel right. He may look at you and know everything is wonderful. He’s attracted to you. He loves the light you bring into his life. Everything is perfect on paper. But he is just missing a certain spark.
Chances are, he probably cannot even communicate or understand why he’s lost interest or why something doesn’t feel right. That’s the crazy thing about love: it’s unpredictable.
There may not be a reason why a man loses interest in your relationship. It may just happen for him. Sure, when he doesn’t offer you a reason, it may feel like a much harder thing to get over. But realize his being unsure is still a valid emotion.
No matter the reason, when a man you’re interested loses interest in you, feelings will be bruised. Hearts will be broken. But it’s important to remember that there are many reasons why men lose interest that have nothing to do with you. It’s on him.
Sometimes the clichéd line, “It’s not you; it’s me” – is entirely true. It’s not you. It’s him. And no matter what he says, don’t own his lack of interest and turn it into something bad about you.
Sex Post Freud Part Two Posted November 15th 2019


Sigmund Freud was born in Moravia, part of the Austrain Empire in 1856, the year of the Crimean War. He died in September 1939, just before the start of World War Two. Much had changed during that period. Others had taken on board his ideas of psychoanalysis and two world wars had impacted on ideas of sexual freedom, and religion- particularly in relation to women.
The 1960s were ostensibly the years of sexual revolution. They were, but not with the peace and love outcome so popularly advertised at the time. This was the age of bra burning, equal pay and female rights without responsibilty campaigns. Social Class inqualities remained untouched.
So Freud was stood on his head. Everything was the man’s fault. history has been rewritten. Working class men are portrayed as inherently rapists and racists. Curiously those two R words differ in only one third letter, P and C. PC is for political correctness and police constable, key elements in our modern society.
So came Germaine Greer and the likes of post feminist Emma Watson with ‘Me Too.’ Suddenly all men had been and were sex offenders. Every woman who made an allegation was automatically telling the truth.
On the one hand all men were in need of sex therapy and viagra, on the other hand they were lurking in the pubs, clubs, alleyways and workplace to take advantage of all the shy retiring highly intelligent ravishing beauties across our nation and the western world.

It is no wonder that record numbers of young men are losing their libido, opting for sex change or committing suicide. Woman can make rape and assault allegations as many years after the event as they like. Target driven corrupt police will then name the accused calling for more women to come forward with allegations.
With enough allegations on record, the unscrupulous and corrupt Crown Prosecution Service ( CPS ) will present this to a gullible jury certain of getting a conviction.
According to material I read on Aylesbury Police station wall, a woman has the right to say no to sex at any time during the act. If the man does not stop he can be accused of rape at any time, regardless of years or evidence after the event. I think modern laws are a bit of a passion killer. Robert Cook
Sex Post Freud Part One Posted November 5th 2019

Sexual freedom is like the property owning democracy. It is a little box to put you in. You think you own it, especially if you are female. If you are female you can kick your man out of the box and get another man in to pay the mortgage. You won’t know the truth; that only the elite own stuff and that includes you. Property owning is a myth for most, enslavery in fact. Sex is a drug, an opium for self delusion like all other drugs.
Sigmund Freud tried to break people free of the sex box, though analysis was for the wealthy and not stigmatised. The lunatic asylum was for anyone else at the turn of the 19th century and little has changed beyond the euphemism of ‘care in the community’ because the elite do not care- a lot of them still go to private shrinks.
Freud’s ideas shocked the self righteous good people of his home city all so religious Vienna. That was because he stated the obvious, that the sexual libido was the driving force of human behaviour. For centuries the myth of a God created in human image, was the offical truth, excuse for wars and reason for life.
Our elites are reviving that nonsense in the name of diversity and tolerance. Ironically these people are the most intolerant which is why they pass laws to prevent criticism. It is why the British elite won’t let the masses actually leave police state Europe.
Cameron’s idea was to get a mass vote of confidence in his ‘once in a lifetime’ vote. His experts in mass psychology told him he would because they assumed they knew how stupid and afraid the voters are.
That was by the way. Back to my theme of sex. The real reason for life is sexual reproduction. It is a primary drive, informing the development of the human psyche.
Freud outraged polite society by arguing that humans were sexually aware by age four and that posh women liked sex. Frustrating the sex drive, denying it even was behind the mental problems of the upper class females who came to him for the fashionable and new psychoanalysis. Upper class men coped by seducing or forcing the underclass of women, especially servants and prostitutes, into the animal sex they craved but could not admit to.
In those day posh women were dressed up in lashings and layers of fancy clothing, bustling about, absurdly long hair, faces disguised by make up, natural odours masked by perfume. To suggest that there was anything sexual under the clothing, let alone a secret place of appetite was outrageous to the fake Christians.
The clothes were worn to protect women’s virtue, hiding the truth of sex. Not surprisingly the clothes themselves became a fetish for frustrated repressed men, hence the popularity of naughty books called bodice rippers.
Two World Wars put the masses in the front line. Butchery and bloodshed revealed what people were made of and how young they could die. Naturally, sexual appetites increased to make up for lost population. Life was not about girls being sugar and spice and all things nice, or boys being made of slugs and snails and puppy dogs tails.
So a new and better world was promised to the survivors of World War Two and their offspring. I grew up in the 1950s and know what real austerity was like. Today austerity is about overpaid incompetent public servants complaining that their pay rises are too low- that is another story.
So by the mid 1960s in Britain the fake sexual liberation began- along with a whole new range of mental health problems. The 1960s were ‘swinging’ the media told us. The more worrying undertones from a minority of pop groups like ‘The Kinks’ were not what mattered to love struck young females in their ever shorter skirts, on the pill and calling for abortion on demand. This was the age of free love. On the face of it Freud had been accepted at last.

The little picture frame was made by Robert and shows a picture of his dad and the dog, ‘Prince.’ The elite have always looked down on the underclass. They have an army of bureucrats to keep the population down, and to distract them. Sexual hypocrisy is a major part of their mind and skill set. RJC
TO BE CONTINUED ON TO THE AGE OF MALE SEX OFFNDERS, ME TOO AND AN EXPLOSION OF SEX OFFENCES.
Tavistock Institute: Building Absolute Mind Control for the New World Order Posted October 30th 2019
RobertsCourt.com

Eugenics is highly active in America as an unconscious political power source, but has been made invisible to your rational mind. This intellectual blindness has been programmed. The only way to understand eugenics as a sophisticated “crowd control” device is to view the big picture. The big picture tells us that powerful Mind Control is all around us and even runs through us. This is no passive development. Like usury, eugenics is a major “crowd control” and Mind Control device employed by the elite against the non-elite which has been deliberately made invisible via your own belief system. It’s top-down programming has been manipulated secretly. By “depatterning” our minds, beginning in childhood, Tavistock and their Tory American allies serve a broader agenda of psychological warfare against the democratic mind.
“We are your overlords.”—Led Zeppelin
To weaken the moral fiber of the nation and to demoralize workers in the labor class by creating mass unemployment, demoralization can be advanced as a science. It can even be made utterly irresistible, sexy and hip. As jobs dwindle due to the post industrial zero growth policies introduced by the Club of Rome, the report envisages demoralized and discouraged workers resorting to alcohol and drugs, simultaneously seeking more and more top-down government. Top-down reversals of individual-rights-based social contracts, like the U.S. Constitution, require the destruction of parental authority then replacing the parent with programmed bureaucrats. Through crisis, this can produce a cascading effect toward mass programming, effectively reversing the Constitution.
Psychology a Girl Thing

Looking at this month’s Psychologies I come to the conclusion that it is just another feminist driven insidious publication. Regardless of gender, it is absurd to expect everyone to enjoy their work. In Britain and so many other countries, most jobs are hard, boring, with long hours and short on pay.
But hang on a minute, this magazine is aimed at the kind of women who complain that they only get a million pounds a year from the low order BBC propogandist TV licence payers while their eqially elite pampered patronising male counterparts get two million. Or maybe they are lawyers working for the CPS, out to get convictions regardless of how much defence evidence the police are witholding. Some people enjoy that sort of thing.


Men, especially daughter loving fathers, need to understand that women are not all part of an innocent vulnerable blob. Most average women may lack the muscle power of an average man, but there is more to wielding power than muscle and women have the law on their side, using clothes. looks and sexual power. I heard women talking on BBC Radio Four about the dangers of research into growing babies outside the womb. ‘Not a good’ idea said one educated lady. ‘We would lose our power if that happened.’
The Right to Die October 17th 2019
The very idea of personality disorder as decided by state authorities suggests that there is a prescription for a personality order- on other words, social engineering to make people fit through drugs and/or hospital conditioning. The key questions are who decides this, how and why?

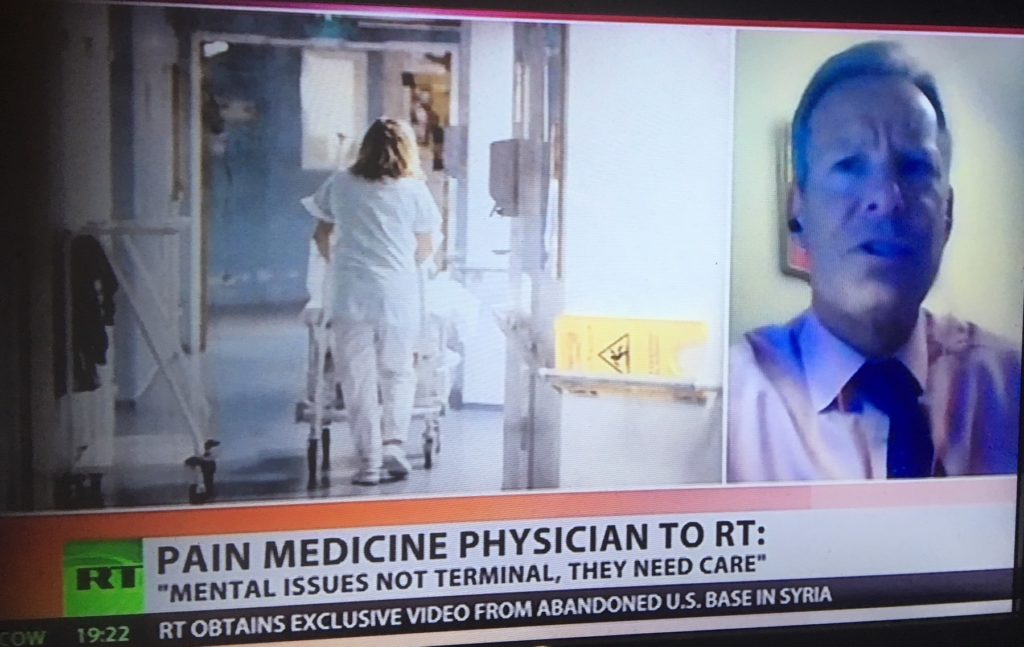
This poor girl has been looking for help for the last two years. Ordinary impressionable men and women of the Western world are being driven mad by elite propoganda, and very nasty doctors, about diversity and non binary is good nonsense. For most people nature is binary.
Normal Women want husbands and children without being policed by morons in blue uniforms, feminists, and so called health experts- Psychiatrists are whores as R,D Laing said they were. They prop up our hypocritical excuse for a society / democacy.. These dreadful patronising people are medicalisisng peoples’ unhappiness.
As for the God squad, they should keep their bigotry to themselves. I and many others, claim the right not to worship this 3000 year old political bull-hit. Society has driven this girl mad, labelled her, making her life even more intolerable. God doesn’t care what happens to this girl, nor does society. So she should get what she wants, not life in ‘the cuckoos nest’. Robert Cook
Fitting Up The Misfits October 18th 2019
The article above about the 23 year old girl who wants to die, was first published on our editorial page. Paranoid Persoanality Disorder appears to be a catch all dignosis for any one who does not fit into our allegedly diverse, police and feminist dominated culture.
It is a subject very close to my heart because of my long standing disagreement with my ex wife and her family regarding my youngest son Edward, who I have not seen for nearly 12 years. These people, mindful of a family member who spent his entire adult life in a mental hospital, where he died, decided that my son was in some way retarded.
The family, who I will not name at the moment for legal reasons are much more powerful than myself. Apart from my eldest son, I have no family and grew up in extreme poverty. Class is the key factor in life chances, not gender or ethnicity.
My son son Edward had enormous problems with being bullied at school. This was a misery I knew from my own school days and witnessed as a teacher. Reluctantly my ex wife allowed me to teach Edward at home for two years before forcing him to go to private school where he was bullied. He developed OCD. I got outside help which my wife cancelled, insisting I was the one with the problem. She ordered me to see an analyst at £40 an hour in 2006.
Previously Edward wrote me pleading letters to be let off school and prepared a contract for each of his parents to sign, saying we would help him kill himself if he had to go back to school. I have the copy my ex wife signed. I did not sign it. I was very alarmed, verbally abused by my wife and hit several times.I nearly succeeded in hanging myself in March 2007 because my life was intolerable. My oldest son’s life was also being harmed.
My ex wife, who admitted to police that she hit me on at least four occasions that she could remember, ridiculed and over rode my protests with her family’s support. The police did nothing about it.
Edward spent the last three years of his life at my home, laying on his bed in his underpants with a playstation, cling wrapped sandwiches, wipes and a bottle to pee in. In 2003, six years before our divorce, I was told by my ex wife that Icould not have any contact with either of my sons unless she was present. If I dd not obey then I would lose my family.
She was still taking Edward, then aged 20, to the toilet and washing him up until the day she left -taking him with her, telling his older brother and me that we could never see him again.
The noises coming from the bathroom while she was washing him were most alarming. The police told me that this would only have been of interest them if it had been me taking a 20 year old daughter to the bathroom. I have been threatened with prosecution and prison for raising this issue with them.
My ex wife’s brother – whose wife is also a police officer backing her husband’s allegations against me – was ( and may still be ) a senior police officer. Edward was sent to his remote rural home after my wife and I split up.
My ex brother in law damingly lied that my oldest son and I were stalking and threatening his family on the weekend of October 4th/5th 2008. Without any investigation, by my ex brother in law’s police force or my locla one in which he served as a Divisional Commnder. I know what the motives were.
My ex brother in law’s home was 158 miles away and we were 15 miles north of Liverpool with a friend at the time he alleged we were stalking and threatening violence to his family, including his children.
Thi senior police officer also lied that a police sergeant ( it is [possible the sergeant and his partner lied to curry favour ) found us nearby. The ex brother in law’s family also lied and the police have lied ever since that my son and I were threatening them with violence. I was arrested after confronting the police with evidence in support of my allegations in 2015.
The force in question put a PNC Criminal Marker on my car on October 9th 2008 and created soft intelligence records that ruined mine and my eldest son’s career and lives= leading to violence from locals. To this day the police will not explain the marker because they know it was illegal involving high level abuse of power , conspiracy and misconduct in public office..
PNC Criminal Markers are given for sex, violence, drugs and arms suspects. My car was chased, sometimes dangerously, and searched many times, hence I was desparate to find out why. I found out in May 2009, but not from the police forces in question. Suspects with PNC markers are liable to being shot by police.
There is much more to this saga and I am taking a great risk to my freedom by telling this much, as I have been in court and locked in cold cells for 12 hours at a time, my house ransacked, police lying to my lawyers , the CPS and threatening me with a long prison sentence too many times because of it. It has been truly terrifying and harmful to my health.
Malicious allegations of domestic violence, never explained to me or investigated, were made during six hearings in 2016- but my ex wife had never mentioned them during the divorce- because she would have to be faced with the evidence and my challenge.
After two failed prosecutions, the police have made several attempts to have me sectioned, with the local GPs, Dr Rodger Dickson’s support. British representative democracy is wonderful as long as you know who it is designed to represent.
Robert Cook October 18th 2019

We had rented a bungalow at £1000 a week for two weeks. Of course my in laws were in the area. They had moved up country but were always back when we were in town.
lIt took a great deal of argument to get my wife’s agreement to get Edward out of the
bungalow to fly this plane around the Penwith Peninsula. I took the photo and Edward was elated having proved he could do something so skillful.
But he was soon taken back to his bedroom, only coming out to continue washing the skin off his hands. I have little time for psycholgists and psychiatrists their labels and pills. I came across R D Laing during post graduate psychology at London University . Edward is pictured left. Image RJC
How is paranoid personality disorder diagnosed?
If a person has symptoms, the doctor will begin an evaluation by performing a complete medical history and physical examination. Although there are no laboratory tests to specifically diagnose personality disorders, the doctor might use various diagnostic tests to rule out physical illness as the cause of the symptoms. For example, difficulty hearing or long-lasting substance abuse may be confused with PPD.
If the doctor finds no physical reason for the symptoms, he or she might refer the person to a psychiatrist or psychologist, health care professionals who are specially trained to diagnose and treat mental illnesses. PPD is different from psychotic disorders such as schizophrenia, paranoid type or delusional disorder, persecutory type, in that the person with PPD lacks the perceptual distortions (for example, hearing voices) or bizarre delusional thinking (for example, being followed everywhere by the FBI). Psychiatrists and psychologists use specially designed interview and assessment tools to evaluate a person for a personality disorder. Source clevelandclinic.org
Editorial Comment
The crucial question, apart from being able to drive a coach and horses through this pseudo mental illnes ( designed to miss the reality of the ‘patient’s life and current circumstances ) is who in the medical profession has enough arrogance to think they can diagnose this condition, let alone define it?. A related question is, who asked for the diagnosis and why?
When I was growing up in Winslow of the 1950s, there was a mental hospital containing lots of old women who had been incarcerated there in the 1920s because they offended hypocritical God fearing society by having babies out of wedlock- some obviously raped by powerful employers in the country houses where they worked as skivvies. On such case is mentioned in ‘The Book of Winslow’ by Robert Cook ( 1989 )
Robert Cook

Some have suggested that Tony Blair fits the bill and should face justice for the sort of war crimes and lies that Julian Assange faces a lifetime in jail for exposing, along with Chelsea Manning.
I last saw Blair at the London Coliseum, after seeing ‘La Boheme’. More than his ‘tiny hand ‘ looked frozen! . Miserable looking pair him and Cherie. Robert Cook


The Psychology of Hate Posted September 24th 2019
Recently, several members of a group calling itself “Respect the Flag” were sentenced to prison for terrorizing guests at the birthday party of an 8-year-old African-American girl in Georgia. Pointing a shotgun, they yelled racial slurs and death threats at guests, including children.
It wasn’t an isolated incident. According to a recent study, there are at least 917 organized hate groups in the United States. The study, based on data collected by the Southern Poverty Law Center (SPLC) and presented in their annual census of hate groups, looked at the presence of hate groups on Twitter. SPLC found that the number of likes and comments on hate group accounts grew by 900 percent in the last two years.
Why do we hate? The reasons are complex, but following are some of the factors that may play a role in helping us understand hate and, hopefully, work toward change.
Fear of “The Other”
According to A.J. Marsden, assistant professor of psychology and human services at Beacon College in Leesburg, Florida, one reason we hate is because we fear things that are different from us.
Behavioral researcher Patrick Wanis, cites the in-group out-group theory, which posits that when we feel threatened by perceived outsiders, we instinctively turn toward our in-group—those with whom we identify—as a survival mechanism. Wanis explains, “Hatred is driven by two key emotions of love and aggression: One love for the in-group—the group that is favored; and two, aggression for the out-group—the group that has been deemed as being different, dangerous, and a threat to the in-group.”
Fear of Ourselves
According to Washington, D.C., clinical psychologist Dana Harron, the things people hate about others are the things that they fear within themselves. She suggests thinking about the targeted group or person as a movie screen onto which we project unwanted parts of the self. The idea is, “I’m not terrible; you are.”
This phenomenon is known as projection, a term coined by Freud to describe our tendency to reject what we don’t like about ourselves. Psychologist Brad Reedy further describes projection as our need to be good, which causes us to project “badness” outward and attack it:
“We developed this method to survive, for any ‘badness’ in us put us at risk for being rejected and alone. So we repressed the things that we thought were bad (what others told us or suggested to us that was unlovable and morally reprehensible) — and we employ hate and judgment towards others. We think that is how one rids oneself of undesirable traits, but this method only perpetuates repression which leads to many mental health issues.
Lack of Self-compassion
The antidote to hate is compassion — for others as well as ourselves. Self-compassion means that we accept the whole self. “If we find part of ourselves unacceptable, we tend to attack others in order to defend against the threat,” says Reedy. “If we are okay with ourselves, we see others’ behaviors as ‘about them’ and can respond with compassion. If I kept hate in my heart for [another], I would have to hate myself as well. It is only when we learn to hold ourselves with compassion that we may be able to demonstrate it toward others.”article continues after advertisement
It fills a void
Psychologist Bernard Golden, author of Overcoming Destructive Anger: Strategies That Work, believes that when hate involves participation in a group, it may help foster a sense of connection and camaraderie that fills a void in one’s identity. He describes hatred of individuals or groups as a way of distracting oneself from the more challenging and anxiety-provoking task of creating one’s own identity:
“Acts of hate are attempts to distract oneself from feelings such as helplessness, powerlessness, injustice, inadequacy and shame. Hate is grounded in some sense of perceived threat. It is an attitude that can give rise to hostility and aggression toward individuals or groups. Like much of anger, it is a reaction to and distraction from some form of inner pain. The individual consumed by hate may believe that the only way to regain some sense of power over his or her pain is to preemptively strike out at others. In this context, each moment of hate is a temporary reprieve from inner suffering.”
Societal and Cultural Factors
The answer to why we hate, according to Silvia Dutchevici, LCSW, president and founder of the Critical Therapy Center, lies not only in our psychological makeup or family history, but also in our cultural and political history. “We live in a war culture that promotes violence, in which competition is a way of life,” she says. “We fear connecting because it requires us to reveal something about ourselves. We are taught to hate the enemy — meaning anyone different than us — which leaves little room for vulnerability and an exploration of hate through empathic discourse and understanding. In our current society, one is more ready to fight than to resolve conflict. Peace is seldom the option.”article continues after advertisement
What Can We Do?
Hatred has to be learned, Golden says: “We are all born with the capacity for aggression as well as compassion. Which tendencies we embrace requires mindful choice by individuals, families, communities and our culture in general. The key to overcoming hate is education: at home, in schools, and in the community.”
According to Dutchevici, facing the fear of being vulnerable and utterly human is what allows us to connect, to feel, and ultimately, to love. She suggests creating “cracks in the system.” These cracks can be as simple as connecting to your neighbor, talking with a friend, starting a protest, or even going to therapy and connecting with an ‘Other.’ It is through these acts that one can understand hate and love.”
In other words, compassion towards others is the true context that heals.
The SPLC encourages anyone who witnesses a hate crime — including hateful harassment or intimidation — to first report the incident to local authorities, then go to SPLC’s #ReportHate intake page to continue the effort to track hate in the country.
Psych Central Professional
Home » Pro » The Exhausted Woman » The Difference Between Male and Female Narcissists

The Exhausted
Womanwith Christine Hammond, MS, LMHC
Editorial Comment Hate used to be a word popular with soap opera script writers, schoolkids and girls dumping their boyfriends. The famous German philopsopher Goethe said and wrote : ‘You have to be a good hater.’ International English athlete Dick Taylor said : ‘You have to hate to win races.’ When I went before an RAF commission board at RAF Biggin Hill back in the early 1970s, I was asked if I could kill.
A female officer, obviously the board’s psychiatrist was annoyed by my hesitation, cutting in with the comment : ‘Well that’s what it is all about in the end.’ I see her point. How can you kill without emotion, without hate, without believing that the enemy is the bad person and worthy of hate?
A great deal of killing has been orchestrated by the bullies who beccame the ruling elite over the centuries. After Rome went Christian and the barely civilised world spilt between Christian and Islam versions of worship and corrupt rule, each side proclaimed they were right. Love was for God and hate for the enemy.
During the so called ‘Great War’ which was all about greed and empire, millions of young men were slaughtered by their betters while propoganda whipped up hate on both sides. British guns were blessed and returning soldiers in 1918, many crippled or traumatised, were thrown on the scrap heap.
The rich rode out the depression until there was an excuse for more war, hate and patriotic hysteria. The post war hippy period was a flash in the pan, the Western World led by Britain and icons like Germaine Greer morphed into feminism and the apparently endless world of hating men, making them pay and putting them in their place.
Hate has been a useful word enabling us to understand extreme emotions and explore causes. Now it is a label and a crime to control the fall out from a new social order- created, by the ruling elite who have no idea of life at the bottom- called DIVERSITY.
The word fan is short for fanatic. The multi billion pound world of sport relies on fans who are known to get drunk and violent, replacing a sense of lost tribalism and belief with football favours etc. Society’s rulers, including feminists, are very concerned. When they look for causes of hate crimes they are not looking at basic human nature.
They are looking at their new world order design to better design and control the individuals and groups that do not fit the kind of diversity they want. Drugs or prison are their ultimate resort if education and psychotherapy do not fit. Robert Cook September 24th 2019
The Difference Between Male and Female Narcissists Posted September 2019
By Christine Hammond, MS, LMHC
Last updated: 27 Jun 2019~ 2 min read

Too often, narcissism is portrayed as an overly aggressive male disorder. It is not. Females can be narcissistic as well although it might look a bit different from males. Meryl Streep in her role as Miranda Priestly in “The Devil Wears Prada” did an excellent job portraying a narcissistic female boss. Michelle Pfieffer did as well in playing a narcissistic mother in “White Oleander.”
There are several areas that the difference in sexes can be seen. But because this is a disorder, there will be a crossover of similarities. Yet, all of this is consistent with the DSM-V definition of narcissism.
Appearance. Narcissists, in general, believe themselves to be attractive and are usually well groomed to attract attention. While males combine their attractiveness with charm to accomplish a goal, females use it to gain superiority. Most females tend to be obsessed with their appearance sometimes resulting in numerous plastic surgeries.
Seduction. Both male and females narcissists are generally gifted in the art of seduction, but how they seduce is different. Males use their charm to entice a mate. Females use their bodies to allure a mate. This can sometimes be seen in provocative clothing. This is different from a Histrionic Personality Disorder (HPD). HPD’s continually wear inappropriately revealing clothing whereas a narcissist does it selectively for a specific person or to accomplish a goal.
Confidence. Narcissists cover their deep-rooted insecurity with a belief that they are “special.” Males tend to be self-confident, gaining their assurance from within. Females gain their poise from comparing their superiority over others. They feel good about themselves when others are beneath their own standards of excellence.
Money. The love of money is strong for narcissists as they believe money gives them power, control, success, status, and dominance over others. Males are preoccupied with obtaining money at all cost, including stealing it from family members. Females enjoy excessively spending money. Both do their behaviors without any shame or remorse for their actions.
Fidelity. If a narcissist fails to get the attention they believe they deserve, they will seek it from outside a committed relationship. While both can be unfaithful, males tend to be serial adulterers. Females act more like black widow spiders, idealizing their mate to attract and them emasculating them. For the spouse or partner, the more they give, the more the narcissist wants. It becomes insatiable.
Children. Narcissists like to raise baby narcissists. Often they pick a favorite child and focus all of their efforts and attention on that child. The other children are left feeling inadequate, unworthy, and insecure. Males generally view children as a nuisance, frequently complaining that they, not the children, should have all the attention of their spouse or partner. Females view children as an extension of themselves, even when the child is an adult. Everything the child accomplishes is a reflection of their superior parenting.
Competition. Nothing proves supremacy quite like competition for narcissists. They love an opportunity to excel over others at work and at home. While the competitiveness is frequently praised in a job, it is not amongst family. Males treat other males as rivals. This can be seen in brother/brother and parent/child relationships. Females battle with other females for dominance. This is seen in sister/sister and parent/child relationships.
This is not a complete list of differences, rather it is meant to bring awareness as to the many ways narcissism can be portrayed.
Christine Hammond, MS, LMHC
Christine is a Licensed Mental Health Counselor by the State of Florida with over fifteen years of experience in counseling, teaching and ministry.
She works primarily with exhausted women and their families in conflict situations to ensure peaceful resolutions at home and in the workplace. She has blogs, articles, and newsletters designed to assist in meeting your needs.
As author of the award winning book, The Exhausted Woman’s Handbook, Christine is a guest speaker at churches, women’s organizations, and corporations.
You can connect with her at her website Grow with Christine at www.growwithchristine.com.
12 Traits Of A Female Narcissist Posted September 23rd 2019
Share on Facebook Share on Twitter
Just as it is among men, narcissism, a dysfunctional behavior is also common among women.
The following traits provided by experts, victims and survivors of emotional abuse and those who had at a time encountered female narcissists; all give detailed explanation to narcissism among women.19 Traits Of A Female Narcissist
Watch video or continue reading 11 Traits of A Female Narcissist Watch this video on YouTube.
- A female narcissist is good at marketing herself. Being the most charming person in the room, you can’t take that away from her; as she craves for attention.
- A narcissist female lacks common courtesy. She’s convinced that the reason for her existence is to make the world complete, thus, sees no reason to reciprocate empathy to others.
- When in a relationship, a female narcissist disengages, use neglect and abandonment to punish her partner.
- Female narcissist lacks the ability to process shame i.e. has difficulty apologizing when found guilty.
- She is unpredictable in her moods. Due to pride and other traits, a narcissist won’t open up to you what she actually wants.
VIDEO: 5 Successful People With INTJ Personality
- Study shows female narcissists will apologized profusely if backed into a corner i.e capable to regret wrong doings just for short-term, it won’t be long when she returns to narcissistic patterns.
Read: Glaring Difference Between Being a Narcissist and Having High Self-esteem
- She belittles your accomplishments, hopes and dreams.
- A female narcissist is prone to envy. She seeks opportunity to undermine others, though pretends she’s contented with what she’s got.
- She focuses her attention on makeup, and more likely to have plastic surgery.
- She is unreasonably jealous.
- A female narcissist seeks favorable treatment. She believes that she deserve to have every good thing the world has.
- Narcissist enjoys being photographed. She places much priority in getting her best portrait on social media sites.
Read: How Social Media Makes Us Narcissistic [Infographic]
- She believes she’s intellectually superior to peers.
Further readings: Paul Wink: The Three Types of Narcissism in Women. Institute of Personality Assessment and Research. University of Carlifornia at Berkeley. J Res Pers: Behavioral Manifestations of Narcissism in Everyday Life. 2010 Aug 1; 44(4): 478–484. doi: 10.1016/j.jrp.2010.06.001 Philipson, I. (1985), Gender and narcissism, Psychology of Women Quarterley, Vol. 9, pp. 213-228. Rhodewalt, F., Tragakis, M.W. and Finnerty, J. (2001), Narcissism and self-handicapping, Linking self-aggrandizement to behavior, Department of Psychology, University of Utah.
written by Moses Chukwu Published: August 6, 2016 in Personality
7 Signs A Woman Is A Total Narcissist Posted September 23rd 2019
like us on facebook
If you ‘like’ us, we’ll LOVE you!Photo: weheartit

Elizabeth Ayers-CallahanBlogger Self November 22, 2017
Yes, women can be narcissists, too!
Close your eyes and imagine a narcissist. Try to picture what you think a narcissist looks like in your mind. It looks like a man, right? While, yes, there are many men in the world with the narcissistic personality disorder, too often, we associate the qualities of narcissism only with men.
We think of unrelenting ego and a smug sense of self-satisfaction and, for whatever reason, we identify those as male qualities. It’s one of the most common stereotypes about narcissism.
But here’s the thing — narcissism knows no gender boundaries. Women can be narcissists too.
Are men more likely to be narcissists than women? There is some research to back that up. However, that doesn’t mean that women are immune from narcissism.
We all know women who make everything all about THEM, women who flaunt themselves, women who are vain or self-absorbed. Women who definitely fit the classic definition of narcissism, which is “excessive or erotic interest in oneself and one’s physical appearance.”
RELATED: How To Leave A Narcissist
There are many, many female narcissists in the world and, if you want to maintain healthy relationships with the people in your life, you need to stay away from them. Here are 7 signs she’s a narcissist.
1. Every conversation revolves around her.
While it’s fine to talk about yourself occasionally in social settings, a true narcissist will almost exclusively talk about herself OR will constantly be attempting to steer the conversation back to her. Ask yourself, “When was the last time she asked a question about ME?” If the answer is NEVER, that’s a pretty clear sign that she’s very full of herself.
2. She’s constantly canceling plans with you.
Conflicts happen, but one of the big signs she’s a narcissist is when she pathologically refuses to commit to prior engagements. She doesn’t care about the impact on others.
She never even thinks about your ruined evening or your disappointment. All she wants is the freedom to do whatever she wants, whenever she wants, no matter how it impacts the people around her.
3. She goes crazy when you tell her “No.”
This is one of the easiest ways to detect a narcissist. When they ask you do to something, just say “No.” It doesn’t even have to be a hard “No.” You can just delay your response or say, “I’ll get back to you.”
Narcissists HATE those kinds of responses. They don’t like other people exerting influence on their self-centered spheres of existence. If you know a woman who loses her mind when you respond in the negative, she definitely has some narcissistic qualities.
4. She flirts with people she doesn’t like.
Flirting is a fun thing for adults to do, but narcissists use flirting as a tool to get what they want. This is particularly apparent if you know a woman who is constantly trying to use her charm or sexuality on people she’s not romantically interested in.
RELATED: 3 Mind Games ALL Narcissistic Men Play In Relationships
Narcissists think they’re the hottest things on Earth, and that inflated sense of self-image makes them believe that no one could EVER resist them. Thus, they flirt as a form of manipulation because they can’t imagine any man or woman wouldn’t be totally seduced by their feminine wiles.
5. She doesn’t speak highly of the people in her life.
Narcissists see themselves standing on the top of the social pyramid — with everyone else firmly beneath their feet. This attitude can become apparent if you listen to how they talk about others.
Does the woman in your life always refer to other people as “idiots”? Does she call her friends “sluts” or “morons”? Does she always question other people’s intelligence, but never questions her own?
That’s classic narcissist behavior. We all have the occasion to rip on our friends from time to time, but if you know a woman who is always doing that and never showing any signs of empathy or self-deprecation, she’s probably a narcissist.
6. She never accepts blame.
If she’s running late, does she ever apologize or was it always the fault of traffic/your directions/someone else? Narcissists have a real problem with culpability — they don’t like admitting that they’re ever at fault for a mistake or a problem.
Their worldview doesn’t support a reality where they could be wrong, so they always deflect blame and argue that someone else (or a factor beyond anyone’s control) caused the problem. You will rarely, if ever, hear a narcissist say “My bad.”
7. Her phone is full of selfies.
Is it all selfies? There’s nothing wrong with selfies, but if you know a woman who seems to exclusively take selfies, paying all her attention to framing herself perfectly and never thinking to grab a shot of her family, friends, or the world around her, that’s a big narcissist red flag.
Women are just as capable as being narcissists as men are. If you have a woman in your life who never seems to exhibit any empathy and who always wants to make things about HER, she probably has narcissist tendencies and you should consider keeping your distance.
Friendships and relationships are all about give and take, which is something a true narcissist will never, ever understand.
RELATED: 7 Traits That Make You A Prime Target For A Narcissist
Elizabeth Ayers-Callahan is a mom, wife and regular blogger for YourTango. She is obsessed with The Kardashians and basically every season and series of The Real Houswives, though she will only sometimes admit it.
17 Quotes Narcissists Will Love (Almost As Much As Themselves)

Michelle TogliaContributor QuotesRead Later
Causes of PTSD- NHS Source September 23rd 2019
Contents
Post-traumatic stress disorder (PTSD) can develop after a very stressful, frightening or distressing event, or after a prolonged traumatic experience.
Types of events that can lead to PTSD include:
- serious accidents
- physical or sexual assault
- abuse, including childhood or domestic abuse
- exposure to traumatic events at work, including remote exposure
- serious health problems, such as being admitted to intensive care
- childbirth experiences, such as losing a baby
- war and conflict
- torture
PTSD is not usually related to situations that are simply upsetting, such as divorce, job loss or failing exams.
PTSD develops in about 1 in 3 people who experience severe trauma.
It’s not fully understood why some people develop the condition while others do not.
But certain factors appear to make some people more likely to develop PTSD.
Who’s at risk
If you have had depression or anxiety in the past, or you do not receive much support from family or friends, you’re more susceptible to developing PTSD after a traumatic event.
There may also be a genetic factor involved in PTSD. For example, having a parent with a mental health problem is thought to increase your chances of developing the condition.
Why does it develop?
Although it’s not clear exactly why people develop PTSD, a number of possible reasons have been suggested.
Survival mechanism
One suggestion is that the symptoms of PTSD are the result of an instinctive mechanism intended to help you survive further traumatic experiences.
For example, the flashbacks many people with PTSD experience may force you to think about the event in detail so you’re better prepared if it happens again.
The feeling of being “on edge” (hyperarousal) may develop to help you react quickly in another crisis.
But while these responses may be intended to help you survive, they’re actually very unhelpful in reality because you cannot process and move on from the traumatic experience.
High adrenaline levels
Studies have shown that people with PTSD have abnormal levels of stress hormones.
Normally, when in danger, the body produces stress hormones like adrenaline to trigger a reaction in the body.
This reaction, often known as the “fight or flight” reaction, helps to deaden the senses and dull pain.
People with PTSD have been found to continue to produce high amounts of fight or flight hormones even when there’s no danger.
It’s thought this may be responsible for the numbed emotions and hyperarousal experienced by some people with PTSD.
Changes in the brain
In people with PTSD, parts of the brain involved in emotional processing appear different in brain scans.
One part of the brain responsible for memory and emotions is known as the hippocampus.
In people with PTSD, the hippocampus appears smaller in size.
It’s thought that changes in this part of the brain may be related to fear and anxiety, memory problems and flashbacks.
The malfunctioning hippocampus may prevent flashbacks and nightmares being properly processed, so the anxiety they generate does not reduce over time.
Treatment of PTSD results in proper processing of the memories so, over time, the flashbacks and nightmares gradually disappear.
Page last reviewed: 27 September 2018
Next review due: 27 September 2021
Women and Mental Health Posted September 23rd 2019
WOMEN
Women are more likely to have been treated for a mental health problem than men (29% compared to 17%).This could be because, when asked, women are more likely to report symptoms of common mental health problems. (Better Or Worse: A Longitudinal Study Of The Mental Health Of Adults In Great Britain, National Statistics, 2003)
Depression is more common in women than men. 1 in 4 women will require treatment for depression at some time, compared to 1 in 10 men. The reasons for this are unclear, but are thought to be due to both social and biological factors. It has also been suggested that depression in men may have been under diagnosed because they present to their GP with different symptoms, for example a range of physical, stress related symptoms. (National Institute For Clinical Excellence, 2003)
Women are twice as likely to experience anxiety as men. Of people with phobias or OCD, about 60% are female. (The Office for National Statistics Psychiatric Morbidity report, 2001)
MEN
Men are more likely than women to have an alcohol or drug problem. 67% of British people who consume alcohol at ‘hazardous’ levels, and 80% of those dependent on alcohol are male. Almost three quarters of people dependent on cannabis and 69% of those dependent on other illegal drugs are male. (The Office for National Statistics Psychiatric Morbidity report, 2001)
Differences in the extent of mental health problems
Mental health problems affect women and men equally, but some are more common among women. Abuse is often a factor in women’s mental health problems. Treatments need to be sensitive to and reflect gender differences.
Various social factors put women at greater risk of poor mental health than men. However women’s readiness to talk about their feelings and their strong social networks can help protect their mental health.
Women as guardians of family health
It is essential that women look after their mental health although busy lifestyles often make this difficult. Traditionally women have tended to take on the responsibility of looking after the health of members of their family as well as themselves. For instance women may shop for their family and choose what they eat or manage what their family do when they feel unwell. This role makes it particularly important that women understand how the choices we all make in everyday life can affect our mental health.
Women as carers
Carers can be women whether they care for their children, partner, parents, other relatives or friends. Women carers are more likely to suffer from anxiety or depression in the general population. just over half of people who care for a person with a mental health problem are women and the average age of carers is 50 – 64 years.
Social support
Women’s friendships with other women help protect their mental health, providing a source of support, particularly in hard times or at times of loss or change. Mentally healthy women generally talk about their feelings more than men and more often have stronger social networks of friends and family. Good social support can play a part in preventing mental ill health and can help people recover from mental health problems.
Women’s mental health
About 25% of people who die by suicide are women. Again, women’s greater emotional literacy and readiness to talk to others about their feelings and seek help may protect them from suicidal feelings. Being a mother also makes women less likely to take their own life.
Women are particularly exposed to some of the factors that increase the risk of poor mental health because of the role and status that they typically have in society. The traditional roles for women from some ethnic groups living in the UK can increase their exposure to these risks.
The social factors particularly affecting women’s mental health include:
- more women than men are the main carer for their children and they may care for other dependent relatives too intensive caring can affect emotional health, physical health, social activities and finances
- women often juggle multiple roles they may be mothers, partners and carers as well as doing paid work and running a household
- women are over represented in low income, low status jobs often part-time and are more likely to live in poverty than men
- poverty, working mainly in the home on housework and concerns about personal safety can make women particularly isolated
- physical and sexual abuse of girls and women can have a long-term impact on their mental health, especially if no support has been received around past abuses.
- Mental health problems affecting more women than men
Some women find it hard to talk about difficult feelings and ‘internalise’ them, which can lead to problems such as depression and eating disorders. They may express their emotional pain through self-harm, whereas men are more likely to ‘act out’ repressed feelings, and to use violence against others.
Depression
More women than men experience depression. One in four women will require treatment for depression at some time, compared with one in 10 men. The reasons for this are unclear, but are thought to include social factors such as poverty and isolation and biological factors such as the hormonal changes experienced by women. However, some researchers dispute the relatively low depression rate for men.
Post natal depression is believed to affect between eight and 15% of women after they have given birth.
Women’s increased life expectancy means they are more likely than men to outlive their partner and move into residential care. This means they are more at risk of depression associated with psycho-social factors. Older people are often faced with more difficult life events and daily stresses than younger people and this may explain why they have a slightly increased risk of depression. Losses whether bereavement or losses associated with growing old such as loss of independence because of physical illness or disability can trigger depression.
Estimates suggest that 20% of older people living at home have symptoms of depression, rising to 40% for older people living in care homes. The majority of people affected are women. Those over the age of 85 are at particular risk.
Anxiety
Women are twice as likely to experience anxiety disorders as men. About 60% of the people with phobias or obsessive compulsive disorder are women. Phobias affect about 22 in 1,000 women in the UK, compared with 13 in 1,000 men.
Dementia
Two thirds of people with dementia are women. Risk of dementia increases with age, and women have a higher life expectancy than men.
Eating disorders
Eating disorders are more common in women than men, with young women most likely to develop one. 1.9% of women and 0.2% of men experience anorexia in any year. Between 0.5% and 1% of young women experience bulimia at any one time.
Post-traumatic stress disorder (PTSD)
Worldwide, more women are affected by PTSD than men, largely because women are exposed to more sexual violence. The risk of developing PTSD after any traumatic event is 20.4% for women and 8.1% for men.
Paranoid personality disorder Posted September 22nd 2019
From Wikipedia, the free encyclopedia Jump to navigationJump to search Not to be confused with paranoid schizophrenia.
| Paranoid personality disorder | |
|---|---|
| Specialty | Psychiatry, clinical psychology |
Paranoid personality disorder (PPD) is a mental illness characterized by paranoid delusions, and a pervasive, long-standing suspiciousness and generalized mistrust of others. People with this personality disorder may be hypersensitive, easily insulted, and habitually relate to the world by vigilant scanning of the environment for clues or suggestions that may validate their fears or biases. They are eager observers. They think they are in danger and look for signs and threats of that danger, potentially not appreciating other evidence.[1]
They tend to be guarded and suspicious and have quite constricted emotional lives. Their reduced capacity for meaningful emotional involvement and the general pattern of isolated withdrawal often lend a quality of schizoid isolation to their life experience.[2][verification needed] People with PPD may have a tendency to bear grudges, suspiciousness, tendency to interpret others’ actions as hostile, persistent tendency to self-reference, or a tenacious sense of personal right.[3] Patients with this disorder can also have significant comorbidity with other personality disorders (such as schizotypal, schizoid, narcissistic, avoidant and borderline)
Contents
Causes
A genetic contribution to paranoid traits and a possible genetic link between this personality disorder and schizophrenia exist. A large long-term Norwegian twin study found paranoid personality disorder to be modestly heritable and to share a portion of its genetic and environmental risk factors with the other cluster A personality disorders, schizoid and schizotypal.[4]
Psychosocial theories implicate projection of negative internal feelings and parental modeling.[5] Cognitive theorists believe the disorder to be a result of an underlying belief that other people are unfriendly in combination with a lack in self-awareness.[6]
Diagnosis
ICD-10
The World Health Organization‘s ICD-10 lists paranoid personality disorder under (F60.0). It is a requirement of ICD-10 that a diagnosis of any specific personality disorder also satisfies a set of general personality disorder criteria. It is also pointed out that for different cultures it may be necessary to develop specific sets of criteria with regard to social norms, rules and other obligations.[7]
PPD is characterized by at least three of the following symptoms:
- excessive sensitivity to setbacks and rebuffs;
- tendency to bear grudges persistently (i.e. refusal to forgive insults and injuries or slights);
- suspiciousness and a pervasive tendency to distort experience by misconstruing the neutral or friendly actions of others as hostile or contemptuous;
- a combative and tenacious sense of self-righteousness out of keeping with the actual situation;
- recurrent suspicions, without justification, regarding sexual fidelity of spouse or sexual partner;
- tendency to experience excessive self-aggrandizing, manifest in a persistent self-referential attitude;
- preoccupation with unsubstantiated “conspiratorial” explanations of events both immediate to the patient and in the world at large.
Includes: expansive paranoid, fanatic, querulant and sensitive paranoid personality disorder.
Excludes: delusional disorder and schizophrenia.
DSM-5
The American Psychiatric Association‘s DSM-5 has similar criteria for paranoid personality disorder. They require in general the presence of lasting distrust and suspicion of others, interpreting their motives as malevolent, from an early adult age, occurring in a range of situations. Four of seven specific issues must be present, which include different types of suspicions or doubt (such as of being exploited, or that remarks have a subtle threatening meaning), in some cases regarding others in general or specifically friends or partners, and in some cases referring to a response of holding grudges or reacting angrily.[8]
PPD is characterized by a pervasive distrust and suspiciousness of others such that their motives are interpreted as malevolent, beginning by early adulthood and present in a variety of contexts. To qualify for a diagnosis, the patient must meet at least four out of the following criteria:[8]
- Suspects, without sufficient basis, that others are exploiting, harming, or deceiving them.
- Is preoccupied with unjustified doubts about the loyalty or trustworthiness of friends or associates.
- Is reluctant to confide in others because of unwarranted fear that the information will be used maliciously against them.
- Reads hidden demeaning or threatening meanings into benign remarks or events.
- Persistently bears grudges (i.e., is unforgiving of insults, injuries, or slights).
- Perceives attacks on their character or reputation that are not apparent to others and is quick to react angrily or to counterattack.
- Has recurrent suspicions, without justification, regarding fidelity of spouse or sexual partner.
The DSM-5 lists paranoid personality disorder essentially unchanged from the DSM-IV-TR[9] version and lists associated features that describe it in a more quotidian way. These features include suspiciousness, intimacy avoidance, hostility and unusual beliefs/experiences.
Other
Various researchers and clinicians may propose varieties and subsets or dimensions of personality related to the official diagnoses. Psychologist Theodore Millon has proposed five subtypes of paranoid personality:[10]
| Subtype | Features |
|---|---|
| Obdurate paranoid (including compulsive features) | Self-assertive, unyielding, stubborn, steely, implacable, unrelenting, dyspeptic, peevish, and cranky stance; legalistic and self-righteous; discharges previously restrained hostility; renounces self-other conflict. |
| Fanatic paranoid (including narcissistic features) | Grandiose delusions are irrational and flimsy; pretentious, expensive supercilious contempt and arrogance toward others; lost pride reestablished with extravagant claims and fantasies. |
| Querulous paranoid (including negativistic features) | Contentious, caviling, fractious, argumentative, faultfinding, unaccommodating, resentful, choleric, jealous, peevish, sullen, endless wrangles, whiny, waspish, snappish. |
| Insular paranoid (including avoidant features) | Reclusive, self-sequestered, hermitical; self-protectively secluded from omnipresent threats and destructive forces; hypervigilant and defensive against imagined dangers. |
| Malignant paranoid (including sadistic features) | Belligerent, cantankerous, intimidating, vengeful, callous, and tyrannical; hostility vented primarily in fantasy; projects own venomous outlook onto others; persecutory delusions. |
Differential diagnosis
Paranoid personality disorder can involve, in response to stress, very brief psychotic episodes (lasting minutes to hours). The paranoid may also be at greater than average risk of experiencing major depressive disorder, agoraphobia, social anxiety disorder, obsessive-compulsive disorder or alcohol and substance-related disorders. Criteria for other personality disorder diagnoses are commonly also met, such as:[11] schizoid, schizotypal, narcissistic, avoidant, borderline and negativistic personality disorder.
Treatment
Because of reduced levels of trust, there can be challenges in treating PPD. However, psychotherapy, antidepressants, antipsychotics and anti-anxiety medications can play a role when a person is receptive to intervention.[12]
Epidemiology
PPD occurs in about 0.5–2.5% of the general population.[5][11] It is seen in 2–10% of psychiatric outpatients. It is more common in males.[11]
History
See also: History of paranoia
Paranoid personality disorder is listed in DSM-V and was included in all previous versions of the DSM. One of the earliest descriptions of the paranoid personality comes from the French psychiatrist Valentin Magnan who described a “fragile personality” that showed idiosyncratic thinking, hypochondriasis, undue sensitivity, referential thinking and suspiciousness.[13]
Closely related to this description is Emil Kraepelin’s description from 1905 of a pseudo-querulous personality who is “always on the alert to find grievance, but without delusions”, vain, self-absorbed, sensitive, irritable, litigious, obstinate, and living at strife with the world. In 1921, he renamed the condition paranoid personality and described these people as distrustful, feeling unjustly treated and feeling subjected to hostility, interference and oppression. He also observed a contradiction in these personalities: on the one hand, they stubbornly hold on to their unusual ideas, on the other hand, they often accept every piece of gossip as the truth.[13] Kraepelin also noted that paranoid personalities were often present in people who later developed paranoid psychosis. Subsequent writers also considered traits like suspiciousness and hostility to predispose people to developing delusional illnesses, particularly “late paraphrenias” of old age.[14]
Following Kraepelin, Eugen Bleuler described “contentious psychopathy” or “paranoid constitution” as displaying the characteristic triad of suspiciousness, grandiosity and feelings of persecution. He also emphasized that these people’s false assumptions do not attain the form of real delusion.[13]
Ernst Kretschmer emphasized the sensitive inner core of the paranoia-prone personality: they feel shy and inadequate but at the same time they have an attitude of entitlement. They attribute their failures to the machinations of others but secretly to their own inadequacy. They experience constant tension between feelings of self-importance and experiencing the environment as unappreciative and humiliating.[13]
Karl Jaspers, a German phenomenologist, described “self-insecure” personalities who resemble the paranoid personality. According to Jaspers, such people experience inner humiliation, brought about by outside experiences and their interpretations of them. They have an urge to get external confirmation to their self-deprecation and that makes them see insults in the behavior of other people. They suffer from every slight because they seek the real reason for them in themselves. This kind of insecurity leads to overcompensation: compulsive formality, strict social observances and exaggerated displays of assurance.[13]
In 1950, Kurt Schneider described the “fanatic psychopaths” and divided them into two categories: the combative type that is very insistent about his false notions and actively quarrelsome, and the eccentric type that is passive, secretive, vulnerable to esoteric sects but nonetheless suspicious about others.[13]
The descriptions of Leonhard and Sheperd from the sixties describe paranoid people as overvaluing their abilities and attributing their failure to the ill-will of others; they also mention that their interpersonal relations are disturbed and they are in constant conflict with others.[13]
In 1975, Polatin described the paranoid personality as rigid, suspicious, watchful, self-centered and selfish, inwardly hypersensitive but emotionally undemonstrative. However, when there is a difference of opinion, the underlying mistrust, authoritarianism and rage burst through.[13]
In the 1980s, paranoid personality disorder received little attention, and when it did receive it, the focus was on its potential relationship to paranoid schizophrenia. The most significant contribution of this decade comes from Theodore Millon who divided the features of paranoid personality disorder to four categories:[13]
1) behavioral characteristics of vigilance, abrasive irritability and counterattack,
2) complaints indicating oversensitivity, social isolation and mistrust,
3) the dynamics of denying personal insecurities, attributing these to others and self-inflation through grandiose fantasies
4) coping style of detesting dependence and hostile distancing of oneself from others.
See also
- DSM-IV codes (personality disorders)
- ICD-10 codes (personality disorders)
- Delusional disorder
- Delusions of reference
- Paranoid anxiety
- Paranoid schizophrenia
- Persecutory delusions
- Schizotypal personality disorder
References
Waldinger, Robert J. (1 August 1997). Psychiatry for Medical Students. American Psychiatric. ISBN978-0-88048-789-4. Meissner & Kuper, 2008 MacManus, Deirdre; Fahy, Tom (August 2008). “Personality disorders”. Medicine. 36 (8): 436–441. doi:10.1016/j.mpmed.2008.06.001. Kendler KS, Czajkowski N, Tambs K, et al. (2006). “Dimensional representations of DSM-IV cluster A personality disorders in a population-based sample of Norwegian twins: a multivariate study”. Psychological Medicine. 36 (11): 1583–91. doi:10.1017/S0033291706008609. PMID16893481. Personality Disorders at eMedicineAaron T. Beck, Arthur Freeman (1990). Cognitive Therapy of Personality Disorders (1st ed.). The Guilford Press. ISBN9780898624342. OCLC906420553. The Classification of Mental and Behavioural Disorders (ICD-10) by WHO: “Diagnostic guidelinesArchived 2014-03-23 at the Wayback Machine, p.158 “Schizoid Personality Disorder (pp. 652–655)”. Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (2013). ISBN978-0-89042-555-8. American Psychiatric Association (2000). Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition Text Revision (DSM-IV-TR). Washington, DC: American Psychiatric Association. Millon, Théodore; Grossman, Seth (6 August 2004). Personality disorders in modern life. Wiley. ISBN978-0-471-23734-1. “Internet Mental Health — paranoid personality disorder”. Archived from the original on 2013-01-31. Retrieved 2004-06-01. “”Paranoid Personality Disorder” at Cleveland Clinic”. Archived from the original on 2012-03-04. Retrieved 2008-02-13. Salman Akhtar (1990). [https://books.google.de/books?id=bU0eAAAAQBAJ&pg=PA149#v=onepage&q&f=false Paranoid Personality Disorder: A Synthesis of Developmental, Dynamic, and Descriptive Features] Archived 2018-04-01 at the Wayback Machine. American Journal of Psychotherapy, 44, 5–25.
- Bernstein, D. P., Useda, D., Siever, L. J. (1995). Paranoid Personality Disorder. In: J. W. Livesley (Ed.). The DSM-IV Personality Disorders. (pp. 45-57). New York: Guilford.
External links
- National Personality Disorder website for England
- Articles about Personality Disorders in Web4health web site
Johns Hopkins Psychiatrist: Transgender is ‘Mental Disorder;’ Sex Change ‘Biologically Impossible’ Posted September 13th 2019
By Michael W. Chapman | June 2, 2015 | 1:34 PM EDT

Dr. Paul R. McHugh. (Photo:
Johns Hopkins Medicine)
(CNSNews.com) — Dr. Paul R. McHugh, the former psychiatrist-in-chief for Johns Hopkins Hospital and its current Distinguished Service Professor of Psychiatry, said that transgenderism is a “mental disorder” that merits treatment, that sex change is “biologically impossible,” and that people who promote sexual reassignment surgery are collaborating with and promoting a mental disorder.
Dr. McHugh, the author of six books and at least 125 peer-reviewed medical articles, made his remarks in a recent commentary in the Wall Street Journal, where he explained that transgender surgery is not the solution for people who suffer a “disorder of ‘assumption’” – the notion that their maleness or femaleness is different than what nature assigned to them biologically.
He also reported on a new study showing that the suicide rate among transgendered people who had reassignment surgery is 20 times higher than the suicide rate among non-transgender people. Dr. McHugh further noted studies from Vanderbilt University and London’s Portman Clinic of children who had expressed transgender feelings but for whom, over time, 70%-80% “spontaneously lost those feelings.”
While the Obama administration, Hollywood, and major media such as Time magazine promote transgenderism as normal, said Dr. McHugh, these “policy makers and the media are doing no favors either to the public or the transgendered by treating their confusions as a right in need of defending rather than as a mental disorder that deserves understanding, treatment and prevention.”

Time magazine, June 9, 2014,
America’s Next Civil Rights Frontier. (Photo: AP)
“This intensely felt sense of being transgendered constitutes a mental disorder in two respects. The first is that the idea of sex misalignment is simply mistaken – it does not correspond with physical reality. The second is that it can lead to grim psychological outcomes.”
The transgendered person’s disorder, said Dr. McHugh, is in the person’s “assumption” that they are different than the physical reality of their body, their maleness or femaleness, as assigned by nature. It is a disorder similar to a “dangerously thin” person suffering anorexia who looks in the mirror and thinks they are “overweight,” said McHugh.
This assumption, that one’s gender is only in the mind regardless of anatomical reality, has led some transgendered people to push for social acceptance and affirmation of their own subjective “personal truth,” said Dr. McHugh. As a result, some states – California, New Jersey, and Massachusetts – have passed laws barring psychiatrists, “even with parental permission, from striving to restore natural gender feelings to a transgender minor,” he said.
The pro-transgender advocates do not want to know, said McHugh, that studies show between 70% and 80% of children who express transgender feelings “spontaneously lose those feelings” over time. Also, for those who had sexual reassignment surgery, most said they were “satisfied” with the operation “but their subsequent psycho-social adjustments were no better than those who didn’t have the surgery.”
“And so at Hopkins we stopped doing sex-reassignment surgery, since producing a ‘satisfied’ but still troubled patient seemed an inadequate reason for surgically amputating normal organs,” said Dr. McHugh.
The former Johns Hopkins chief of psychiatry also warned against enabling or encouraging certain subgroups of the transgendered, such as young people “susceptible to suggestion from ‘everything is normal’ sex education,” and the schools’ “diversity counselors” who, like “cult leaders,” may “encourage these young people to distance themselves from their families and offer advice on rebutting arguments against having transgender surgery.”
Dr. McHugh also reported that there are “misguided doctors” who, working with very young children who seem to imitate the opposite sex, will administer “puberty-delaying hormones to render later sex-change surgeries less onerous – even though the drugs stunt the children’s growth and risk causing sterility.”
Such action comes “close to child abuse,” said Dr. McHugh, given that close to 80% of those kids will “abandon their confusion and grow naturally into adult life if untreated ….”
“’Sex change’ is biologically impossible,” said McHugh. “People who undergo sex-reassignment surgery do not change from men to women or vice versa. Rather, they become feminized men or masculinized women. Claiming that this is civil-rights matter and encouraging surgical intervention is in reality to collaborate with and promote a mental disorder.”
CNSNews Reader,
The liberal media are terrified of the truth, especially when it leads to uncomfortable questions about their own leftist worldview.
CNS News covers the stories that the liberal media are afraid to touch. It drives the national debate through real, honest journalism — not by misrepresenting or ignoring the facts.
CNSNews relies on the support of our loyal readers to keep providing the news and commentary that matter to the American people, not just stories that prop up the liberal agenda.
Editorial Comment I am not sure the liberal media are terrified of the truth. The best they ever do is twist truth. Their worst is burying it with lies. There are so many factors driving people, especially men, mad that it would be hard to separate cause from effect when it comes to sex change or the more correctly named gender reassignment.
Psychiatry More Dangerous to Individuals than Psychology- September 2019
The antipsychiatry movement: Who and why
Current Psychiatry. 2011 December;10(12):4-53 By Henry A. Nasrallah, MDAuthor and Disclosure Information

Although irritating, antipsychiatry helps keep us honest and rigorous about what we do PDF Download
Psychiatry is the only medical specialty with a longtime nemesis; it’s called “antipsychiatry,” and it has been active for almost 2 centuries. Although psychiatry has evolved into a major scientific and medical discipline, the century-old primitive stage of psychiatric treatments instigated an antagonism toward psychiatry that persists to the present day.
A recent flurry of books critical of psychiatry is evidence of how the antipsychiatry movement is being propagated by journalists and critics whose views of psychiatry are unflattering despite the abundance of scientific advances that are gradually elucidating the causes and treatments of serious mental disorders.
What are the “wrongdoings” of psychiatry that generate the long-standing protests and assaults? The original “sin” of psychiatry appears to be locking up and “abusing” mentally ill patients in asylums, which 2 centuries ago was considered a humane advance to save seriously disabled patients from homelessness, persecution, neglect, victimization, or imprisonment. The deteriorating conditions of “lunatic” asylums in the 19th and 20th centuries were blamed on psychiatry, not the poor funding of such institutions in an era of almost complete ignorance about the medical basis of mental illness. Other perceived misdeeds of psychiatry include:
- Medicalizing madness (contradicting the archaic notion that psychosis is a type of behavior, not an illness)
- Drastic measures to control severe mental illness in the pre-pharmacotherapy era, including excessive use of electroconvulsive therapy (ECT), performing lobotomies, or resecting various body parts
- Use of physical and/or chemical restraints for violent or actively suicidal patients
- Serious or intolerable side effects of some antipsychotic medications
- Labeling slaves’ healthy desire to escape from their masters in the 19th century as an illness (“drapetomania”)
- Regarding psychoanalysis as unscientific and even harmful
- Labeling homosexuality as a mental disorder until American Psychiatric Association members voted it out of DSM-II in 1973
- The arbitrariness of psychiatric diagnoses based on committee-consensus criteria rather than valid and objective scientific evidence and the lack of biomarkers (this is a legitimate complaint but many physiological tests are being developed)
- Psychoactive drugs allegedly are used to control children (antipsychiatry tends to minimize the existence of serious mental illness among children, although childhood physical diseases are readily accepted)
- Psychiatry is a pseudoscience that pathologizes normal variations of human behaviors, thoughts, or emotions
- Psychiatrists are complicit with drug companies and employ drugs of dubious efficacy (eg, antidepressants) or safety (eg, antipsychotics).
Most of the above reasons are exaggerations or attributed to psychiatry during an era of primitive understanding of psychiatric brain disorders. Harmful interventions such as frontal lobotomy—for which its neurosurgeon inventor received the 1949 Nobel Prize in Medicine—were a product of a desperate time when no effective and safe treatments were available. Although regarded as an effective treatment for mood disorders, ECT certainly was abused many decades ago when it was used (without anesthesia) in patients who were unlikely to benefit from it.
David Cooper1 coined the term “antipsychiatry” in 1967. Years before him, Michel Foucault propagated a paradigm shift that regarded delusions not as madness or illness, but as a behavioral variant or an “anomaly of judgment.”2 That antimedicalization movement was supported by the First Church of Christ, Scientist, the legal system, and even the then-new specialty of neurology, plus social workers and “reformers” who criticized mental hospitals for failing to conduct scientific investigations.3
Formerly institutionalized patients such as Clifford Beers4 demanded improvements in shabby state hospital conditions more than a century ago and generated antipsychiatry sentiments in other formerly institutionalized persons. Such antipathy was exacerbated by bizarre psychiatrists such as Henry Cotton at Trenton State Hospital in New Jersey, who advocated that removing various body parts (killing or disfiguring patients) improved mental health.5
Other ardent antipsychiatrists included French playwright and former asylum patient Antonin Artaud in the 1920s and psychoanalysts Jacques Lacan and Erich Fromm, who authored antipsychiatry writings from a “secular-humanistic” viewpoint. ECT use in the 1930s and frontal leucotomy in the 1940s understandably intensified fear toward psychiatric therapies. When antipsychotic medications were discovered in the 1950s (eventually helping to shut down most asylums), these medications’ neurologic side effects (dystonia, akathisia, parkinsonism, and tardive dyskinesia) prompted another outcry by antipsychiatry groups, although there was no better alternative to control psychosis.
In the 1950s, a right-wing antipsychiatry movement regarded psychiatry as “subversive, left-wing, anti-American, and communist” because it deprived individuals of their rights. Psychologist Hans Eysenck rejected psychiatric medical approaches in favor of errors in learning as a cause of mental illness (as if learning is not a neurobiologic event).
The 1960s witnessed a surge of antipsychiatry activities by various groups, including prominent psychiatrists such as R.D. Laing, Theodore Lidz, and Silvano Arieti, all of whom argued that psychosis is “understandable” as a method of coping with a “sick society” or due to “schizophrenogenic parents” who inflict damage on their offspring. Thomas Szasz is a prominent psychiatrist who proclaimed mental illness is a myth.6 I recall shuddering when he spoke at the University of Rochester during my residency, declaring schizophrenia a myth when I had admitted 3 patients with severe, disabling psychosis earlier that day. I summoned the chutzpah to tell him that in my experience haloperidol surely reduced the symptoms of the so-called “myth”! Szasz collaborated with the Church of Scientology to form the Citizens Commission on Human Rights. Interestingly, Christian Scientists and some fundamental Protestants3 agreed with Szasz’s contention that insanity is a moral, not a medical, issue.
Editorial Comment It is noteworthy that psychiatrists find criticism ‘ irritating ‘ rather than worrying. R D Laing called psychologists whores, as in all things to the State who pays them to avoid reality and keep on ‘fuc–ng things up. We have never had so many overtly mad people, and as in the old U.S.S.R, it is a great way for discrediting dissidents. Elites are like that and the masses easily fooled or misled.
[PDF] One Flew Over the Cuckoos Nest by Ken Kesey Book Free Download (325 pages)
Author Ken Kesey | Submitted by: Jane Kivik
Free download or read online One Flew Over the Cuckoos Nest pdf (ePUB) book. The first edition of this novel was published in 1962, and was written by Ken Kesey. The book was published in multiple languages including English language, consists of 325 pages and is available in Mass Market Paperback format. The main characters of this young adult, high school story are Chief Bromden, Randle Patrick McMurphy. The book has been awarded with , and many others.530725 Reviews
Price: N/A Free
Download

Suggested PDF: The Electric Kool-Aid Acid Test by Tom Wolfe pdf
One Flew Over the Cuckoos Nest PDF Details
| Author: | Ken Kesey |
| Original Title: | One Flew Over the Cuckoos Nest |
| Book Format: | Mass Market Paperback |
| Number Of Pages: | 325 pages |
| First Published in: | 1962 |
| Latest Edition: | February 1st 1963 |
| ISBN Number: | 9780451163967 |
| Language: | English |
| Main Characters: | Chief Bromden, Randle Patrick McMurphy, Nurse Ratched, William “Billy” Bibbit, Charles Cheswick |
| category: | young adult, high school, academic, read for school, media tie in, movies, literature, historical, historical fiction, humor, unfinished, american, american classics, medical, classics, seduction |
| Formats: | epub(Android), audible mp3, audiobook and kindle. |
Now available in Spanish, English, Chinese, Russian, Hindi, Bengali, Arabic, Portuguese, Indonesian / Malaysian, French, Japanese, German and many others.
Please note that the tricks or techniques listed in this pdf are either fictional or claimed to work by its creator. We do not guarantee that these techniques will work for you or not.
Some of the techniques listed in One Flew Over the Cuckoos Nest may require a sound knowledge of Hypnosis, users are advised to either leave those sections or must have a basic understanding of the subject before practicing them.
DMCA and Copyright: The book is not hosted on our servers, to remove the file please contact the source url. if you see a Google Drive link instead of source url means that the file witch you will get after approval is just a summary of original book or the file has already been removed.
Related Books
Hot Sometimes a Great Notion by Ken Kesey by Ken Kesey Download Hot The Electric Kool-Aid Acid Test by Tom Wolfe by Tom Wolfe Download Hot The Cuckoos Calling by Robert Galbraith by Robert Galbraith Download Hot The New Answers Book: Over 25 Questions on Creation / Evolution and the Bible by Ken Ham by Ken Ham Download
- Julia Anna – December 02, 2017 Loved each and every part of this book. I will definitely recommend this book to young adult, high school lovers
- John Doe – December 02, 2017 Great book, One Flew Over the Cuckoos Nest pdf is enough to raise the goose bumps alone.
- William Ballard – March 02, 2018 It’s always fun to read Ken Kesey books
Add a review
Why do we want comfort? Belle Smith Posted September 8th 2019

Humans may seek comfort in times of distress because they are left with a feeling of loneliness. They are in need of affection. They need to know that there is somebody there that cares about them and someone that can tell them that everything is going to be okay.
I’ve mentioned that in times of distress, people may feel lonely, I know this because I often feel this way. It can be hard for some people to think positively all the time and have a healthy state of mind. It comes easy for some people, but others really struggle with their mental health.
Please, if you know that somebody feels down or not too good mentally, ask them if they are alright. Don’t just leave them on their own, I know what this feels like. You can never know what they are going through inside their minds. They need some reassurance that everything is going to be alright. It will give them some insight that you care about them.
Take care x
What don’t narcissists want you to know? Carol VeeAnswered Jun 21, 2018 Posted September 8th 2019
That they love headgames. That they are master head fuc*ers and cunning manipulators. That they have dark secrets like porn addiction or other addictions or an attraction to children. I am 6 months out from discarding mine.
I wasnt mean when I told him I was done, but when he hoovered me and told me he still thot about me and cared for me and still wanted to be friends, I made sure to tell him that there was NO chance because I did not and would never trust him because of his lies and porn addiction. He has hoovered me since with phone call hang ups but I hadnt heard anything RECENTLY until yesterday when he called me and I never answer so he left a long voicemail where he was having a conversation with probably a woman…. what he doesnt know is that it was all garbled and I couldnt understand anything… I know he did this because I was behind his car the other day at a stop light and completely ignored him like he doesnt exist for me (which he doesnt)… I thot I might get a hoover after that and I did….I know the phone hang ups are a way to see if I will call him back…… NO WAY EVER. If I did I am sure he would either not answer or say I DIDNT MEAN TO CALL U IT WAS A MISTAKE… I truly believe he sits around and tries to find ways to manipulate and use me….WONT HAPPEN, EVER….78.4k views · View Upvoters · View Sharers
RecommendedAllView 90 other answers to this question
About the Author

Carol Vee
95.8k content views13.6k this month More Answers from Carol VeeWhy do empaths stay with narcissists after they’ve seen all the red flags?309 Views
“A generation of sociopaths”
Nick Hubble September 5th 2018
Ever wanted to know what your children and grandchildren’s generation think of you? Well, here goes… One of the first ‘suggested’ searches when I started to type in ‘The baby boomers…’ into Google was, simply… “The baby boomers ruined everything.” So, I clicked the search. Here are the first page of results:
As you can see, the headlines don’t make for pretty reading. Unfortunately, these kinds of views aren’t unique. Hell, a book was released a couple of years ago about the boomers. Do you know what it was called? “A generation of Sociopaths”. These views are ridiculous. Childish at best. But millions of people around the UK believe, in their hearts, that they’re true. Like it or not, if you’re reading this there’s a high chance you’re one of “The people who stole the world”. Even if you’re actually not.
What is paranoid personality disorder? Posted August 28th 2019
Paranoid personality disorder (PPD) is a type of eccentric personality disorder. An eccentric personality disorder means that the person’s behavior may seem odd or unusual to others. An individual with paranoid personality behavior is very suspicious of other people. They mistrust the motives of others and believe that others want to harm them. Additional hallmarks of this condition include being reluctant to confide in others, bearing grudges, and finding demeaning or threatening subtext in even the most innocent of comments or events. A person with PPD can be quick to feel anger and feel hostile toward others.
PPD usually appears in early adulthood. According to the Cleveland Clinic, PPD appears to be more common in men than women.
Treatment for PPD can be challenging, because people with PPD have intense suspicion and mistrust of others. A mental health professional must establish trust with the patient. This trust enables the patient to confide in the professional and believe that they have a disorder.
Read more: Personality disorder »
What are the causes of paranoid personality disorder?
The cause of paranoid personality disorder is unknown. However, researchers believe that a combination of biological and environmental factors can lead to paranoid personality disorder.
The disorder is present more often in families with a history of schizophrenia and delusional disorders. Early childhood trauma may be a contributing factor.
What are the symptoms of paranoid personality disorder?
Often, people with paranoid personality disorder don’t believe that their behavior is abnormal. It may seem completely rational to a person with PPD to be suspicious of others. However, those around them may believe this distrust is unwarranted and offensive. The person with PPD may behave in a hostile or stubborn manner. They may be sarcastic, which often elicits a hostile response from others, which may seem to confirm their original suspicions.
Someone with PPD may have other conditions that can feed into their PPD. For example, depression and anxiety can affect a person’s mood. Mood changes can make someone with PPD more likely to feel paranoid and isolated.
Other symptoms include:
- believing that others have hidden motives or are out to harm them
- doubting the loyalty of others
- being hypersensitive to criticism
- having trouble working with others
- being quick to become angry and hostile
- becoming detached or socially isolated
- being argumentative and defensive
- having trouble seeing their own problems
- having trouble relaxing
Some symptoms of PPD can be similar to symptoms of other disorders. Schizophrenia and borderline personality disorder are two disorders with symptoms similar to PPD. It can be difficult to clearly diagnose these disorders.
How is paranoid personality disorder diagnosed?
Your primary care provider will ask you about your symptoms and history. They’ll also do a physical evaluation to look for any other medical conditions you may have. Your primary care provider may send you to a psychiatrist, psychologist, or other mental health professional for further testing.
The mental health professional will perform a comprehensive assessment. They may ask about your childhood, school, work, and relationships. They may also ask you how you would respond to an imagined situation. This is to gauge how you might react to certain situations. The mental health professional will then make a diagnosis and form a treatment plan.
Read more: Types of mental health professionals »
How is paranoid personality disorder treated?
Treatment for PPD can be very successful. However, most individuals with this condition have trouble accepting treatment. Someone with PPD doesn’t see their symptoms as unwarranted. If an individual is willing to accept treatment, talk therapy or psychotherapy are helpful. These methods will:
- help the individual learn how to cope with the disorder
- learn how to communicate with others in social situations
- help reduce feelings of paranoia
Medications can also be helpful, especially if the person with PPD has other related conditions such as depression or anxiety disorder. Medications may include:
- antidepressants
- benzodiazepines
- antipsychotics
Combining medication with talk therapy or psychotherapy can be very successful.
What is the long-term outlook?
The outlook depends on whether the individual is willing to accept treatment. Individuals who accept treatment can hold down a job and maintain healthy relationships. However, they must continue treatment throughout their lifetime, because there’s no cure for PPD. Symptoms of PPD will continue, but can be managed with care and support.
People with PPD who resist treatment may lead less functional lives. PPD may interfere with their ability to hold down a job or have positive social interactions.
Keep reading: What do you want to know about mental health? »
3 sourcescollapsedHealthline has strict sourcing guidelines and relies on
Editorial Comment Perhaps the most crucial line in this piece is where it says the causes are unknown. The basic differnece between pyschiatry and psychology is that the former is a specialism for quaified doctors in medicine and the latter argue that odd behaviour is an outcome of trauma.
These days there is a view in medicine that trauma and other significant events can change a persons DNA, so diagnosis moves back into the realms of medicine. Whatever, the whole business is based on guesswork.
So we have the latest nonsense that the rising number of anxiety cases is caused by women being exposed to stressful situations during pregnancy. With no reference to sources, this pacifying propoganda was all over BBC Radio 4 last week. Robert Cook September 8th 2019
How do narcissists apologize?Margherita Veronese, Expert in personality disorders Answered Aug 17
A pathological narcissist never apologizes.
Often the narcissist’s victim develops new belief systems or fantasies. These fantasies in some ways help the victim to deal with the emotional pain that comes with the break up in the short-term. But in the long term, they keep you as the victim locked up in the negative cycle of narcissistic abuse even after the narcissist has left.
The first of this fantasy is that the narcissist will admit to his mistakes and acknowledge the pain that he has caused you. The reason this is a fantasy is that if this were true, then the person in question will not be a narcissist.
Another destructive belief after the narcissist has left is that your suffering will break the narcissist and will make him realize what he has done to you. Again, remember that one of the hallmark features of narcissism is their lack of empathy, and if this belief could be a reality, then the person you are dealing with is not a narcissist. If your suffering could break him, if you could activate some semblance of empathy, humanity, or remorse, then the person in question does not have NPD. Although this can give you a level of comfort, in the longer term it is going to put you in more pain because it is divergent from reality. So, you can think of these beliefs as some form of magical thinking.
The pathological untreated narcissist is like a biological machine driven by a blind impulse. He has grown up without developing a personality; instead of a person, multiple psychic functions work only if they receive emotional energy from the outside. This is why the narcissist regards others as an extension of himself. Without the relationship with the victim, his psyche disintegrates. He creates a web of tormented relationships and intrigues that he needs to survive, causing emotional reactions on his victims.
If the narcissist apologizes he is lying and is manipulating you.
Surely trauma bonding is another great issue for you. Trauma bonding is one of the reasons people continue to stay in abusive relationships. It is being loyal to a person who is destructive, abusive, and exploitative. It is a subconscious survival strategy and a way of coping with prolonged, severe, and repetitive abuse. It is quite similar to Stockholm’s Syndrome where a hostage bonds with their captor during captivity.
Narcissists, psychopaths, borderline narcissists or whatever spectrum the abuser falls in all go through cycles of abusing and that confuses the victim even further. This is often why it is difficult for victims to leave abusive relationships even if they know that they are in a toxic relationship. The narcissist will reward your good behavior. Therefore, if you are obedient and compliant, he will idealize you. He might tell you how amazing you are and how much he treasures you in his life. He might even randomly do things that he does not usually do. For instance, he might buy a gift or do chores which he never does. Therefore, you may end up feeling a sense of relief, hope, and temporary happiness. Then suddenly, he tells you that you are worthless, stupid, and can’t get anything right, and he makes you feel betrayed and neglected. This way, he fosters an emotional dependency and wants to control your emotional state.
If you correctly process your experience, understanding that you are dealing with a very strong pathological personality and evaluating your mistakes (due to inexperience) you can finally get out of it.
To do this, dialogue with a therapist is necessary. You can start by developing your experience, informing yourself about the dynamics of the narcissistic relationship by reading books, but surely the advice of a professional is required.
The narcissist cannot change, but his victim can change. I recommend this new book that explains the narcissistic way of thinking and strategies to deal with a real narcissist but most of all it helps the victims of narcissists change themselves, their mindset and lifestyle, to get rid of these toxic relationships.
Download the Audio Book Version of This Book for FREE
Just by Signing Up for a FREE 30-Day Audible Trial!
Click one link below to get started!
For Audible US Search for:
Recent Posts
Recent Comments
Archives
Categories
Copyright 2020 | MH Newsdesk lite by MH Themes
